Talking about animal culls
| name: | William D. Hueston, DVM, Ph.D. | |
| Field: | Director, Center for Animal Health and Food Safety, University of Minnesota | |
| Date: | December 7, 2006 | |
| Email: | huest001@umn.edu | |
| Location: | Minnesota, U.S. |
Comment:
I’m pulling together an article on the risk communication challenges of our current policies of mass animal destruction as response to exotic animal disease introductions – those piles of burning cattle carcasses in the U.K., trenches full of pigs in Taiwan or tens of thousands of gassed birds in Southeast Asia.…
Any suggestions?
Peter responds:
A few quick thoughts re mass animal destruction:

- It’s crucial to acknowledge the yuck factor. Disgust is a close cousin of dread and a well-established component of what I call outrage. And disgust is a nearly universal reaction to mass animal destruction. (It’s a common reaction to normal slaughtering methods too, for that matter.) People’s response to their own disgust is likely to be bimodal: (a) “If you've got to do something that disgusting, it must be really serious!” or (b) “It can’t be right to do something that disgusting – you must be overreacting!” In many cases it would be wisest to ally with (a) – that is, to use disgust at your precaution as evidence of the seriousness of the risk. “Things are so bad we feel we have no choice but to….” Sometimes you need to disavow both (a) and (b), which is harder: “I know this may seem like a very extreme response to a fairly routine outbreak. The photos are so gross! Even I have trouble looking, and I’ve been working on animal health for decades. But this is actually Standard Operating Procedure for situations of this sort….” What’s never wise is to ignore people’s disgust and act as if that weren't our reaction.

- It’s important to acknowledge that some people question the ethics of mass animal destruction altogether. Animal rights groups rarely encounter a more responsive public than when they oppose these sorts of culls. Those managing the culls should try to acknowledge the existence of opponents even before the opponents show themselves. “The bottom line is that we’re killing animals in order to [protect human health] [prevent the spread of an infectious animal disease] [both]. We’re even killing healthy animals in order to stop the chain of contagion. The science that says this is the most effective way to stop the outbreak is extremely strong. But of course we never, ever use this strategy with humans, and there are some who believe that animals should have much the same rights as humans – including the right not be sacrificed this way for the greater good. We do it anyway – but with real sorrow, real awareness of what we are doing, and real respect for the beliefs of those who think we shouldn’t do it.” (There’s a seesaw at work here. The more respectful the authorities are of the views of animal rights advocates, the likelier the rest of us are to decide, albeit reluctantly, that other priorities must come first.)

- Actions that appear callous or disrespectful should be avoided if possible – photos reminiscent of concentration camps; use of bulldozers; macabre humor on the part of those administering the cull; etc. If they can’t be avoided they should be acknowledged. “I know this looks awfully callous. It was necessary, but it feels so wrong!” Get on the other side of that seesaw too.

-
A narrower point that’s extremely important right now vis-à-vis bird flu and H5N1-related bird culls: Don’t pretend that what you’re doing is in the farmer’s interest when it isn’t. My wife Jody Lanard and I have done some work (Jody more than I) with international agencies and Asian governments wishing to encourage farmers to cooperate with culls. They often try to claim that an H5N1 outbreak is a serious threat to the health of the farmer and his family. This is simply false. Bird-to-human transmission of H5N1 remains difficult; only a few hundred cases have cropped up in the face of millions of opportunities. Interacting with sick birds is nowhere near as dangerous to the farmer as losing his livelihood. And of course there is no “business case” whatever for a farmer whose birds are healthy to destroy his own livelihood in order to create a cordon sanitaire and stop the spread of infection. That’s wise for the world at large, for reasons of poultry industry prosperity as well as pandemic prevention. But it is surely a net loss – a catastrophe, in fact – for the farmer, his family, and his village. We have advised clients to say exactly that. (It’s not a secret; claims to the contrary are transparently false.) Of course what makes most sense is for the developed world to subsidize compensation to developing world farmers, whose sacrifice helps to protect us all. If compensation isn’t in the cards, there are two other options: appeals to altruism and coercion. Dishonest claims that the farmer ought to want to cull his flock undermine altruism and add insult to the injury of coercion.
That’s what comes immediately to mind. I'll look forward to seeing your article.
Risk communication and the legitimacy of counterterrorism
| name: | Rusty Cawley | |
| Field: | Public Affairs Counsel, The Integrative Center for Homeland Security, Texas A&M University | |
| Date: | November 30, 2006 | |
| Email: | rcawley@vprmail.tamu.edu | |
| Location: | Texas, U.S. |
Comment:
In our first issue of “Public Citizen,” our director Dr. David H. McIntyre compares the American approach to counterterrorism with the Australian approach. While editing this document, I was struck by the following paragraph:
When counterterrorism works, it appears excessive and unnecessary. The need for counterterrorism measures is only apparent when they fail. This is a perpetual strategic dilemma that demonstrates why LEGITIMACY is the key issue in all terrorism/counterterrorism efforts. Counterterrorism can only succeed when the people have faith in their government. In fact, promoting government legitimacy is the only strategically decisive goal of counterterrorism. The goal of terrorism is to destroy that bond, not just to kill people or destroy infrastructure. This is hard for even experts to understand, and harder still for them to articulate.
Am I wrong or does this sound like a risk communications challenge?
Peter responds:
This is beautifully said. And I agree: It’s a risk communication challenge.
In fact, Dr. McIntyre’s entire short article framed a risk communication challenge – the challenge of reconciling the threat of violent Islamism with the organizing “narrative” of Western thought (especially, I think, the West’s self-image).
A step in the right direction (the step Dr. McIntyre seems to be trying to take) is dilemma-sharing. We need to be saying much more explicitly that we see an extraordinary conflict between our vision of how differing religions should share the world and our understanding of how to meet the Islamist terrorist threat. We need to say that we’re having enormous trouble reconciling the two. We need to explain – mostly to ourselves – how painful it is to choose between entertaining a much more illiberal vision and denying ourselves some pretty important weapons against Islamist attack.
At least one thing wrong with the Pope’s speech in Regensburg (cited by Dr. McIntyre) was his failure to express any sense of the painful dilemma that might require reinstating the “old narrative” he was advancing. He sounded, perhaps accurately, like the old narrative had always been his preferred narrative, and would have been his preferred narrative even if Islamist terrorism had not become a force to reckon with.
I think President Bush’s advocacy of various civil liberties infringements has been similarly deficient. He certainly leaves me feeling that he doesn’t see the dilemma – that he is quite comfortable abandoning these liberties in order to fight Islamism more effectively, perhaps even that fighting Islamism is merely an excuse for doing what he’d have wanted to do anyway.
Our answer to the question, “Should we grant liberal freedoms to those who deny the validity of those freedoms and would not grant them to us if in charge?” has almost always been a resounding “Yes!” That answer is relatively low-cost when liberal values are securely in charge. Can we still afford to give the same answer? We can’t sensibly address that question unless we acknowledge both that the price seems to be higher than it was and that it may nonetheless be a price worth paying.
We need a debate that starts with consensus about a few points:
- We cherish our liberal “narrative” – our sense of ourselves as essentially tolerant – and are rightly extremely reluctant to give it up.
- That narrative may now be getting in the way of repelling the threat of violent Islamism.
- The crucial question is whether we should move to a new narrative; or whether we must address the Islamist threat handicapped by our deeply felt values; or whether we can somehow forge a compromise or a short-term exception.
- The debate over how best to answer this question is deeply divisive internally, but that debate must nonetheless take place. Those who don’t see some truth and some virtue on both sides of the debate – who don’t see that there is a painful dilemma here – will be little help in finding a resolution.
- This is not an entirely new situation. We had a similar debate with respect to our battle with Communism, for example, though religion was not then at the core. Part of our debate should be about what lessons to draw from history.
It’s going to take more than good risk communication to address this dilemma effectively. But it’s certainly going to take good risk communication.
The role of outrage in regulatory reform
| name: | Bruce Hugman | |
| Field: | Communications consultant | |
| Date: | November 24, 2006 | |
| Email: | mail@brucehugman.net | |
| Location: | Thailand |
Comment:
I just came across this reference in my weekly English newspaper, and was rather encouraged by first impressions: http://www.brc.gov.uk/news/2006/061018.asp.
It appears to suggest an access of good sense before the U.K. goes the way of countries like Sweden, where, in some respects, the population have lost their edge because of over-protection by government and regulation. There is considerable discussion of risk and how it should be managed and who should take responsibility for it – including the radical suggestion that citizens might well be able to deal with more than anxious politicians want to let them.
What do you think? I still visit your website and continue to value your wisdom!
Peter responds:
Thank you for the link to the U.K.’s Better Regulation Commission (BRC) news release announcing its report: “Risk, Responsibility, Regulation: Whose Risk Is It Anyway?” I knew this was coming, but I didn’t know it had arrived. Having just browsed the full report ![]() , I agree with you that it represents real progress. I especially liked the short case studies, annotated in terms of the questions they raise.
, I agree with you that it represents real progress. I especially liked the short case studies, annotated in terms of the questions they raise.
I do think the report would have benefited from some risk communication expertise – especially a better understanding of the reality that people don’t (and in my judgment shouldn’t) judge risks purely in terms of what I call the “hazard.” People’s choices about which risks to try to mitigate are always going to be responsive to “outrage” as well as “hazard.”
In my terms, the BRC wants to reduce regulatory attention to low-hazard high-outrage risks. This is possible, I think, only if the outrage is well-managed. When outrage is ignored and allowed to build, the pressure to over-regulate hazard builds right along with it. Over-regulating a small hazard doesn’t actually mitigate the outrage much; an outrage problem needs an outrage solution. (For a long disquisition on this complicated issue, see “Because People Are Concerned: How Should Public Outrage Affect Application of the Precautionary Principle?”. ![]() ) But ignoring a big outrage because it’s a small hazard isn’t a solution either.
) But ignoring a big outrage because it’s a small hazard isn’t a solution either.
The problem of our over-regulation of low-hazard high-outrage risks is very different from the “nanny state” problem – which stems mostly from “over-regulation” of high-hazard low-outrage risks, especially those that are voluntary and pleasurable.
New York City, for example, recently proposed outlawing the use of transfats in restaurants. The data that transfats contribute importantly to mortality are pretty unassailable, I think. But so are the data that transfats taste good; the data that many people, given the choice, will take the risk; and the data that those who wish to avoid transfats are able to do so already without further regulation.
I certainly agree with the BRC that encouraging people to make their own risk management decisions is an important piece of progress. But it won’t necessarily make regulations more cost-effective with regard to lives saved per unit of cost (or per unit of bureaucratic interference). If those are the right metrics, the New York City transfat regulation is probably sound.
In other words, I think the BRC report would be a better guide to regulatory reform if it distinguished more carefully the two key problems it addresses:
- Public demand for a governmental response to low-hazard high-outrage risks – which is a misuse of resources insofar as it doesn’t significantly reduce hazard (and may actually increase hazard), but which addresses a public mandate that is genuine and understandable.
- Regulatory inclination to interfere in people’s lives by regulating voluntary behavior that incurs significant hazard, but does so without significant public outrage (indeed, the public may be outraged mostly at the regulation itself).
Of course the lowest-hanging fruit is the over-regulation of low-hazard low-outrage risks – where bureaucrats run amok and do something that addresses neither a serious hazard nor a serious outrage. An example in the BRC report: a regulation requiring people to remove doormats from their entryways because of a hypothetical tripping risk.
But once you’ve gotten rid of such totally useless regulations, you’re left with two real policy dilemmas: what to do when people are really upset about a tiny threat to their health, and what to do when people are perfectly happy to endanger themselves seriously.
Lessons of the O.J. Simpson / Rupert Murdoch /
Judith Regan controversy
| name: | Brian | |
| Field: | Health care public affairs professional | |
| Date: | November 24, 2006 | |
| Location: | New York City, U.S. |
Comment:
I have a curious request, and I’ll understand 100% if you decline. But here goes.
If you were writing a memo to Rupert Murdoch in the wake of the O.J. Simpson book/TV special controversy, what communications recommendations would you give for both Rupert and News Corp. moving forward?
Peter responds:
I have followed this only peripherally – it was hard to miss! – but I have to admit the outrage at the scheduled book and shows surprised me. I’d have expected most people to feel something closer to vindication. (“See, he was guilty, just as I said all along.”) I’d have predicted some outrage at the legal system for having no way to retry Simpson for murder, and maybe some outrage at Simpson for still being coy rather than contrite, and certainly lots of demand to make sure the victims’ families and victim advocacy organizations benefited from it all.
But the outrage at News Corp. for its role in the deal, and the insistence that it back out, surprised me.
Though it surprised me, the outrage certainly didn’t offend me – as any attempt at government censorship would have, or as a violent response like the response to the Muhammad cartoons would have. It’s not “censorship” for people to react to a publication they dislike by shunning and shaming those involved, and thus costing them reputation and profitability. And I approve of corporate “self-censorship” in response to public outrage. That’s exactly how the system is supposed to work. When stakeholders disapprove of something a company has decided to do, the company gets to choose whether to do it anyway and endure the costs of the disapproval or to defer to its stakeholders’ values and change its decision. Of course the choice is tougher when stakeholders disagree with each other, or when management’s strongly felt values are in conflict with the mood of the society. On occasion there are good reasons not to be responsive to public outrage. I don’t believe the O.J. Simpson controversy is such an occasion.
Obviously, I wouldn’t have been canny enough to advise News Corp. to steer away from the deal. I would have advised the company that the deal would certainly make it look pretty cheesy, willing to profit from just about anything that’s not illegal. And I’d have advised it to acknowledge that this was so, and to have arrangements in place (or at least offers on the record) from the outset to share their profits with victims’ organizations and the specific victims’ families. But I wouldn’t have known to warn that the deal would probably cost News Corp. more money than it would make.
As the outrage built, I certainly would have advised Judith Regan not to disavow the financial motives for her involvement in the project. I could believe she saw the book as a sort-of confession; I could even swallow her rhetoric about “closure.” But I couldn’t buy that she wasn’t interested in the money too, or that she saw the project as a way of healing victims of domestic violence everywhere.
And I would have urged Rupert Murdoch attribute his decision to pull the plug on the project more to the public’s outrage and less to his own (belated) outrage. I suppose it’s possible Murdoch wasn’t paying attention to what Regan was up to until people started revealing how disgusted they were. But to me this smacks of the childish way companies typically react to being forced by others to do something they don’t want to do. Like a six-year-old forced to clean her room, companies imagine the consolation prize is that they get to pretend it’s voluntary: “I’m not cleaning my room because you made me. I’m cleaning my room because I want to!” When you’re bowing to pressure, it’s more honest, more gracious, and ultimately more profitable to say so.
What advice would I give now that the furor is pretty much over? The main thing, I think, is to keep mentioning it in the months ahead, maybe even the years ahead – however long it takes until the public (not the company’s management) is sick of hearing about it. In the aftermath of a bad mistake, people want to know that you know it was a bad mistake. They want to know that you feel chastened and have learned some lessons. That may mean announcing some changes in company policy or personnel. It may mean putting a retrospective on the incident in the company’s annual report. The next time the company decides not to move forward on some project because it could be offensive, it would be wise to say so, and to point out specifically that it doesn’t want to make again the mistake it made with O.J. Simpson.
And the next time the company decides to move forward on a project that some could find offensive, it should certainly mention Simpson before its critics do, explaining that it thought long and hard before deciding to go ahead anyway … and why it sees this situation as different from the Simpson situation.
Defining risk: Why not include benefits too?
| Name: | Ray Pena |
| Field: | Emergency manager |
| Date: | November 24, 2006 |
| Email: | gouiuray1@yahoo.com |
| Location: | Virginia, U.S. |
Comment:
Risk = the possibility of gain + the possibility of loss.
If risk is only the possibility of loss, then why would anyone ever take a risk? I think risk is more than the possibility of loss. Risk is the possibility of gain plus the possibility of loss. We take the risk because we believe the possible gain exceeds the possible loss.
If the possible gain exceeds the possible loss, the risk is positive and more likely to be taken. If the possible loss exceeds the possible gain, the risk is negative and less likely to be taken.
Positive Risk = the possibility of reward > the possibility of loss.
Negative Risk = the possibility of loss > the possibility of reward.
Peter responds:
Many different occupations – from medicine to insurance to emergency management – consider “risk” a key concept. Each has its own definition. Or, rather, each has its own definitions; often there is plenty of definitional disagreement even within an occupation.
But I think for most people “risk” is about bad outcomes. In some definitions the risk is the bad outcome itself. In some definitions it’s the probability of the bad outcome (how likely it is), or the magnitude of the bad outcome (how bad it is). In quantitative risk assessment it’s the probability multiplied by the magnitude.
I don’t know of an occupation that routinely includes good outcomes in what it means by risk. People who invest money in a highly speculative stock, for example, don’t normally say it isn’t very risky because the potential gain is so high. They say it’s worth the risk because the potential gain is so high.
You’re certainly right that we judge the wisdom of taking a particular risk by balancing the probability and magnitude of bad outcomes against the probability and magnitude of good outcomes. But we don’t usually include the good outcomes in our definition of the risk itself.
That said, there is a profound sense in which you’re right and the conventional definitions are wrong.
People define risk in terms of bad outcomes and then try to balance risks (and costs) against benefits to reach a decision. That’s what we mean to do. But empirical studies of actual decision-making show that very often that’s not what we actually do. Instead, we systematically misperceive high-risk high-benefit situations. If we’re focused on the risk side, we underestimate the benefits. If we’re focused on the benefit side, we underestimate the risks.
For obvious reasons, advocates of specific outcomes do this in their rhetoric. Supporters of nuclear power tend to claim the risks are lower than they really are, while anti-nuke activists tend to claim the benefits are lower than they really are. But endless evidence says ordinary people accomplish a similar distortion in their private thoughts.
Here’s why. It’s hard to balance risks against benefits – not just intellectually hard, but emotionally hard. The act of balancing forces us to recognize that we can’t have it all, that we have to choose between giving up on benefits we covet and bearing risks we fear. We avoid the discomfort of a tough choice by misperceiving one of the two factors, telling ourselves either that the benefits aren’t really all that terrific or that the risks aren’t really all that horrific. We think we’re balancing risks against benefits. We keep them distinct in our definitions. And then we muddle them in our perceptions in order to make tough decisions feel easier.
This risk-versus-benefit confusion is one of three such confusions that play crucial roles in risk perception … and therefore in risk management and risk communication. The other two:
- The magnitude-versus-probability confusion. It is very hard for people to perceive high-magnitude low-probability risks correctly. It’s uncomfortable to notice that a risk is really horrible (so take precautions) but really unlikely (so shrug it off). We tend to make the problem go away by either underestimating risk magnitude or overestimating risk probability. See my column on “Worst Case Scenarios.”
- The hazard-versus-outrage confusion. Decades ago, I proposed redefining the word “risk” so it includes not only the probability and magnitude of bad outcomes (which I want to call “hazard”) but also the factors like control, trust, dread, and familiarity that make a risk upsetting (which I call “outrage”). Whether you like my definitions or not, the evidence is clear that outrage has a huge impact on hazard perception. A risk that is really upsetting is likely to be seen as very dangerous, whether it is or not. But if a risk doesn’t have the characteristics that make it upsetting, it’s hard to notice that it’s dangerous.
Unlike the other two, this hazard-versus-outrage muddle isn’t symmetrical. Hazard doesn’t lead people to misperceive outrage. But outrage routinely leads people to misperceive hazard. Whether we think a risk is dangerous depends systematically on whether it’s upsetting – that is, on whether it’s controlled by others, managed in untrustworthy ways, dreaded, unfamiliar, etc. For more on my “Risk = Hazard + Outrage” concept, start with “Risk Communication: Facing Public Outrage,” and then look at some of the articles listed in my Outrage Management Index.
My effort to untangle the hazard-versus-outrage muddle led me to propose including what I call outrage in the definition of risk. So I can’t say you’re way off base wanting to include benefits in the definition of risk. You’re going against the tide, but so was I.
However we decide to define “risk,” what matters is that we stay alert to these three distinctions: (a) Hazard versus outrage; (b) Magnitude versus probability; and (c) Benefit versus risk (or, if you win your battle, “positive risk” versus “negative risk”).
Why it’s hard to persuade people to add pandemics to the long list of things they’re worried about
| name: | Margot White, J.D. | |
| Field: | Public health and human rights professor | |
| Date: | November 18, 2006 | |
| Email: | MLWhite@salud.unm.edu | |
| Location: | New Mexico, U.S. |
Comment:
Having only taken up the issue of pandemic influenza a year ago, my search for wisdom regarding risk communication led me immediately to your articles. I have benefited greatly from them and thank you for your precision and breadth.
From my background in medical ethics, law, and human rights, I have plunged into pandemic issues to bring the “preparedness” rubric to the public, to local communities. This is extremely important. However, I have discovered significant cultural, political, social barriers to this that I want to share with you in the hope that you might have some insight or wisdom to offer.
First of all, we live in a time when fear-mongering has been rampant and people’s capacity for additional threat perception is extremely – and justifiably – limited. There is what I call “Y2K syndrome” (a hugely over-hyped allegation of dire disruptions that never materialized) as well as “phantom menace syndrome” (the politically motivated scare tactics surrounding supposed disease threats from smallpox and anthrax – neither of which ever materialized and never truly existed anyway). Among those who do pay attention to the news media, therefore, there is justified skepticism about this new disease threat. Once the global context for this is introduced, they can generally be persuaded – but bringing people out to a town hall on pandemic influenza is a challenge in itself!
Given the general lack of education in this country with respect to how the U.S. connects with the rest of the world, there is the additional barrier of ignorance regarding globalization, recent worldwide changes in agricultural practices, the nature of viruses, the ecology of infectious diseases, etc. Even among clinicians, there is an astonishing lack of awareness of the context for disease outbreaks or the relationship between globalization and infectious diseases, or human rights and the spread of diseases throughout the world.
In addition to these barriers, we have ongoing cultural distractions ranging from sports to sitcoms and an Orwellian public discourse that has turned off most intelligent observers and utterly confused everyone else. Trying to bring complex fact patterns to an exhausted middle class is proving extremely difficult. (Forget those at or below the poverty level – the recommendation to “wash hands” and “stockpile food” is so grossly wide of the mark that it borders on the grotesque.)
Meanwhile, for whatever reason (turkey-consuming holidays? editorial fatigue?), our own national media outlets are noticeably “ho-hum” about avian influenza outbreaks ongoing in Asia, or the ongoing threat to humans by simple processes of evolution and ecology.
The concept of “planning” and preparedness, moreover, is flawed at its core. It is disconnected from local conditions, and offers generic “all hazard” mantras about “incident command” and “first responders” that bear no relation to the actual dimensions of a pandemic disease process. The public is simply left out of all of this. How are they supposed to develop the capacity to stay home for a month when their jobs are not secure? How will they obtain extra supplies of insulin for their diabetic child when insurance companies won’t pay the cost?
Why isn’t anyone in a leadership position addressing these issues? These are the risks that no one seems to be communicating – the risks of an exhausted public, a brainwashed and misled population that is both undereducated and overstimulated and can no longer distinguish the real from the fabricated, the authentic from the artificial, news from entertainment, real threats from politically motivated fear-mongering.
Any suggestions?
Peter responds:
I hear your frustration loud and clear. I often feel much the same frustration. And yet there has been progress.
- There is now a cohort of “pandemic fanatics” that didn’t exist a few years ago – people who are following the issues, preparing their households, and harassing their neighbors and employers. If a pandemic comes, they will be ready to lead.
- Public awareness in the mainstream has improved. In fact, it has improved so much that we have a new reason for frustration when there’s a lull (as there is right now) and it appears to be slipping.
- Civil society is taking notice. More and more companies, even small ones, are beginning the process of developing their own pandemic plans. So are many hospitals (at last!), schools, and soup kitchens. The ones that haven’t started yet are at least thinking maybe they should.
- Realism is taking hold. News stories (though scarcer) are showing more clarity about the distinction between bird flu in birds and pandemic flu in humans. Government pronouncements contain less knee-jerk over-reassurance. There is a better balance between medical preparedness and infrastructure preparedness.
Alerting a complex society to a risk it hasn’t previously focused on much is a slog. It was a slog for those who came before us too – those who pushed for wider acceptance of hardhats or seatbelts or vaccinations; those who are still pushing for wider acceptance of radon testing or carbon monoxide monitoring. Progress isn’t guaranteed; sometimes society shrugs off a risk and refuses to take precautions. What’s guaranteed is that progress, if it comes, comes slowly. If and when a severe pandemic materializes, of course, people will climb the learning curve very, very quickly. Getting people to climb the learning curve beforehand can save lives and reduce suffering. We can only hope there’s sufficient time, and keep slogging.
Several of the barriers you raise deserve discussion.

Has people’s ability to respond to the pandemic threat been undermined by their exposure to too many other threats?
It is certainly true that fear arousal is a competition. Jerry Falwell wants people to be more afraid of gay marriage; Greenpeace wants people to be more afraid of genetically modified foods; you and I want people to be more afraid of a pandemic. People have only so much fearfulness to allocate. And people have only so much time, energy, and money for precautions. So our success must come at the expense of Falwell, Greenpeace, and the advocates of awareness and precaution-taking with respect to thousands of other risks.
This understanding can greatly ameliorate officials’ widespread “fear of fear.” When we try to frighten people into pandemic preparedness, we are not turning them into more frightened people; we’re just competing for our slice of the fearfulness pie.
What isn’t true, I think, is that people are more threatened – or feel more threatened – than in the past. It’s pretty obvious that most people don’t face greater actual risks than their grandparents; if anything, we face fewer and less dangerous risks than they faced, freeing us to obsess over threats that didn’t make the cut for them. Nor do I believe that people are more bewildered or more overwhelmed than their grandparents were by the panoply of risks they face, and thus less able to take a new risk onboard. It has always been difficult to persuade people to take a new risk onboard before it was imminent and obvious. And those trying to do the persuading have probably always imagined that the task must have been easier in past generations.

Have people become so skeptical about all those phantom threats that it is harder and harder to warn them about a real threat?
I love your phrase “phantom menace syndrome.” And I think you’re probably right that people are more skeptical than they used to be, more aware that the current scare of the week may not turn out to be such a big deal after all.
But I see very little persuasive evidence that this skepticism translates into any kind of immunity. Sophisticated skepticism (even cynicism) seems to coexist with vulnerability. People know that you and I and Jerry Falwell and Greenpeace are all trying to arouse them to action against one or another risk. They know they shouldn’t take our word for it. They know that some of the risks they’re being warned against probably are phantoms, and some of the people doing the warning probably have hidden agendas. They may know all this more clearly than their grandparents knew it. But like their grandparents, they have a quantum of fearfulness to allocate. And like their grandparents, they keep on reallocating, ignoring some new candidates for their attention and taking others onboard.
It’s interesting to read in your comment the oscillation between these two concerns. Are people so overwhelmed by so many threats that they can’t think straight about how dangerous pandemics really are? Or are people so disenchanted with all those efforts to frighten them that they can no longer take pandemic warnings or any warnings seriously? Neither, I think – at least no more so than their grandparents.

Have “politically motivated scare tactics” and indiscriminate fear-mongering undermined the legitimacy of our efforts to frighten people?
I encounter this objection a lot when I urge clients to be more willing to frighten people into pandemic preparedness. Some point out that Hitler mobilized fear to justify the Holocaust. Others point out that President Bush mobilized fear to justify the invasion of Iraq. (I am not suggesting that these are equivalent sins.) How can it be right for us to do the same thing to justify pandemic precautions?
In the final analysis, ethics are personal, and I would never urge a client to do something that felt unethical to that client. But for myself, at least, I see fear-arousal as an ethically neutral tool – good when deployed on behalf of good goals and evil when deployed on behalf of evil goals. (I’d add that it may be evil even when deployed on behalf of good goals if it’s deployed hypocritically; whatever you’re trying to accomplish, you should think twice before frightening people about something you don’t actually consider scary.)
The term “fear-mongering,” of course, begs the issue. We apply the term only when we believe that a particular effort to frighten people is illegitimate. We all agree it applies to Hitler’s rants against Jews and others. Opponents of the war in Iraq would apply it to President Bush’s warnings that Saddam Hussein might have Weapons of Mass Destruction. It sounds like you’d probably be comfortable applying it to Y2K, smallpox, and anthrax warnings. I’m inclined to apply it to Falwell’s and Greenpeace’s warnings. Industry applies it to activist anti-pollution campaigns. Anti-pollution activists apply it to industry efforts to warn about job loss and economic stagnation. Lots of people apply it to our efforts on behalf of pandemic preparedness.
The most effective way we know to motivate preparedness and precautions is to frighten people. Excessive fear is immobilizing, of course, but so is insufficient fear – and insufficient fear is by far the more common of the two problems. If we think pandemics are worth preparing for, we ought to want to arouse some proportionate fear about pandemics. I see no reason to be deterred by the fact that other communicators are working to arouse fear about other issues in ways we consider disproportionate.

Is ignorance a major barrier to pandemic precaution advocacy?
Yes and no. There are certainly a lot of things we need people to know about pandemics and pandemic preparedness.
But the relationship among information, attitudes, and behavior isn’t what we usually imagine. Educators are particularly prone to assume that the relationship looks like this:
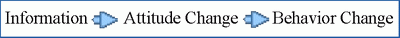
But Leon Festinger’s “cognitive dissonance theory” established some 50 years ago that behavior change usually comes first, often motivated by fear or other emotions. Then people seek out information to justify the new behavior and thus reduce the “cognitive dissonance.” Finally, they evolve attitudes that integrate the new information, stabilizing the new behavior. Thus:

(You may want to look at a book chapter
 by Brian A. Day and Martha C. Monroe that describes my approach to these issues in greater detail.)
by Brian A. Day and Martha C. Monroe that describes my approach to these issues in greater detail.)
Is the concept of planning “flawed at its core”?
I agree with you fervently that planning that doesn’t involve the public is flawed at its core. People don’t necessarily have a perfect understanding of how they are likely to respond to a particular threat or a particular recommended precaution. But their understanding of their own likely responses is hugely better than the understanding of professional planners. So unless we consult with them as we plan, our plans are pretty close to useless. (Collaborative planning has other advantages as well – among them that people are likelier to trust and comply with a plan they helped develop.) As you point out, the discontinuities between planners’ expectations and people’s actual responses are greatest when the planners are planning for people most unlike themselves – for poor people and ethnic minorities, for example.
For a landmark study demonstrating these realities for two case studies, a smallpox attack and a dirty bomb attack, see the “Redefining Readiness”
 report by Roz Lasker and others at the New York Academy of Medicine.
report by Roz Lasker and others at the New York Academy of Medicine. I’m not sure whether I agree with you that the “all hazards” approach is flawed at its core. I do see lots of differences between pandemics and other sorts of emergencies – but I also see the inefficiency, maybe even the futility, of preparing independently for an endless list of possible scenarios. Ideally, we would pursue all-hazards preparedness as far as it can take us, and then would focus real attention on what’s unique about the hazards that worry us most.
Certainly one of the most important things about a pandemic is that people, families, and neighborhoods would be forced to rely largely on their own resources, rather than waiting to be helped by governments. That’s not unique to pandemics, but it certainly distinguishes pandemics from many other kinds of emergencies. It makes citizen involvement in pandemic planning all the more important. And it makes the “incident command” concept all the more peripheral.
Margot responds:
You are right, of course, about the “cognitive dissonance” insights. My collaborations with infectious disease experts over the years brought this into focus repeatedly.
It is, I think, a healthy response to the current political climate to be wary of assertions that “we” (the public) should be ready to trade off our civil liberties in the face of vague and unspecified threats to our “security.” The challenge is to provide accurate and up-to-date factual information that differentiates the pandemic from other kinds of threats. I agree with you that realistic fear is an appropriate and necessary motivator.
Finally, about the “incident command structure” – it seems unlikely that this decision-making and coordinating rubric will have much to offer after a couple of weeks of a pandemic, much less a couple of months or years. My concern is that the overall responsibility, having been handed to homeland security agencies rather than health-related agencies, may too easily become militarized.
In all of this, the core focus needs to be public awareness and engagement at some level of the preparedness process. Without knowing the extraordinary dimensions of a pandemic, both in time and in geographic reach, people will not grasp what they need to do that is different from preparing for floods or fires. In this sense, the “all hazards” approach is inadequate, even for first responders.
Peter responds:
You are worried that emergency response agencies and their traditional preoccupation with command structure will lead to a militarization of pandemic response, and to a resulting insensitivity to human rights issues. This strikes me as a legitimate worry.
I have been worried that when health departments are in charge of pandemic preparedness, they tend to focus on a fairly mild pandemic paradigm – because in a mild pandemic (like 1957 and 1968) the main issues really are medical issues: hospital surge capacity, ventilator sufficiency, antiviral supply, etc. In a severe pandemic (like 1918), on the other hand, the main issues are likely to be infrastructure survival: energy supply, food supply, water supply, and the like. These non-medical concerns tend to get more attention when pandemic planning is in the hands of emergency response agencies.
We’re best off, obviously, when both sorts of departments have a hand in pandemic planning – along with human rights experts, risk communication experts, a wide range of other sorts of experts, and, above all, normal people whose chief expertise is the sort of ordinary self-knowledge we experts tend to lack.
Aren’t the outrage factors just aspects of risk perception?
| name: | Jennifer Vazquez | |
| Field: | MD/MPH student | |
| Date: | October 29, 2006 | |
| Email: | vazqueje@umdnj.edu | |
| Location: | New Jersey, U.S. |
Comment:
I was wondering if you could explain the difference between the components of outrage and risk perception factors.
It seems to me that there are similarities between the two, and based on your Risk = Hazard + Outrage equation, that the outrage components would influence risk perception.
I would appreciate it if you could clarify this for me.
Peter responds:
You are absolutely right that many people refer to what I call outrage components as aspects of risk perception.
I try to steer away from the perception formulation because it leads so easily to the view that people are making a mistake when they take voluntariness, control, trust, and the rest seriously. “Perception” gets interpreted as “misperception” – and the lesson seems to be that clear thinkers should avoid contaminating their judgments about risk with all this extraneous psychological chaff.
In my formulation, “outrage” and “hazard” are both part of what risk means. A situation is thus riskier if it’s less under your control (for example), every bit as much as it is riskier if it’s likelier to kill you. If I make the situation less deadly, I’m making your risk smaller. If I give you some control, I’m also making your risk smaller.
So where does perception fit in? Outrage has a huge impact on hazard perception – a bigger impact, in fact, than hazard has. If I give you more control over the situation, you are likely to perceive the hazard as smaller, even though the hazard hasn’t actually changed.
But even though outrage greatly influences hazard perception, it’s a mistake to think they’re the same thing. How much control you have is how much control you have. How likely you are to get killed is how likely you are to get killed. (Both have to be perceived, by the way; perception is the only means humans have for inputting data.) So yes, how much control you think you have will affect (that is, distort) how endangered you think you are. But independent of its effect on your hazard perception, how much control you think you have will directly affect how serious you consider the risk. And that part isn’t a distortion or a misperception at all. It’s part of what people mean when they talk about a risk being big or small, serious or trivial.
Think about a controversy over a factory’s emissions of dimethylmeatloaf. Narrow the controversy to two issues: the dose-response curve of dimethylmeatloaf for pancreatic cancer (a traditional hazard issue) and the frequency with which the plant manager has misled the neighborhood about how much dimethylmeatloaf is emitted (a traditional outrage issue). Notice three truths:
- We “know” the dose-response curve and the integrity of the plant manager only through perception. We may perceive these two variables accurately or inaccurately. We probably have better data on the integrity of the plant manager.
- If the plant manager has been consistently candid, we are likelier to see the dose-response curve as fairly benign. If the plant manager has been dishonest, on the other hand, we are likelier to suppose that the dimethylmeatloaf must be really dangerous.
- Even though the plant manager’s integrity affects our perception of the dose-response curve, they’re not the same thing. If we discover that dimethylmeatloaf cannot cause pancreatic cancer – thus correcting a misperception – we will nonetheless continue to consider it a serious risk to live near a factory with a dishonest management.
Pandemic flu good communication example file
| name: | Jody Lanard, M.D. | |
| Field: | Short-term consultant, international health agency | |
| Date: | October 29, 2006 | |
| Location: | Philippines |
Comment:
Crfullmoon sent you the link to the Flu Wiki's “Pandemic Flu Misinformation Hall of Shame.”
Equally useful, or perhaps even more useful, would be a “Pandemic Flu Good Communication Example File.” In my experience teaching risk communication, people seem to perk up when I tell them “good example stories” – it gives them hope that it is possible to learn strategies for doing a better job.
The first training exercise that seems to give my workshop “students” hope is when they practice converting over-reassuring statements into reassuring but cautionary statements. Here is a typical “before” and “after” for such a makeover:
| Before: “The outbreak is under control.” |
After: “Even though it looks like the outbreak is under control, we are not relaxing our surveillance, and we urge people to continue taking the recommended precautions for a little while longer.” |
Then we go on to harder strategies.
I'll try to prime the pump on this when I get back from my current posting in the Philippines, but maybe someone on the Flu Wiki will get it started sooner than that!
Peter responds:
For readers who don’t know, Jody Lanard is my wife and colleague – a psychiatrist turned risk communication consultant. She is currently winding up a five-week assignment in the Philippines. She often helps respond to Guestbook entries; this is the first time she has written one.
I fervently agree that good examples are at least as powerful a learning tool as bad examples. So a repository of good pandemic news stories (good reporting and good sourcing) would be really useful – especially if it were annotated to explain what makes it good. For a comparable annotation of a wonderful pandemic speech given in May 2005 by Australian Health Minister Tony Abbott, see “Superb Flu Pandemic Risk Communication: A Role Model from Australia.”
Risk communication and corporate social responsibility
| Name: | Robert Stroehle |
| Field: | Corporate communications (freelance) |
| Date: | October 29, 2006 |
| Location: | Germany (but currently working in Beijing, China) |
Comment:
I first wanted to thank you for your very informative website on risk communications. In my research on the web I have seen a lot of people talking about this, but your conclusions seem very clear to me.
I am a student of political sciences and social psychology in Frankfurt/Main Germany. Right now I am doing an internship in a German company in Beijing, China for three months. In Frankfurt I worked with Edelman as a freelancer for the last year during my studies, focusing on crisis communications.
Have you written any paper on the relationship between CSR [corporate social responsibility] and crisis communications, risk communications, and risk management? Or could you tell me any author that has written on this relationship?
I would like to write my diploma on this topic, focused on the Chinese market. (Actually there is a relevant crisis in China right now, the SK2 scandal, involving some shampoo that contained toxics.)
I think the relationship exists and a good CSR management could keep customers from ruining a company’s reputation. Do you see this as I do?
Peter responds:
I haven’t done a lot of writing on the relationship between risk communication (or crisis communication) and CSR. I agree with you that it’s a fruitful relationship to explore.
I have written on what I see as one of the key differences: Whereas CSR is preoccupied with “responsibility,” risk communication is much more interested in “responsiveness.” See “Responsible or Responsive?” for a dialogue I had with John Elkington of SustainAbility on this distinction. I feel even more strongly about this distinction today than I did when this exchange took place. I don’t much want corporate CEOs deciding what’s good for the world. I want the world deciding, in an ideological free-for-all in which CEOs play no greater role than the rest of us. And then I want CEOs knuckling under to what the world has decided, because that’s the path of profitability and survival for their companies.
I also comment routinely, though not usually in writing, on the distinction between trying to do good/look good on the one hand and trying to avoid doing evil/looking evil on the other hand. I am convinced that the latter plays a much more important role than the former in corporate reputation and profitability; the former is, of course, at least as central to CSR people. There is a transcript on the Web of a presentation I gave at a 2004 corporate responsibility conference run by the Boston College Center for Corporate Citizenship. The very beginning of the transcript addresses this distinction between the ways of improving a company’s reputation: trying to be loved more (which is central to CSR) versus trying to be hated less (which is at the core of the outrage management side of risk communication).
Neither of these distinctions, of course, means that risk communication and CSR are antithetical. They are allied. But they are far from identical, I think!
Pandemic flu misinformation “Hall of Shame”
| name: | crfullmoon | |
| Field: | Flu Wiki fan | |
| Date: | October 23, 2006 | |
| Location: | U.S. |
What I would add to this site:
More guidance for local authorities to be proactive with communicating pandemic preparedness to their citizens, now?
Comment:
Greetings, and thanks to you and your partner for all your excellent work.
I didn’t know if you had seen this thread yet. It has some interesting examples: http://www.fluwikie2.com/pmwiki.php?n=Forum.PandemicFluMisinformationHallOfShame
Peter responds:
Thank you for the link, which I am delighted to pass on. I never know whether to be amused or discouraged by examples of bad pandemic communication. But collecting and thinking about these examples of pandemic flu misinformation is a worthwhile task. I hope Flu Wiki forum participants keep the thread going.
Jody (my wife/partner Jody Lanard) and I have our own collection, to which we keep adding. The errors fall into distinct categories:
- Confusion of bird flu with pandemic flu (as if a pandemic were going to reach “here” via sick birds rather than sick people)
- Over-optimism about local preparedness (as if mass inoculation drills were going to help when there’s nothing yet to put into the syringes)
- Excessive focus on medical issues (as if overstretched hospitals were going to be our biggest problem and we didn’t need to worry about a pandemic’s impact on supply lines, infrastructure, and where our food and energy would come from)
- Insufficient mobilization of public involvement and public preparedness (as if governments could do the job themselves, and as if people would necessarily comply with government pandemic plans they hadn’t helped write)
- Confusion of current risk with potential risk (as if the fact that H5N1 has infected very few people so far meant that it’s silly to start worrying until after the virus learns efficient human-to-human transmission)
And so forth. Maybe someone will use the Flu Wiki list to develop a typology of kinds of pandemic misinformation.
I don’t blame journalists for pandemic misinformation in the media as much as I blame their sources. There are only a handful of “pandemic flu reporters” in the world — science or medical writers who have become really expert on this particular story. Most science and medical writers know surprisingly little about the pandemic risk, and of course general assignment reporters know far less.
It is useful to teach journalists more about pandemics. (I will be participating in a December conference at Harvard University that will try.) But teaching pandemic experts more about how to talk to journalists will probably help more. And more crucial than either is teaching local health officers and public health professionals — the principal local news sources and the principal local pandemic planners — more about the realities of pandemic preparedness.
When I see a piece of misinformation in the media, I often can’t tell if the source got it wrong, or if the source explained it badly so the reporter got it wrong. Either way, I believe better sourcing is a higher priority than better reporting. But I’ll settle for either, and work for both.
Risk communication in facility siting controversies
| name: | Wayne | |
| Field: | Engineer | |
| Date: | October 22, 2006 | |
| Location: | Illinois, U.S. |
Comment:
I was referred to your site by an environmental firm that is doing work for me.
I have read with interest a number of your case studies, but have a specific interest in your perspective on how to deal with communities when a new/controversial industry may be coming to their community.
There is a tactic to tell the locals as little as possible, but I was always taught that properly informing the public – answering their questions as opposed to being evasive – leads to much more trust. It’s just human nature.
Thank you in advance for any comments and/or previous writings you can direct me to that deal with heavy industry introduction to new communities.
Peter responds:
As you know from browsing the website, I’m a strong supporter of candor, in siting a controversial facility as in all risk communication.
There’s no question that telling the locals as little as possible makes the siting process move faster in its early stages. But the price is high: When the community finally learns what you’re up to, people’s suspicions about the wisdom of tolerating the facility are validated by your failure to deal straight with them. So after an efficient, secretive start the siting process typically grinds to a halt.
There are two reasons why it’s smarter to have your public debate early rather than late. First, the debate can focus on the pros and cons of the facility, rather than the disingenuous process you used to get it sited – so it’s a fairer, less hostile debate. And second, you get to find out what you’re up against sooner; it’s not really in your interests to proceed blithely for years before you learn that you may not be able to get your facility sited after all.
The counterargument is that there’s not much opponents can do about a fait accompli. So supporters of secret siting say that the further along you are before the locals know enough to try to stop you, the likelier you are to be able to succeed over their objections. This may have made some sense in years past, and may still make some sense in the developing world (unfortunately). But public involvement is now a settled feature of LULU siting in western countries. (“LULU” is a wonderful acronym invented by Frank Popper: “locally unwanted land use.”) You probably can’t get all the way through the siting process without facing the music – so getting three-quarters of the way through it isn’t very smart. And even if you can sustain your secrecy strategy long enough that it’s no longer practical for opponents to make you change course, do you really want to operate a facility whose neighbors will remember and resent for decades that you snuck in when their backs were turned?
For more on this timing issue – though not in the siting context – see “When to Release Risk Information: Early – But Expect Criticism Anyway.”
Three other pointers on risk communication aspects of siting an industrial facility:

In addition to letting the cat out of the bag early in the siting process, do so with appropriate emphasis on the downsides of the facility you are proposing to build.
Presumably you have a case to make that community benefits outweigh community costs and risks. Make your case. But don’t just talk about the benefits. Concede the costs and risks. Better yet, announce them before opponents have a chance to do so. Acknowledge that the burden of proof is on you to show that the community stands to gain more than it loses. Then meet that burden of proof. And work hard to do something for the people – there are usually at least a few – for whom the benefits genuinely don’t outweigh the costs and risks.
In talking about these risk-benefit tradeoffs, moreover, pay more attention to what you’re doing to mitigate the risks than to how great the benefits are. Even though people do tolerate more risk when they have more to gain, they don’t like thinking in terms of tradeoffs. When benefits get higher, we are inclined to see risks as lower – not just more acceptable, but actually lower. So make sure people know about the benefits, and then talk mostly about what you can do to keep the risks low.

Go beyond candor to responsiveness and accountability.
It’s certainly a good start to design a proposal whose community benefits genuinely outweigh its community costs and risks, and then to communicate promptly and straightforwardly about your proposal. But that’s no longer always enough. In addition, your new neighbors are likely to want some say in the design of the facility. They’d rather you came to them with a rough draft and a lot of options to discuss; not unlike your senior management, they want to see their own handiwork in the final product. Benefits and precautions that they have demanded and secured from you are a lot more reassuring than benefits and precautions you offered them from the get-go.
And your new neighbors are likely to want some oversight as well. They’ll want to be able to check for themselves that the facility’s benefits, risks, and costs are what you say they are. I’m working with a client right now that offers to negotiate a formal contract with each community in which the company wants to put a factory. The contract outlines enforceable commitments – including what happens if something goes wrong: how the community will be able to tell and what recourse it will have.

Make sure you’re asking, not telling. And if possible, consider a bunch of communities at once.
The facility siting process that is least likely to succeed is the one governments often use for really controversial facilities. They spend years delineating complex criteria for finding the “best” site for their facility. Then they crank through a site selection process and come up with a single target site. Then, having clearly established in everyone’s mind that the facility is so incredibly dangerous that only the very safest site on the continent will do, they shake their heads in wonderment when the targeted community isn’t wildly enthusiastic about having won this particular lottery.
Ideally, facility siting should be voluntary on both sides. The community should feel like it has a right to say no, and should initially be asked to say maybe, not yes. And the community should know that your company is looking at other options too. “We have identified several possible sites that could work well for us. We’re exploring each of them, looking for a community that thinks hosting our facility will work well for our neighbors too. Let’s sit down together and figure out if we’re a good match for each other.”
For more on risk communication aspects of facility siting, see:
Is emergency preparedness getting too much attention?
| name: | Lisa Pogoff | |
| Field: | Health department emergency preparedness planner | |
| Date: | October 22, 2006 | |
| Location: | Minnesota, U.S. |
Comment:
In an October 2006 article in Medscape Public Health & Prevention, Dr. Joshua Lipsman argues that we are spending far too much effort and money on public health emergency preparedness. More lives could be saved, he suggests, if we focused more on the leading causes of death and less on preparedness for bioterrorism, natural disasters, epidemics, and the like.
The article’s title says it all: “Disaster Preparedness: Ending the Exceptionalism.” Here’s an excerpt:
Even with the inaccuracies in public health spending figures, these numbers suggest that between 6% and 8% of all annual public health expenditures go toward public health emergency-preparedness efforts. The … numbers also raise the question as to whether this level of expenditure is necessary. If we follow McGinnis and Foege’s exhortation to focus on “those factors that represent the root determinants of death and disability,” we are spending too much on public health emergency preparedness – that is, an amount not proportionate to the impact of public health emergencies on health.
What are your thoughts on this article?
Peter responds:
Dr. Lipsman points out that all U.S. catastrophic deaths from September 11, 2001 to the present – including not only 9/11 itself but also Katrina – add up to fewer than 5,000. “Even if these deaths had all occurred in the same year,” he says, “they still would represent less than one half of 1% of all preventable deaths annually. We should not be spending 6% to 8% of public health dollars on preparing for problems that cause only a fraction of 1% of deaths, if that.”
I have worked with a lot of health departments that fervently agree. Many times in recent years I have been brought to a state or local health department to give a seminar on crisis communication. Almost always, federal money paid for the seminar – usually terrorism or bioterrorism money, sometimes pandemic preparedness money. Almost always, most of my audience would have rather spent the money (and their time) on less hypothetical, more imminent health threats.
It’s worth noting that a national or global health catastrophe like the 1918 flu pandemic could alter the statistics significantly. Horrific though they were, 9/11 and Katrina were health disasters only locally. National preparedness for a possible local catastrophe is likely to fail Dr. Lipsman’s cost-effectiveness test. Preparedness for a possible national or international catastrophe has a sounder economic rationale. Nobody knows the probability of another severe influenza pandemic like 1918’s, but given its very high magnitude, it doesn’t have to be all that probable to be worth getting ready for.
Still, Dr. Lipsman is almost certainly statistically in the right. On a dollar-for-dollar basis, disaster preparedness saves fewer lives than going after the main U.S. sources of preventable death would save.
Of course if economic efficiency is the criterion, going after the main U.S. sources of preventable death isn’t much of a bargain either. The least expensive way to save lives is by fighting hunger, poverty, and chronic infectious diseases in the developing world.
The real flaw in Dr. Lipsman’s argument is that nobody (probably including Dr. Lipsman himself) really wants to focus on the least expensive way to save lives.
What are the risks Dr. Lipsman wants to address with money now squandered on preparing for pandemics, natural disasters, and terrorist attacks? He lists them for us. Roughly 800,000 Americans, he says, die annually from smoking, eating too much, and exercising too little. Alcohol kills another 85,000. The remaining biggies: endemic microbial diseases like flu, pneumonia, and tuberculosis; pollution; motor vehicles; firearms; sexual behavior; and illicit drug use.
It’s interesting that Dr. Lipsman puts pollution on his list, because my corporate clients frequently make the same argument about pollution that he is making about disaster preparedness. They complain that factory emissions (for example) are orders of magnitude less deadly than smoking a cigarette and not wearing your seatbelt on your way to a meeting to talk about factory emissions. They’re statistically in the right too.
What they (and Dr. Lipsman) are missing is that living next door to a polluting factory and being attacked by terrorists are both higher-outrage risks than smoking, overeating, and the rest. People don’t prioritize risks according to how cost-effective they are to avert. We prioritize risks according to how upset they make us feel.
This isn’t just a fundamental risk perception principle – though it is that. It is also a fundamental human value. The risk perception part is that upsetting risks are likely to be perceived as more dangerous than they really are, while risks that aren’t very upsetting are perceived as less dangerous than they really are. Understanding that is essential to risk communication. But equally essential is understanding that even when the misperception is corrected, people still hang onto their preference for spending more to mitigate high-outrage risks than low-outrage risks. That’s the part that’s about human values.
I sometimes tell my clients this hypothetical story:
Imagine that every ten years or so a sniper climbs up onto an overpass with a high-powered rifle and shoots and kills a passing motorist. Then he’s good for another decade. Finally, after 30 years and three deaths, he is caught and brought to trial. Here’s his defense: “During the 30 years during which I shot and killed three passing motorists, thousands of people died on our nation’s highways as a result of drunk driving, not wearing their seatbelts, poor highway design, and poor automotive design. Sniping is an infinitesimal part of the highway death toll. In picking on me, a mere sniper, the government is distorting the public’s understanding of the real priorities of highway safety. The money the government is spending catching me, trying me, and imprisoning me could save far more lives if the government made the rational risk management decision to let me continue killing a mere one person per decade, and reallocated the money to repainting the lane markers on highways.”
Like Dr. Lipsman, my hypothetical sniper is right on the data. Nonetheless, no jury would vote to acquit. Even after they study the data, normal people support spending more money per life saved catching and punishing snipers than repainting lane markers.
Two outrage components are especially relevant to disaster preparedness versus smoking, obesity, exercise, and the like: chronic versus catastrophic risk, and voluntary versus coerced risk. A number of other components – moral relevance, dread, familiarity, etc. – also come into play, but let me focus on the two main ones.
First, and most directly relevant, is the distinction between chronic and catastrophic risk. Consider these examples:
- Driving is more dangerous than flying in terms of deaths per passenger mile. But airline crashes are occasional catastrophes, which makes them a source of considerable anxiety (and media interest). Car crashes are routine, and therefore much easier to shrug off.
- Nuclear power is statistically safer than fossil fuel power. Like a severe pandemic, a major nuclear disaster could alter the statistical picture. But even without a major disaster, the hypothetical risk of a catastrophic nuclear accident generates a lot more outrage than the actual but much more diffuse deaths attributable to burning oil and coal.
- Smoking kills roughly 400,000 American a year. Imagine that they all had to die on November 13 in Chicago. On November 14, we would outlaw smoking. But they die spread out over the year, and spread out over the country, in the privacy of their pain. That’s much more acceptable – much lower-outrage.
As with my sniping example, the greater outrage that society attaches to catastrophic as opposed to chronic risk isn’t just a perceptual distortion. When individuals die, the social fabric is relatively undamaged; we bury the dead, we comfort the bereaved, and life goes on. Recovery is much harder when disaster strikes a community – or a country. Disasters rip the social fabric in ways that individual deaths simply don’t. Our willingness to “overspend” on disaster preparedness embeds not just misperception of the statistical risk, but also wisdom about how societies work.
In fact, you can make a pretty good case that we spend too little on disaster preparedness. There are two normal reactions to a high-magnitude low-probability risk – that is, a possible catastrophe. Either we imagine its probability to be higher than it really is, and therefore over-prepare (at least as judged by the cost-effectiveness criterion). Or we go into denial, imagine the probability to be zero, and therefore feel fine about not preparing at all. In response to 9/11 and Katrina, we may be doing a bit more of the former than usual. But we are still doing plenty of the latter. Look at the statistics on how many local hospitals (not to mention power plants, water treatment facilities, and families) have done next-to-nothing to get ready for a possible pandemic. Look at the unpopularity of flood insurance, even though it is subsidized by the federal government. Ask yourself why the levees in New Orleans were inadequate, why so many people didn’t evacuate, why so few brought food with them to the Superdome.
Preparedness is always something of a tough sell, because it’s so emotionally unsatisfying. Preparedness assumes a bad thing may well happen and works to reduce its consequences. By contrast, prevention assumes there are ways to keep it from happening. Both in individual psychology and in political sociology, prevention is much more attractive. We will pay more than it’s worth to take a risk off the table entirely, and less than it’s worth to reduce the damage. The late Aaron Wildavsky argued persuasively that too much of the national safety budget went to prevention and too little to preparedness. A society that focuses too much on preventing disasters, he also argued, will lack resiliency when forced to cope with one it couldn’t prevent. (For more on these issues, see my column on “Worst Case Scenarios.”)
The other outrage component that Dr. Lipsman's article brings to mind is the voluntary-versus-coerced distinction. Most of the risks on Dr. Lipsman’s list are voluntary risks. People choose to smoke, overeat, and live sedentary lives. And the vast majority of Americans who smoke, overeat, or live sedentary lives do so in spite of knowing it’s bad for them.
Leave aside the question of how effective medical intervention – or any intervention – can be in changing the behavior of people who already know better but have so far been unable or unwilling to change. Assume that a dollar spent on smoking cessation clinics will do more good than a dollar spent on bioterrorism early warning systems. This important question remains: Isn’t it more important to protect people from evildoers than from themselves?
Terrorists, like snipers, strike fear into our hearts in ways that our own bad habits cannot match. Once again, this isn’t just a misperception of the statistical risk. Most people know they are unlikely to die in a terrorist attack. Their main worry is that others will die, and they will have to watch it on television, explain it to their children, and go on living in the more miserable world a terrorist attack creates. Overspending on terrorism preparedness isn’t irrational. Neither is a judgment that we don’t want to do everything possible to deter people from their dangerous bad habits. Maybe this is selfishness, a reluctance to expend tax money on other people’s foolishness. Maybe it is tolerance, respect for the life choices of others, and a disinclination to become more of a nanny state than we already are.
Of course natural disasters and infectious disease pandemics aren’t intentional acts of evil. But they aren’t voluntary either. They’re in the middle. And so they generate an intermediate level of outrage, and thus of willingness to prepare.
The bottom line for me: Dr. Lipsman is probably right that we are spending more per life saved on preparing for public health disasters than on persuading people to quit smoking, eat less, and exercise more. But there are reasons why we make this choice. Those reasons are debatable, and worth debating. Cost-effectiveness statistics should be part of the debate, but the statistics shouldn’t be allowed to preempt the debate. Fortunately, given how fundamental outrage is to our psychological makeup and our societal values, there is no real risk of that happening.
Putting extremists on a Community Advisory Panel
| name: | Theresa | |
| Field: | Public consultation consultant | |
| Date: | October 10, 2006 | |
| Location: | Arizona, U.S. |
Comment:
I’m putting together a Community Advisory Panel (CAP) for a facility with a drug-testing lab. As you can imagine, PETA [People for the Ethical Treatment of Animals] is their biggest opponent.
Like you, I am a strong believer in having all points of view, even the strongest opponents, on the CAP. However, I’m getting a lot of pushback about having the PETA-backed opposition group involved. Is there ever a time where an opponent is so radical there is no benefit to involving them?
Peter responds:
In 1971, U.S. President Lyndon B. Johnson said of FBI Director J. Edgar Hoover, “It’s probably better to have him inside the tent pissing out, than outside the tent pissing in.”
It’s not that putting a PETA-backed activist group on your CAP is necessarily a benefit. Let’s assume that having a media-savvy extremist animal rights organization anywhere in the vicinity isn’t your client’s cup of tea. But it’s not up to your client whether the PETA affiliate is in the vicinity; that’s up to the PETA affiliate. All your client gets to decide is whether it would rather have the group attending its CAP meetings or protesting its CAP meetings. Given that limited choice, Lyndon Johnson’s advice is on target.
Of course a PETA affiliate may very well decline any invitation to join an advisory panel for a lab that tests drugs on animals. In fact, I’d say it will probably decline. But it’s hard to tell for sure. Almost invariably, an activist group has two sets of constituencies. Its radical stakeholders – key volunteers, for example – are likely to take offense if the group “compromises itself” by giving courteous advice to the enemy. They want it to stay pure and embattled. But moderate stakeholders – including large numbers of small-money donors – may want to see it settle for half a loaf, accomplishing something concrete even at the expense of purity.
PETA is certainly aware of this dynamic. It knows its leaders and foot soldiers are predominantly animal rights extremists while its financial contributors are mostly animal welfare moderates. It deliberately decides when to zig and when to zag. But it doesn’t aspire to become the World Wildlife Fund or the Humane Society. Opportunities to cement its radical image are usually more tempting than opportunities to soften that image.
Whether or not the local group accepts your invitation to join the CAP, issuing the invitation is in your client’s interests. It’s not in the group’s interests. If the group’s leaders can con the lab into excluding them, they get a free ride: They don’t have to choose between offending their left wing by accepting and offending their right wing by declining. They can stay comfortably outside demanding to be let in. They can make up pretty much any story they want about what probably went on at meetings they weren’t allowed to attend. They can ask archly what the lab is afraid they might find out.
Although your client is better off issuing an invitation that’s declined than not issuing one at all, it is even better off if its invitation is accepted. Among the many reasons why this is so: It’s much harder for activists to invent dastardly deeds to accuse lab management of perpetrating if they have undisputed access to the real evidence. (Of course if the real evidence is pretty dastardly, your client’s options are much less attractive. I’m assuming the lab is already taking animal welfare seriously.)
Another good reason to hope the group says yes is the opportunity to build a record of accountability. Even a well-run animal testing laboratory needs to ratchet up its animal welfare policies periodically. Paradoxically, improvements that opponents have demanded yield more outrage reduction than improvements that the lab has instituted unilaterally. So it’s handy to have a PETA surrogate in the room pushing the envelope.
And a third reason for wanting the group on the CAP: It will do wonders for the demeanor and demands of more moderate groups. If the PETA allies aren’t present, the moderates who are present will feel some pressure to stand in for them, to show you and show the world that they’re no patsies. But if the PETA allies are there and vocal, the moderates may well feel a different sort of pressure: Pressure to show that “we’re not like them.” In one pretty common CAP dynamic, the extremists kill a lot of the group’s time with repetitive off-the-wall accusations. Other CAP members are rolling their eyes. The company, however, continues to take the group’s claims very, very seriously. If your CAP follows this scenario, the lab could end up allied with the PETA affiliate on behalf of the importance of not muzzling anybody. The extremism of the PETA people and the responsiveness of the lab people combine to make everyone else on the CAP that much more fervently moderate.
Of course there are downsides. For one thing, the CAP will accomplish less with extremists on board. I’m guessing that concrete accomplishments are less important to your client than providing a venue where anti-lab outrage can be safely vented and accommodated – but it’s still important to make sure there are some real accomplishments. Another disadvantage: The CAP will be potentially more fragile. Moderates may get frustrated at the lack of concrete progress and quit … or just stop coming. Or the extremists themselves may realize that their presence is helping the lab’s cause more than their own, and look for a pretext to quit in protest.
Still, on balance the lab has more to gain than to lose by getting the PETA allies there and keeping them there. So it should look for ways to make its invitation easier for a PETA-backed group to accept, and harder or costlier to decline.
For example, I remember working with a cement company that was seeking permits to burn certain types of waste in its cement kiln, essentially turning the kiln into an incinerator. After painful reflection, it decided to invite a local Greenpeace affiliate to join its CAP. The group initially declined, on the grounds that it opposed all incinerators and wasn’t about to give up its opposition. My client said something like this:
Of course not! We’re not asking you to stop opposing incinerators. We assume you’ll oppose ours, and we certainly aren’t making support for our incinerator a condition for sitting on our CAP. But it’s possible the incinerator will be approved despite your opposition. If that happens, you would certainly want to make sure it’s as safe as an incinerator can be. So we’re asking you to pursue two parallel tracks. Work to stop the incinerator – and just in case you fail, work to push us to make sure we design, build, and operate the safest incinerator possible. Given how deeply concerned you are about incinerator safety, how could you do any less?
The company’s invitation to the Greenpeace affiliate led to a succession of private negotiations and public appeals. Eventually, the group decided it couldn’t afford to look insincere about incinerator safety, and it reluctantly joined the CAP. The company never got the permit. But at least the Greenpeace affiliate was inside the tent pissing out.
Talking about “high-path” and “low-path” avian flu
| name: | Leah Bucco-White | |
| Field: | State government information officer | |
| Date: | September 30, 2006 | |
| Email: | leah.buccowhite@hhss.ne.gov | |
| Location: | Nebraska, U.S. |
Comment:
I’m curious about your thoughts regarding the use of high-path/low-path terminology when talking about bird flu.
We’re a public health agency working on bird flu news release templates. We know “bird” experts use the high-path/low-path terminology. But do those terms necessarily mean something to the everyday person?
We don’t necessarily see low-path H5N1 as new news, but it does need to be addressed as birds continue to test positive in the U.S. When bird flu is affecting birds, distinguishing between the two is useful. But what we’re truly concerned about is the bad one. If bird flu affects people (not talking pandemic), the high-path/low-path description becomes a moot point because we’re only talking high-path.
So what about using “deadly bird flu” to describe high-path? Would that make things more meaningful to the public without having to go into all the low-path versus high-path explanations? Then what would you call low-path? Or would this confuse people even more?
Peter responds:
The science in a nutshell:

- There are lots of different strains of bird flu, just as there are lots of different strains of human flu.

- Categorized in terms of ability to inflict harm on poultry, bird flu comes in two “strengths.” “High-pathogenic avian influenza” (often abbreviated as HPAI) can be deadly to poultry. “Low-pathogenic avian influenza” (LPAI) causes very mild symptoms in poultry, or sometimes no observable symptoms at all.

- Some bird flu strains – not all – have been found in both HPAI and LPAI versions. This is true of the H5N1 strain that is currently getting so much attention.

- The bird flu strain that is currently devastating some bird populations, that has managed to spread to a few hundred people, and that many believe threatens a possible human pandemic is HPAI H5N1.
- LPAI H5N1 occurs from time to time in North America. (In fact, it's often called “North American H5N1,” as opposed to the “Asian” HPAI H5N1.) In its current form, LPAI H5N1 is no threat at all to human health – at least to the best of scientists’ knowledge thus far.
- HPAI strains differ in their ability to cause serious disease when they spread from a bird to a human. HPAI H5N1 is deadly to humans (though so far very hard for humans to catch). But a recent high-path H7N3 strain, which devastated domestic chicken flocks in Canada two years ago, caused only a mild eye infection when it spread to some poultry workers.

- Laboratory tests for bird flu give you some information fairly quickly, while other information takes longer. You usually get the H before the N. You usually get both before the definitive high-path or low-path determination (though you may have a strong high-path/low-path hint from clinical observation – birds are dying or they aren't).
- Some strains of bird flu can be low-path in most wild bird species and high-path in domestic poultry. Some strains can be low-path but then mutate (or not) to high-path after they spread to domestic poultry. H5N1 has both of these traits. So if H5N1 is found in wild birds that are perfectly healthy, it is still possible that it’s HPAI as far as poultry are concerned. And it’s also possible that it’s LPAI but will become HPAI later.
All that is what you ideally want people to understand – though it’s a lot for laypeople (and even for many officials) to absorb. You want people to recognize that not all cases of bird flu are H5N1, and that not all cases of H5N1 are high-path. You want people to recognize that vanishingly few cases of high-path H5N1 in birds have so far spread to a human victim, and that not one of those rare human cases has so far launched a pandemic. And you want people to recognize that if a pandemic ever does start, the human risk will no longer be from birds, but from each other.
At a minimum, you want to avoid giving people misunderstandings. Any story is a misleading story if it creates the impression that there is already a bird flu pandemic somewhere else that fortunately hasn’t reached Our Town yet. Any story is a misleading story if it creates the impression that we are safe from a pandemic as long as our birds aren’t sick. Any story is a misleading story if it creates the impression that every case of bird flu represents an imminent threat to human health. And any story is a misleading story if it creates the impression that so long as a wild bird is healthy it doesn’t matter what bird flu strain it has.
The only way to make this all clear is to say it, and keep saying it. And acknowledge that it is confusing. And admit that it took you a while to understand it too. And apologize for sometimes explaining it in ways that add to the confusion.
- When you find a case of low-path bird flu, you need to announce that that’s what you found – and explain that this is a potentially significant economic problem if it gets into poultry flocks, but not a problem at all for human health (as far as we know).
- When you find a case of high-path bird flu, you need to announce that that’s what you found – and explain that this is a very big economic deal for poultry farmers. Depending on what high-path strain it is, it may also be a potential health risk to poultry workers, and a possible longer-range threat to public health because of pandemic potential.
- When you find certain kinds of low-path bird flu – H5 or H7 – you need to explain that these types could have the potential to become high-path over time. That’s why farmers are culling many chickens that aren’t terribly sick, trying to eliminate the virus before it has a chance to develop into a devastating high-path strain.
- And when you find a healthy wild bird that has a bird flu strain that’s low-path in wild birds but high-path in poultry, you need to take the time to explain why it’s not a big deal (yet) nor are you entirely out of the woods (yet).
I vote for using the terms “high-path” and “low-path” – and explaining that “path” is short for “pathogenic,” which means “disease-causing.” (I’d also point out that these terms are used only to describe the effects of various flu strains on poultry; they’re not used for people.) The abbreviations “HPAI” and “LPAI” probably come across as off-puttingly technical. And phrases like “deadly bird flu” are likely to cause more problems than they solve. A high-path bird flu that threatens to devastate poultry flocks isn’t necessarily deadly to wild birds – or to humans, unless they’re unlucky enough to catch it. A headline about “deadly bird flu” is likely to send a far more alarming signal than you intended.
But the vocabulary issue isn’t the main issue. The main issue is telling the public what kind of avian influenza you have found, and what you think it means (and doesn’t mean). If you are candid and precise, reporters and the public will have a better chance of eventually getting it right.
The biggest dilemma is what to do with incomplete information. I’m a strong supporter of announcing everything you know as soon as you know it, even when there’s more you don’t yet know. That’s the best way to give the public a fair shot at understanding not just the high-path/low-path distinction, but also the fact that it isn’t an ironclad distinction. It’s also the best way to teach the public to trust that you’re not going to withhold potentially frightening information while you wait and hope that new data will prove it isn’t frightening after all.
Waiting and hoping that new data will show a possibly high-path outbreak is blessedly low-path is the high-stakes poker game some veterinary and health officials are now playing.
Last April in New Jersey, for example, authorities discovered bird flu during routine surveillance testing in an urban live poultry market. It was presumably a low-path strain, since the birds were healthy. But see #8 above: Some low-path bird flus can mutate to high-path. State officials said nothing whatever about the initial discovery until they had some fairly advanced lab tests back. Then they announced only that it wasn’t N1. They very likely knew first what the H was, since H lab results normally come in quicker. But they never said. (An apparently knowledgeable source told a reporter from the prestigious science journal Nature that it was H5, but New Jersey officials still haven’t confirmed or denied the claim.) As for the N, at least they said what it wasn’t, but not what it was. As far as I am aware, no other state has steadfastly refused to reveal what strain of bird flu it found – not just while awaiting further data, but even after all the data were in.
Here’s another example, this one from Michigan. State officials announced that routine surveillance had found low-path H5N1 in a pair of wild swans. Fine – I don’t doubt that’s what they found. But odds are they found out first that the virus was H5, then that it was N1, and then that it was low-path. (The fact that the swans weren’t sick wasn’t any help in the high-path/low-path diagnosis; H5N1 can be high-path in poultry and low-path in swans.) So for some period of time Michigan authorities kept to themselves the news that they had some swans that might or might not have the “deadly” Asian high-path H5N1, the one everyone’s worrying about. The possibility they didn’t announce turned out not to be the case, so no doubt they felt validated in their decision to suppress their partial information until they had it all.
But eventually authorities somewhere in the U.S. will almost certainly find high-path H5N1 in birds. The information will again come piecemeal, and the authorities will in all probability have suppressed the early data while waiting hopefully, and futilely, for reassuring final results. When they get around to announcing the bad news, they will be rightly pilloried for not having warned us sooner. This is normal bureaucratic behavior, but it isn’t good risk communication.
How much should we trust what WHO says about pandemic phase?
| name: | Philip | |
| Field: | Interested citizen | |
| Date: | September 30, 2006 | |
| Location: | United Kingdom |
Comment:
There seems to be some concern re the WHO alert system. Currently we are at Phase 3, although there is concern we should be Phase 4 re: Qinghai (July ’05) and the Turkey/Iraq cluster (Jan. ’06).
Is there any known modeling on escalation of alert levels from 3 to 4 to 5 to 6? Has anyone done any planning around the speed of each escalation, or is this not possible?
I accept that WHO internally may be using a different system (not available to the public) and probably plays down the actual risk, but if we are to truly believe the alert levels, has any appropriate modeling been done – perhaps using previous examples, for example SARS?
Peter responds:
This response was written jointly with my wife and colleague Dr. Jody Lanard.
You write: “I accept that WHO internally may be using a different system (not available to the public) and probably plays down the actual risk….”
We have no reason to think that WHO is using a different system, or that WHO is playing down the risk. Everyone – including WHO officials – wishes there were certainty about the predictive value of each cluster, and of each new situation that arises with H5N1 in humans. When WHO investigates a cluster or other new development, it is looking for evidence of progress toward a possible pandemic. If it finds such evidence, it needs to decide – without anything approaching certainty – whether the evidence justifies notching up to the next pandemic phase.
The phases are merely ways of describing a progression of the H5N1 virus in the direction of more efficient human-to-human transmission. The actual cut-off points between each phase and the next were judiciously but arbitrarily defined; WHO could just as easily have divided the progression into more or fewer phases. These cut-offs are not nearly as crisp and definitive as we all wish they could be – and as we all sometimes imply they are. Even if the facts of a particular situation are known and undisputed, there may be room for debate over whether that situation does or doesn’t meet the criteria for Phase 4.
Nor can anybody predict how long H5N1 (or any flu virus) might linger in one phase before moving on to the next. We could move to Phase 4 and stay there for years – which would probably lead many people to conclude we shouldn’t have moved to 4 at all. Or we could move to Phase 4 and then move almost instantly to 5 and 6 – which would probably lead many people to conclude we should have moved to 4 earlier.
The phases are approximations that WHO experts hope will provide at least a little guidance to countries that are deciding how to respond to a changing situation.
Remember: This has never been tried before. We have no experience predicting pandemics – no experience with successful predictions, and no experience with failed predictions.
Everyone worries that some countries may try to hide what is happening, or may not be aware of what is happening in some remote areas. But some people worry also that WHO may try to hide what is happening. You can find entire threads on Flu Wiki and other flu-related websites devoted to this latter worry.
It’s a worry we personally do not share. Here’s why: The more you know the people who work at and with WHO, the more you realize how deeply committed they are, and the more you understand how much they struggle against the technical and political constraints they work under. If or when the situation appears more urgent, and knowable data support that impression, we are convinced that WHO will warn the world. WHO did so with SARS, which to us is the clearest publicly available evidence that it will do so again when it thinks a warning is necessary.
(However, there are important differences between the emergence of SARS – a disease that appeared in humans before any animal source was known – and the emergence of a pandemic virus from an existing known animal source. When SARS appeared, it looked for all the world like the start of a flu pandemic – more precisely, it looked like one of the ways a flu pandemic might look when it starts. SARS turned out to be far less transmissible than flu, and it had a much longer incubation period. But in the first weeks, no one knew this, and it raised the specter of The Next Pandemic.)
As it monitors H5N1 outbreaks in animals and humans, WHO is explicitly worried about errors in both directions. If WHO raises the phase at the very first rumor of increased human-to-human transmission, or larger clusters, it may be responsible for a false alarm. It’s not just that this could lead to serious economic repercussions; it would also impair WHO’s credibility and thus its ability to warn the world effectively the next time it announced a phase change. But if WHO waits until it has evaluated every possible lab test and traced every conceivable source of exposure in a given cluster, its warning may come very late in the evolution of the virus – reducing the time available for urgent efforts to respond to the threat.
WHO knows, almost for sure, that it will end up catching some blame one way or the other. If a severe pandemic devastates the world, by definition WHO will not have warned us early enough or aggressively enough. If years go by with no severe pandemic, it will have made mountains out of molehills. Already, many who expect a severe pandemic are critical of WHO’s reticence, while many who doubt that a severe pandemic is imminent are critical of its stridency. Not knowing which set of critics will turn out right, WHO tries to chart a scientifically defensible middle course and let the blame fall where it may.
None of this means that WHO’s middle course is necessarily the right course. There are grounds for debate over whether WHO should worry more about false positives or false negatives – whether it should be more deliberative (eventually confirming a phase change that others will have announced already) or more urgent (quickly announcing a phase change while others are still skeptical). That's a different debate – a more useful debate, we think – than the one over whether WHO is suppressing facts it knows to be alarming.
Ultimately, if the virus starts causing Phase 4-level damage, WHO officials will probably be slower to announce it than we and they will wish. But it will not have been because of a conspiracy or a cover-up. It will be a delay during which officials assess the new data and debate whether they justify a change in phase.
Below are some responses to other comments and questions in your email. As communication experts who are not flu experts, we want to emphasize that our technical answers below may not be exactly correct, so please do not rely on them as definitive.

You write: “There seems to be some concern re the WHO alert system. Currently we are at Phase 3, although there is concern we should be Phase 4 re: Qinghai (July ’05) and the Turkey/Iraq cluster (Jan. ’06).”
We are not aware of any human cases related to the dead wild birds in the Qinghai Lake area, so from our limited knowledge, we don’t see how the Qinghai avian outbreak would have influenced the WHO pandemic phase level.
In Turkey and Iraq, there did not appear to be any human-to-human transmission, or large clusters. Here is a nice WHO description of the relevance of occasional and very limited human-to-human transmission, dated December 5, 2005, just before the human cases in Turkey started to emerge:
What is the significance of limited human-to-human transmission?
Though rare, instances of limited human-to-human transmission of H5N1 and other avian influenza viruses have occurred in association with outbreaks in poultry and should not be a cause for alarm. In no instance has the virus spread beyond a first generation of close contacts or caused illness in the general community. Data from these incidents suggest that transmission requires very close contact with an ill person. Such incidents must be thoroughly investigated but – provided the investigation indicates that transmission from person to person is very limited – such incidents will not change the WHO overall assessment of the pandemic risk. There have been a number of instances of avian influenza infection occurring among close family members. It is often impossible to determine if human-to-human transmission has occurred since the family members are exposed to the same animal and environmental sources as well as to one another.
(http://www.who.int/csr/disease/avian_influenza/avian_faqs/en/index.html#isit)
A Phase 4 declaration would require “evidence of increased human-to-human transmission.” The worst known situation thus far is one instance of probably three generations of spread – human-to-human-to-human – in three members of an Indonesian family, part of the largest cluster of human cases to date: 7 or 8 people.

You write: “Is there any known modeling on escalation of alert levels from 3 to 4 to 5 to 6?”
There is lots of modeling, but absolutely no data or prior experience to suggest how a progression from 3 to 4 to 5 to 6 will actually occur. No one has ever observed the evolution of an influenza pandemic before.

You write: “Has anyone done any planning around the speed of each escalation, or is this not possible?”
Officials are aware that a pandemic may arise very quickly once any human-to-human transmission begins, or it may evolve very slowly, with larger human clusters “burning out” and not spreading widely for quite some time. Everyone is hoping that the next severe pandemic will be preceded by a prolonged warning period, with gradual signs that human-to-human transmission is becoming more efficient. But all planners know that they have no idea how much warning there will be that “This Is It.” Both rapid-evolution and slow-evolution pandemic scenarios have been used in drills and planning exercises.
Telling 9/11 emergency responders to wear their masks –
and explaining later what went wrong
| name: | Dave Johnson | |
| Field: | Editor, ISHN [Industrial Safety & Hygiene News] | |
| Date: | September 19, 2006 | |
| Location: | Pennsylvania, U.S. |
Comment:
I’m writing a piece on risk communication surrounding the Ground Zero health effects on response and recovery workers. It’s interesting to go back to EPA and OSHA press releases from Sept.–Dec. 2001 and read again and again their reassurances that air samples indicated it was safe for the public, tourists, and financial district workers to “get back up and running” in effect.
The language seemed careful to make the distinction – safe “beyond the WTC site” – but details were seldom provided regarding readings at the site. In a few instances EPA and/or OSHA stated some samples at the site were above limits of standards. But those statements would be followed by positive comments such as “but levels are expected to decrease” in relatively short order, or “standards are set (such as for asbestos) for long-term exposures” inferring that work at Ground Zero was not long-term. Again, the overall tone of these releases comes across as “no worries, it’s all good.” EPA chief Whitman ends one release: “The good news continues to be that the air samples have all been at levels that cause us no concern.”
This to me is a unique exercise in risk communication. What say you?
I understand the feds post-9/11 wanting to come across confident, in control, and not alarmist. I understand that an OSHA inspector couldn’t go up to a firefighter digging for body parts and say, “You’re not wearing a respirator, pal, I’m fining your department.” (Actually, I’m not sure in New York federal OSHA has jurisdiction over municipal governments. But the same would hold true for construction contractors.) And the OSHA chief did give repeated statements reminding workers to “protect themselves” by using masks. (Though according to the OSH Act it’s the employers’ responsibility to ensure workers wear protective gear. Employers get cited, not employees. I have not come across such “reminders” aimed at employers on site.)
On the other hand, I agree with a panelist on a recent NYC TV broadcast who said: “The urgency wasn’t there to get all workers to use masks to protect themselves from the fumes.” Nothing in the press releases or speeches I’ve dug up from the weeks after 9/11 carries a real tone of urgency in terms of the need for proper respiratory protection.
The most direct language used that I came across was from Labor Secretary Chao, speaking Nov. 20, 2001, in NYC announcing an OSHA/WTC partnership. She describes the job of protecting workers being “difficult and sensitive,” the recovery and cleanup work “extremely difficult and dangerous,” and states, “Terrorists have made [Ground Zero] one of the most hazardous workplaces in America.”
Why didn’t the OSHA chief use this kind of graphic language when he visited the site two days after 9/11? That would have provided some of that sense of urgency. Instead, it comes from his boss two months later. I’m guessing politics dictated different communications at different times. What’s your take, Peter?
Peter responds:
The key context for official statements about the safety of rescue and recovery workers at Ground Zero is the much more publicized statements about the safety of civilians some distance from Ground Zero. The most important and most quoted of these statements came from EPA Administrator Christie Todd Whitman on September 18, 2001. Its key sentence reads as follows: “I am glad to reassure the people of New York and Washington, D.C., that their air is safe to breathe.”
Two years later the EPA Inspector General investigated this EPA statement, and revealed that by September 18 EPA had not collected enough data about air quality around the Pentagon and the World Trade Center to justify Whitman’s claim. It wasn’t a lie; that is, Whitman didn’t know it wasn’t true. But she didn’t know it was true, either. It was optimism masquerading as information. The Inspector General’s investigation also found that the White House exercised considerable influence on the statement. I think it’s unduly cynical to interpret this as partisan political interference. It seemed urgently important to give the American people some reassurance. Helping hundreds of thousands of New Yorkers find the courage to return to their homes and offices in lower Manhattan seemed, to some officials, an important enough goal to excuse the decision to go beyond the data. I think this decision was profoundly mistaken, but I’m not convinced it was politically motivated. The goal – at least one goal – was to steady the country, a valid goal even if the chosen means were questionable.
Partisan or not, the September 18 statement was horrible crisis communication. Leave aside the ethics of giving people stronger reassurance than the known facts justify. The crucial crisis communication point is this: When you give people stronger reassurance than the known facts justify, the reassurance rarely works – not even in the short term, before anyone knows whether you will turn out right or wrong. In keeping with the principle of the risk communication seesaw, over-reassuring messages usually backfire. People who are not sure how frightened they ought to be smell a rat; they feel abandoned, left alone with their fears; and they resolve their ambivalence by becoming all the more fearful. Christie Todd Whitman’s September 18 statement that local residents and workers were safe had a paradoxical effect. It frightened the people of lower Manhattan.
It also generated appropriate skepticism, and thus undermined EPA’s credibility on air quality in lower Manhattan. Five years later, the long-term health effect of the 9/11 attacks on people who lived or worked nearby is still a very hot controversy – much hotter, I think, than it would have been if EPA had been cautious rather than over-reassuring at the outset.
I have emphasized this September 18 statement because I believe it is central to the current controversy over whether EPA, OSHA, and various other federal, state, and city agencies did an adequate job of warning rescue and recovery workers. As you point out, the distinction was made at the time. Whitman and her colleagues never claimed the air at Ground Zero was safe to breathe. But as you also point out, Whitman and her colleagues didn’t make nearly as big a fuss as they could have made about its possible dangers. I suspect the decision to over-reassure civilians about the offsite risks got in the way of warning emergency responders aggressively enough about the onsite risks. It would have been hard to insist that Ground Zero was really, really dangerous while urging people a few blocks away to move back in.
Hard, but not impossible. Whitman could have said something like this: “Even though we think the air several blocks from the World Trade Center site is probably safe enough for people to start reclaiming their normal lives, we wish we could say the same about the air at the site itself. Recovery workers are spending long hours in dust and debris that may very well be dangerous. We know that masks and respirators get in the way, but despite the burden the heroic volunteers at Ground Zero really need to keep wearing their safety gear. If people further away also want to wear face masks for a few more days, that extra margin of safety can’t hurt and might turn out to be a very good idea.”
Let me be clear about the distinction between the two situations. Most people in lower Manhattan were ambivalent about whether the air in their homes and offices was safe or not. EPA told them over-confidently that it was safe, and many immediately went to the other side of the seesaw and became more worried. Rescue and recovery workers at Ground Zero, on the other hand, were in the grip of strong emotions (anger at the terrorists, compassion for the victims, determination to take action) that made them impatient with long-term safety precautions. They weren’t ambivalent about wearing masks. They knew they probably should wear them, but they didn’t want to. They experienced the weakness of the government’s warnings as tantamount to permission to disobey.
I also have the impression that Whitman and her colleagues genuinely didn’t realize how serious the onsite risks would turn out to be. This is your field, not mine. But judging from what I’ve read on risk analysis and occupational safety blogs and listservs, the lung injuries suffered by those who worked on the World Trade Center rubble pile for weeks or months seem to have been caused mostly by inhaling pulverized cementious concrete, which turns out to be highly caustic. The focus at the time was apparently on other, more obviously toxic worries: asbestos, vapors from burnt or melted plastics, finely ground glass. Should the experts have realized what the real risks were, and how serious they were – or was 9/11 so unprecedented that there was no way they could have realized its likely impacts? I don’t know. Should they at least have realized how little they knew about the actual risks? I don’t know. If they had realized that cement was the biggest threat, were there different precautions (different masks, perhaps) they could have insisted upon? I don’t know. Is it possible they did realize but were reluctant to say so very loudly? Again, I don’t know.
What should occupational safety and health authorities do in the aftermath of a 9/11-like disaster, when it’s obvious that the air is full of all kinds of possibly hazardous materials for which there are no standards? For that matter, what should occupational safety and health personnel who are not “authorities” do in such a situation? Suppose you’re the safety professional at a factory that has had a major explosion. You don’t know of anything in the air that’s necessarily dangerous. But you don’t know a lot yet about what’s in the air, and some of what you already know is in the air might or might not turn out to be dangerous. Do you require plant rescue and recovery workers to wear masks, goggles, or perhaps even supplied air? Even if the city firefighters are going unprotected? Even if federal and state authorities are issuing vague and unsubstantiated recommendations that they’re not even trying to enforce? Even if the CEO wants to project a can-do image and show that the situation is under control?
Yeah, you should. You should err on the alarming side. You should worry more about being cautious – and looking cautious by genuinely being cautious – than about maximizing the efficiency and comfort of recovery workers or looking like things are well on their way back to normal. This is both good risk communication and good industrial hygiene. But it’s a tough sell.
The over-reassurance (offsite) and under-warning (onsite) that characterized the post-9/11 period are symptomatic of officials’ impulse to cut short the normal adjustment reaction that normal people have to disasters. This knee-jerk impulse is understandable, but it is unwise. Rather than trying to make people “get over” a disaster too quickly – an unrealistic effort that regularly fails – officials should be empathically helping people through the inevitable rough time.
Even in more ordinary times, persuading workers to wear personal protective equipment isn’t easy. Jennifer Busick published an article in the September 2005 issue of Safety Compliance Letter on my views on “Getting Workers to Wear PPE.” ![]() A lot of the recommendations there would help – a little – in a post-disaster scenario too.
A lot of the recommendations there would help – a little – in a post-disaster scenario too.
It’s not as if Whitman and her colleagues weren’t trying to warn about the onsite risks. The iconic photographs of the World Trade Center response nearly all show rescue and recovery workers supplied with masks – but they are wearing their masks down around their necks. I was at a meeting a couple of days ago with a high-ranking New York City firefighter who spent a lot of time at Ground Zero. I asked him about the controversy. “They were issuing warnings,” he told me. “Maybe they weren’t issuing citations, but they were issuing warnings.” Some of the current scapegoating strikes me as pretty unfair. The government aggressively and inappropriately over-reassured civilians. By contrast, it appropriately warned rescue and recovery workers, but not aggressively enough. One of the main reasons why we now want to punish officials for the half-heartedness of their warnings to rescue and recovery workers is because we feel misled and betrayed by their falsely enthusiastic reassurances to the rest of us.
Of course it doesn’t feel that way to emergency responders who will never breathe easily again. It’s a little like the plaintiffs in lawsuits about drug risks. You want the medicine. Your doctor and the label warn you that there could be side-effects. You hear the warnings, but you really want the medicine. And the warnings are tentative, long-term, statistical; and, yes, they’re in a lot smaller type than the promise of symptom relief. So you shrug them off and take the medicine. Years later when your breast cancer or your heart attack is a horrible reality – no longer tentative or long-term or statistical – you understandably tend to feel they should have warned you. They did warn you? Well, then, they should have warned you more loudly!
It’s even more complicated in the case of 9/11. Unlike patients who suffer side-effects from their medications, 9/11 rescue and recovery workers were risking their health for the benefit of others. And I suspect it’s not just the workers who wanted to ignore the warnings. The entire country wanted them to ignore the warnings. We needed heroes, and we have learned from endless movies and TV shows that heroes don’t let personal risk stop them. And they don’t let precautions slow them down either. The willingness of thousands of volunteers to endure horrible conditions was truly heroic. We admired not just the urgent search for possible survivors, but also the slow, laborious search for wedding rings, personal artifacts, and identifiable body parts. We admired the recovery workers who spent months on the "pile" at Ground Zero in much the same way as we admired the firefighters who charged up the stairs of the doomed Twin Towers. We didn’t want to hear anybody suggest these might be foolishly dangerous things to do.
Now we want to blame the authorities for not protecting our heroes sufficiently. And, truly, they didn’t protect our heroes sufficiently. But if they had tried harder to do so, I think we might very well have responded with fury and contempt: “Those pettifogging safety bureaucrats! How dare they insist on their routine safety rules in the midst of a national disaster!”
My wife and colleague Jody Lanard disagrees. She thinks the public would have responded well to strong official requirements to make Ground Zero a safer workplace. At the Pentagon, as opposed to the Twin Towers, recovery workers were sent home if they weren’t wearing their masks. Jody points out that this tougher enforcement of occupational safety regs didn’t lead to a mass groundswell of criticism.
We agree on what officials should have said and done. Although I believe the public wouldn’t have liked them for it, they should have raised more hell about occupational safety at Ground Zero. Even in the first few days when the search for survivors was realistic, they should have been issuing urgent warnings about the importance of not adding to the disaster by unduly endangering rescue workers. As the days passed and rescue gave way to recovery, they should have become more demanding still, insisting that there was no longer an emergency to justify taking excessive occupational health risks.
And they should have framed their warnings with a lot of dilemma-sharing and counter-projection: “We feel terrible being the ones who keep making our nation’s heroes wear those hot and itchy respirators and go home at the end of their shifts and take weekly lung capacity tests. We know we sound like pettifogging safety bureaucrats who can’t tell a national disaster from a routine demolition site. But the national disaster has happened. Our job is to try to make sure we don’t add to the disaster by ignoring how horribly dangerous Ground Zero is right now for recovery workers. Every day since 9/11 we have worried about how to balance the heroic work that’s going on at the site against the need to protect the people who are doing that work – protect them even from their own heroism! We feel like traitors doing it, but starting Tuesday we will be issuing citations to any employer at Ground Zero that fails to enforce the following safety regulations….”
That’s what I think they should have said five years ago. What should they be saying now?
Apologizing. There are of course other important messages. A lot should be said, and is being said, about the importance of getting help to 9/11 rescue and recovery workers who are now disabled and in many cases uninsured. A lot should be said – and not enough is being said – about lessons learned, about how occupational safety will be managed very differently in the aftermath of the next terrorist attack. A little needs to be said about the virtues of hindsight, how much officials wish they had known then what they know now. But the single most important message, I think, is how sorry officials are that they let down the heroes of the 9/11 rescue and recovery.
Christie Todd Whitman seems to be spending most of her time scapegoating instead. On CBS's “60 Minutes,” for example, she said that New York City officials ignored her warnings to make recovery workers wear masks. This may be true. But especially in the context of her over-reassuring September 18 statement about offsite air quality, it is far more important for her to acknowledge that her warnings were too mild, too easy to ignore.
Former New York City Mayor Rudy Giuliani has done some scapegoating too. He criticized Whitman for continually insisting the air was fine – conflating Whitman’s over-reassurances about offsite risk with her (admittedly not very audible) warnings about onsite risk. And he criticized the federal Occupational Safety and Health Administration for not enforcing the mask rule. But on the whole, Giuliani did a lot better than Whitman. “In retrospect, I guess we all should have done it differently: the city, the state and the federal government,” he said on CBS’s “The Early Show.” “Everybody bears responsibility for it.”
addendum:
Based in part on the Guestbook entry above, Dave Johnson wrote a two-part column on “Lessons from Ground Zero: Risk Communication” ![]() for his ISHN Ezine (Industrial Safety & Hygiene News). A slightly revised version
for his ISHN Ezine (Industrial Safety & Hygiene News). A slightly revised version ![]() was published in the November 2006 hard-copy issue of ISHN (pp. 58, 60, 62) under the title, “Lessons from Ground Zero: Risk Communication in the Fog of Disaster.”
was published in the November 2006 hard-copy issue of ISHN (pp. 58, 60, 62) under the title, “Lessons from Ground Zero: Risk Communication in the Fog of Disaster.”
How do we “know” if they’re telling us the truth about BSE – or about anything?
| Name: | Lisa Erickson |
| Field: | Livestock producer, Pioneer ET breeder |
| Date: | September 4, 2006 |
| Email: | ksfboers@ocii.com |
| Location: | Canada |
Comment:
I have never been able to get an answer to this question. EXACTLY how were BSE-positive animals traced back to Canadian sources? Was it by DNA tracking, and if so then where and what was the tracking data?
In this day and age of fraud, propaganda, misinformation, errors, and omissions, must we still accept unquestioningly those news releases carefully prepared by governments and other connected officials for public consumption (pardon the pun)? What factual, ascertainable info is publicly available for consumers/producers to examine? How do we test if the DNA or other tracking data was without political bias or partialities?
Peter responds:
The factual BSE research for this answer was done by my wife and colleague Jody Lanard.
First of all, only one of the three known U.S. BSE cases (“mad cows”) so far was tracked back to Canada. That was the first one. The second was tracked to Texas. The third couldn’t be tracked, but no one was hinting that it might have come from Canada.
The Canadian Food Inspection Agency (CFIA) and the U.S. Department of Agriculture (USDA) state that they are in full agreement about the Canadian origins of the first cow. It was a dairy cow for which there were decent records – including an ear tag that matched the tag number on the dated Canadian health certificate that accompanied the cow when it was imported from Canada to Oroville, Washington.
The CFIA said: “Through the Health of Animals ear tag, herd and registration records, it was determined that the animal was born on April 9, 1997 on a farm in Alberta.” It also said: “The CFIA successfully traced the history of the recent BSE-positive cow found in Washington state.”
For more information, check out the CFIA statement and the USDA statement.
Also check the list of the 12 BSE-positive cows found in North America ![]() as of August 23, 2006 (the three found in the U.S. and the nine found in Canada). Of the nine Canadian cases, by the way, the earliest (1993) was determined to have been imported from the U.K. The other eight are believed to have been born in Canada.
as of August 23, 2006 (the three found in the U.S. and the nine found in Canada). Of the nine Canadian cases, by the way, the earliest (1993) was determined to have been imported from the U.K. The other eight are believed to have been born in Canada.
Why nine Canadian cases and only three U.S. cases? We didn’t try to nail down that one. It could be that Canada has a bigger cattle industry, or tests more of its cows, or does a better job of targeting potentially sick cows for testing. It could be that Canada has been less successful in preventing the disease (perhaps it hasn’t policed feeding practices as well). It could be that the U.S. is keeping some of its sick cows secret. Some of these hypotheses are easily checked. Some aren’t.
Which takes me back to your original question: How do we know they're telling us the truth? For the most part, we don’t. To the best of my knowledge, none of the relevant BSE evidence has been made publicly available for skeptics to do their own testing and checking. Of course evidence is rarely made publicly available in that way. Even the labs that do the testing have to trust that the samples they’re given are from the cows they’re told they’re from. For that matter, juries don’t get to do their own lab analyses or hire their own experts either; they have to rely on the chain of evidence, and on the testimony and cross-examination offered by the parties.
Our best assurance that the one cow said to have been imported from Canada really was imported from Canada is that the Canadian authorities didn’t disagree. Nor has any whistle-blower surfaced to claim that Canadian and U.S. officials were conspiring to mislead the public regarding that one mad cow’s country of birth. Nor has there been a lot of controversy over whether the cow really came from Canada.
By contrast, there has been plenty of controversy about other aspects of BSE testing. The second of the three U.S. cases, for example, was BSE-positive according to a preliminary screening test. The USDA reasonably called the test inconclusive. On the USDA’s “definitive” test of that cow, using its gold standard (at the time) immunohistochemistry test, the cow came up BSE-free. Months later, after a harsh critique by the USDA Inspector General, the cow was tested a third time using the Western Blot test, the current gold standard. This time it was judged BSE-positive. Another controversy: The inability to trace some BSE-positive cows back to their birth herds has led to heated debate in the U.S. about how to implement a better tracking system, despite objections by the cattle industry.
A conspiracy to maintain falsely that that one cow originated in Canada seems unlikely, but it certainly isn’t inconceivable. Like most conspiracy claims, this one is almost impossible to disprove, but the weight of the evidence is against it.
Basically, the trustworthiness of information is based on the answers to three questions. In order of preferability:

- Are skeptics (or their trusted agents) able to verify the information independently? When it’s feasible, independent verification is certainly the best answer to mistrust. See my 2002 column on “Accountability” for more on how to enable skeptics to judge for themselves – and on why companies and governments are reluctant to do this even when they’re telling the truth.

- Are those who are providing the information (or at least some of them) organizations that would rather the results had come out differently? What lawyers call “admissions against interest” are intrinsically more credible than self-serving claims. That's why it makes sense to trust the CFIA more than the USDA about the cow that was born in Canada.

- Have the information sources built a record of trustworthiness that they can draw on now? Even self-serving claims are credible when they come from organizations that have routinely made admissions against interest in the past, and have rarely been caught cheating or even accused of cheating. For some additional insight into how well USDA’s BSE communications stack up against this third standard, see “Misleading toward the Truth” and “Sharing and Bearing Dilemmas.”
One final comment. It isn’t just sources whose reliability should be interpreted in terms of whether what they say is self-serving or an admission against interest. The trust or skepticism of the public – and especially of the stakeholders – should be interpreted that way too. We tend to be too trustful of information that supports our views or interests; we don’t often question claims we’d like to believe. And we tend to be too mistrustful of information that doesn’t go our way; we’d rather sound paranoid than accept the bad news. This is human nature, of course. But it has implications. Listen hard to skepticism when it’s reluctant skepticism – that is, when it comes from a source that would rather the information were true. And listen hard to skeptics when you don’t really want to – when you would rather the information were true. By contrast, skepticism on the part of people who stand to gain from their doubts should be treated, well, skeptically.
Localized geographical identifiers: How to say “This Means You!”
| Name: | Maura |
| Field: | Emergency planning public relations/communications |
| Date: | August 28, 2006 |
| Location: | New York, U.S. |
Comment:
I am interested in any published research references and your opinion about what “identifier” is best to use during emergencies for public information/direction. For instance in a densely populated area, where villages are in towns, should first responders provide public health and safety information based on the town a person lives in? Would Zip Codes work?
In other words, is there risk communications research on common geographical identifiers that could be used during a crisis situation that would “speak” to a wide demographic?
Peter responds:
I don’t know of any research on the issue of localized geographical identifiers. Please don’t take that as definitive. I am a rotten bibliographer. I forget where I read most of what I have read – and the day is long gone when I could read pretty much everything published about risk communication. If you find some relevant studies, please let me know.
The problem of how to tell people “This Means You!” is very real. In the run-up to an emergency, before their vulnerability is obvious and their anxiety is high, people tend to look for reasons to think a warning doesn’t apply to them. There is a story, perhaps apocryphal, of an effort to warn people that the river was about to flood and they should evacuate to higher ground. The sound truck cruised slowly up Elm Street telling everyone to evacuate. Then it skipped Spruce Street and came back on Maple Street, two blocks over. The people on Spruce Street heard the message twice, first as the truck came up Elm and then again as it came back down Maple. But they didn't evacuate. The truck had skipped Spruce, so they figured the flood would too.
The moral of the story is to localize your warnings as much as possible. “West Nile Virus is a threat to California” isn't going to provoke as much precaution-taking among Californians as “West Nile Virus has been found in every county in California.” Of course it has to be true. A list of California counties (or better yet, cities and towns) where West Nile Virus has been found will work well in the locations listed – but people living in unlisted locations are likely to react like the residents of Spruce Street.
When Neil Weinstein and I were working on radon warnings in New Jersey (back in the 1980s and early 1990s), we conceived the idea of a newspaper advertisement listing all the New Jersey Zip Codes in which homes with high radon levels had been identified. We believed this would be nearly all the Zip Codes in the state. We even thought about putting the Zip Codes in random order, so people would have to search the ad. For those who bothered to search, finding their Zip Code would make them feel “targeted” and vulnerable – a strong motivator to test their homes. Those who didn’t search would at least see a long small-type list of Zip Codes; we hoped they’d figure theirs was probably on the list. We never got around to running (or testing) the ad.
The cost of localizing your message is reduced impact on people in the locations you don’t specifically mention. The benefit of localizing your message is increased impact on people in the locations you do mention. Where it’s feasible, I’d mention every village in the town, every neighborhood in the city. If you can manage to vary what you say for each location – a different “area reference person” to call about any questions, for example – that strengthens the localization even more. But if localization forces you to leave out a lot of places you also want to reach, it could do more harm than good.
What does it mean to “manage” terrorism – and the fear of terrorism?
| name: | Tarekegn | |
| Field: | Disaster manager | |
| Date: | August 17, 2006 | |
| Email: | tarekegn1962@yahoo.com | |
| Location: | Ethiopia |
What I would add to this site:
Effective methods of terrorism risk reduction.
Comment:
Is terrorism a disaster? An emergency, a crisis, a catastrophe?
What was wrong with the US that made it hard to manage the 9/11 accident (at least to decrease the risk)? Is the risk of terrorism manageable? Can the events of September 11, 2001 demonstrate that terrorism is a form of risk that cannot be managed?
Peter responds:
I know that many in the field distinguish crises, emergencies, disasters, and catastrophes. In general, I think, catastrophes are the worst; they are sometimes described as disasters that have been mishandled or inadequately prepared for. Both catastrophes and disasters have to end in serious harm; emergencies and crises, by contrast, can come out okay if you’re lucky and skillful. (Hospital emergency rooms routinely prevent health disasters.) “Crisis” is the mildest and most metaphorical of the four terms. If you describe 9/11 or Katrina as a crisis, you risk being accused of understatement.
I am not terribly sensitive to these distinctions. There are lots of examples in my writing in which the terms are used more or less interchangeably.
The 9/11 attacks were certainly a disaster, and maybe a catastrophe. (They were not an accident.) The long-term threat of terrorism is certainly a crisis, and maybe an emergency.
Your other question – whether terrorism can be managed – is fascinating. I’m a risk communication expert, not a risk management expert, but it seems clear to me that terrorism is exactly the sort of risk that can be managed. The fact that the United States hasn’t had another successful domestic attack since 9/11 is evidence that terrorism is being managed – and managed more effectively than most of us predicted and than many of us are willing to acknowledge. The recent arrests in the U.K. are evidence of the same thing.
It is certainly possible to argue that much is wrong with the efforts of various governments (including mine) to manage terrorism – that some of what needs to be done (e.g. shipping port inspections) isn’t happening; that some of what is being done (e.g. airport security) is more for show than actual risk management; and that some of what is being done (e.g., the war in Iraq) is provoking more terrorism than it is preventing. But these are all arguments over how best to manage terrorism risk, not arguments that it cannot be managed.
But like many manageable risks, the risk of terrorism is not entirely preventable. Good management can reduce the frequency and consequences of future attacks, but not to zero. There will be more terrorist attacks, and some will succeed.
The risk communication problem is the extremely complex relationship between terrorism risk management efforts and the extent of public alarm about terrorism.
Take airport security, for example. Whether or not airport security actually deters terrorists, it is defended in part on the grounds that it reassures the flying public. But does it? Or does it reemphasize our vulnerability and rekindle our anger, frustration, and sense of impotence? By reminding us about the risk of terrorism, might airport security paradoxically make us more afraid? I’m not sure.
I have periodically exchanged emails on this topic with Canadian security expert Frank Harvey. Harvey argues that people, at least in the developed countries of the west, are becoming “addicted to security.” He describes what he calls “the homeland security dilemma” – that successful security efforts lead people to feel more vulnerable and demand still more security.
Harvey elaborated as follows in an email responding to a draft of this Guestbook answer:
The homeland security dilemma (HSD) is a much broader thesis that encompasses predictions about public and government behavior/perceptions. Simply put, the greater the financial costs, public sacrifice and political capital invested in security, the higher the public’s expectations and corresponding standards for measuring performance, the more significant the public’s sense of insecurity after each failure, and, paradoxically, the higher the pressure on governments and citizens to sacrifice even more to achieve perfect security. The central argument can be summed up by the following counterintuitive thesis: The more security you have, the more security you will need. This is not because enhancing security makes terrorism more likely (although the incentive for terrorists to attack may increase as extremists feel duty-bound to demonstrate their ongoing relevance), and it is not because successful security measures lead people to feel more vulnerable. It is because huge investments in security (and other financial, political and civil liberty sacrifices) raise public expectations and demands, so that even small failures and perhaps even a few major successes (like those in Toronto and London) increase threat perceptions and amplify public outrage. Moreover, the public’s perceptions (whatever they may be) are not the only issue here – political assumptions about public perceptions determine public policy. If leaders expect a public backlash after small failures, then they will do as much as they can to reach perfection – even if that benchmark is impossible and irrational. Newly implemented security rules regarding prohibiting liquids on flights are a case in point.
In June 2006, Harvey wrote to me:
Consider the following – as a result of the Toronto area arrests of 17 terrorist suspects last week, 70% of Canadians now believe there will be other terrorist attacks in Canada in the near future. In other words, what may turn out to be one of the most successful counter-terrorist operations in history has “increased” threat perceptions in Canada to U.S. levels. Politicians will be very reluctant to question those perceptions, and that’s the dilemma.
I’m not convinced that Harvey is right. I think it is very difficult for people to sustain their fear of terrorism, or indeed of any risk. A successful terrorist attack like 9/11 generates an enormous amount of fear for a while, but soon enough – too soon, many would say – most of us return to the “new normal,” more fearful of terrorism than before 9/11, but less fearful by far than right after 9/11. Are people in the U.S. and Europe excessively worried about terrorism today, as Harvey seems to believe? Or are we insufficiently worried? (Or, conceivably, does the public have it about right?)
In his response to my draft answer, Harvey wrote that “30–50% of Americans (and now Canadians) are worried about being a target, and a much higher percentage (50–70%) believes another attack will take place, despite the very low probability of these events actually occurring, and despite the perfect homeland security record to date.” It seems to me that worrying about being a target is a bit different from believing that you are likely to be a target. As for believing another attack will take place, that’s a belief I share, and one I think the public is better off sharing than disdaining.
I do agree with Harvey that successful counter-terrorism efforts have a paradoxical impact. They are experienced in part as near-misses, and thus as evidence of vulnerability. Media coverage of the recent arrests in the U.K., for example, routinely described them as bad news; reporters saw the story less as civilization’s victory over terrorism than as proof that the terrorists are out there. And Harvey is also right that successful security efforts make people inclined to expect that future security efforts will be successful. This may or may not lead people to demand more security. But it almost certainly leads people to see any future terrorist success as a security failure deserving of blame. It’s easy to imagine the investigations, recriminations, and scapegoating that would follow a second 9/11 in the U.S. And it’s easy to understand why government officials are tempted to respond to this thought experiment with additional layers of security. As Harvey has put it, “the problem is not the ‘failure of imagination’ – we’ve pretty well nailed that one. The problem now is the ‘imagination of failure.’”
The risk communication lesson here, I think, is the urgent need to communicate that terrorism risk management isn’t dichotomous – that while a perfect record is certainly our goal, it isn’t our expectation and shouldn’t be the public’s expectation. Here’s how I put it in an email to Harvey:
How might people’s level of fearfulness and expectations of success be affected by a government communication effort that stressed, simultaneously, the good success record that has been achieved and the impossibility of sustaining it? My sense is that the U.S. government has actually stressed neither as much as I would have recommended. Claims of past success are, perhaps, constrained by security concerns themselves, which lead to suppression of the details that would give such claims more drama and more credibility. And claims of future failure are constrained by a fear that the public will reward the politician who promises the impossible more than the politician who manages expectations realistically. So we end up with a government that seems to be making an implied promise of future perfection, but keeps it deniable by not making it explicitly and keeps it unbelievable by not documenting the sources of past success. This seems pretty unwise to me. I would be saying, very explicitly: We’ve done a lot better than we ever expected. We expect to continue to do well … but not THAT well.
I don’t want to ignore the fact that this Guestbook comment came from Ethiopia, a country with a very different history than the U.S., the U.K., and Canada vis-à-vis terrorism and public attitudes toward terrorism. I am much too ignorant to offer an opinion about these differences. I just want to acknowledge that an informed assessment of terrorism risk communication issues in Ethiopia might lead in very different directions.
For readers interested in more of my exchange of emails with Frank Harvey, our June 2006 emails are appended, along with Harvey’s comments on my draft of this answer.
Motivating disaster preparedness
| name: | Margie | |
| Field: | Volunteer, Office of Emergency Services and Homeland Security | |
| Date: | August 17, 2006 | |
| Location: | California, U.S. |
What I would add to this site:
It’s a wonderful site. Many thanks for all your efforts in providing the vast array of information.
Comment:
What have you found to be the best way to motivate people to prepare themselves for disaster?
Peter responds:
Books have been written about how to motivate disaster preparedness – and few have done the job as well as California’s earthquake preparedness advocates. So I doubt I can add very much of value. But I’ll give it a shot….
In December 2005 I participated in a national conference, sponsored by the CIA, the FBI, and others, on how to get Americans more worried about the threat of terrorism. Nine months later the 9/11 attacks solved the problem.
The most effective motivator of disaster preparedness, in short, is a disaster. Even that works only for a while. Terrorism concerns in the U.S. are demonstrably lower today than they were in the months after 9/11 – though they are almost certainly higher today than they were before the recent arrests in the U.K.
There are two key lessons here. The first lesson is that disaster preparedness advocates should treat disasters (and near-misses) as teachable moments. The best time to talk about hurricane preparedness, for example, was shortly after Katrina struck. Sadly, there will doubtless be other hurricane preparedness communication opportunities this season, so hurricane preparedness communicators should prepare their messages and wait.
The second lesson is that “eternal vigilance” just isn’t in the cards. Since it is incredibly difficult to keep people poised for disaster, the focus should be on preparedness measures that don’t require staying permanently on guard. Precautions that only have to be taken once (or once in a while) – such as getting vaccinated or packing a go kit – are preferable to precautions that have to be taken constantly. And precautions that have to be taken constantly need more sustainable motivators than the fear of disaster. Many people wear their seatbelts, for example, out of habit or peer pressure or concern about getting a ticket; not everyone imagines a crash before buckling up.
This raises another important point. Often disaster preparedness can most effectively be motivated by something other than the fear of disaster. Auto safety communicators have to decide if their deepest commitment is to people wearing their seatbelts or to people worrying about car crashes. If it’s the former, a child who keeps wheedling till you put your seatbelt on is a terrific motivator. But many advocates are so focused on their own reasons for wanting people to take a precaution that they neglect (or even oppose) powerful motivators they consider demeaning or at best irrelevant. Is it okay if teenagers use condoms because they’re sexy, or does it have to be to prevent pregnancy and sexually transmitted diseases? Is it okay if people drive hybrid cars because they’re trendy, or does it have to be to avert global warming? Is it okay if people install smoke alarms because the electrician said they’re required, or does it have to be out of worry about a fire?
Not that fear is a weak motivator. The research on fear appeals has shown again and again that they work. Scaring people is a very good way to get them to prepare for disasters. There are two important qualifiers here. The first qualifier concerns efficacy. If people feel impotent to protect themselves, then scaring them does more harm than good. So fear appeals often need to be accompanied by self-efficacy appeals. The second qualifier: The relationship between fear and action is a ∩-shaped curve. Occasionally people are already more frightened than is useful; they may look apathetic but they’re actually in denial, and scaring them more will only push them more deeply into denial. But usually people who look apathetic are apathetic, and scaring them will help motivate more action.
In my consultations on precaution advocacy – that is, on high-hazard, low-outrage risk communication – these are the three barriers I encounter most often among my clients. They don’t want to wait for the teachable moment. They don’t want to deploy motivators they consider irrelevant or even trivializing. And they don’t want to frighten people. So too often they end up dispensing information when nobody’s listening.
If you can get past these three barriers, motivating disaster preparedness will still be a challenge. It’ll take time; it took a generation for seatbelts and smoke alarms to become the norm. But it won’t be impossible.
End-of-the-world risk communication
| Name: | James Blodgett |
| Field: | Statistician |
| Date: | August 5, 2006 |
| Location: | New York State, U.S. |
Comment:
An upcoming physics experiment, due to start up in 2007, may destroy the Earth. Several string theorists have published papers predicting that the next generation of high-energy particle colliders will produce mini black holes. Such a collider is under construction at CERN, the world’s largest particle physics laboratory near Geneva.
There are reasons to think this collider will be safe, but these reasons may not apply. In the worst case, a mini black hole could swallow the Earth. Strangelets, another collider product, could cause equivalent problems.
For more information and references see www.risk-evaluation-forum.org.
This risk seems a classic case for being careful, for what risk analysts call “the Precautionary Principle.” Unfortunately it appears that this principle is not being applied. A Cassandra complex is at work. Cassandra predicted the fall of her city, Troy, but was not heard. The same is happening with this issue. The public is apathetic. CERN physicists are good enough people, but they initially thought their project to be safe, and it is hard to get them to reverse that and cancel a multimillion-dollar project because of low-probability concerns. Francesco Calogero, a physicist, has suggested that the risks be evaluated by a red team, arguing in favor, and a blue team, arguing against. Until Calogero’s idea becomes standard, it is up to us, the public, to provide the blue team.
This is a risk issue that poses interesting philosophical problems. It is also hard to communicate. Do you have any suggestions?
Peter responds:
I know nothing about the “mini black hole” risk except what I read on your website.
But the generic issue of how to communicate about high-magnitude low-probability risks is a very familiar one. See my long column on “Worst Case Scenarios,” which deals at length with this problem.
Undoubtedly the most common mistake when communicating about risks that are awful but unlikely is to neglect to admit clearly enough or often enough that they’re unlikely. At the extremes this amounts to claiming that they’re likely … or even that they’re certain. George Bush sounded confident that Saddam Hussein had weapons of mass destruction; Greenpeace sounds confident that greenhouse gases will cause disastrous climate changes. In both cases, the argument for precautions was/is properly grounded not in confidence about the risk’s high probability but in the unacceptability of its high magnitude. We buy fire insurance not because we are confident our homes will burn but because we want to cover ourselves against this slim but horrific possibility.
It follows that advocates of precautions against high-magnitude low-probability risks are obligated to distinguish the precautions they consider worth taking (even though they’ll probably turn out unnecessary and wasted in the end) from the precautions they concede are too costly or too difficult to justify (even though the risk magnitude is huge). Were there less damaging ways to protect against WMDs than to invade Iraq? Do we really need to abandon the internal combustion engine and eviscerate the global economy in order to ameliorate the threat of global warming?
In the face of the ultimate risk magnitude – literally the end of the world – you face another, closely related problem. If the risk magnitude is infinite, even an incredibly tiny risk probability is presumably unacceptable. The assertion that any non-zero risk of ending the world is too high sounds sensible enough. But then you are essentially saying that the physics experimentation you’re discussing cannot be permitted under any circumstances. Moreover, an awful lot of technologies over the centuries have been identified as having some potential for ending the world. Can we afford to allow a veto power to anyone who asserts, however implausibly, that the world might end if a particular technology isn’t stopped?
Does any non-zero probability of ending the world end the discussion? Or are there conditions under which you would say: “Okay, the risk still isn’t zero, but it looks smaller now than it did when I first started thinking about the problem. Given the new data, the new theorizing, the new precautions, the new limitations on what experiments you’ll do, the new something, I now think it’s acceptable to proceed.”? If so, you need to provide some tech specs, some conditions for giving the go-ahead. If not, you need to concede that your opposition to this research is unalterable, and that it may set a precedent for others who oppose other technologies on comparable grounds.
Two other suggestions come to mind as I ponder your situation.

- I think it’s important to be vivid about the worst case scenario you envision – what would this particular end of the world be like?

- I think it’s important to concede and counterproject what skeptics are thinking as they read – that all previous predictions of the end of the world have turned out false. You call this a “Cassandra complex,” but it’s really an empirical observation that doomsday predictions don’t have a terrific track record. Less literally apocalyptic scenarios face similar problems, as those who warn about the dangers of global warming, peak oil, and pandemic influenza have discovered. But you face it in its purest form. Of course end-of-the-world predictions only have to be right once to be right forever. But they’ve never been right yet. Since this is what your audience is thinking as it reads, you need to acknowledge explicitly that it is so.
There are probably other suggestions deducible from the “Worst Case Scenarios” column.
James responds:
An immediate reaction: I am not very enthusiastic about your advice to describe the worst case graphically, although as an expert perhaps you are right. My reaction is to fear that readers would see sensationalism.
There is a tendency to dismiss end-of-the-world predictions, and I think sensationalism tends to evoke that dismissal, so I try to downplay that aspect. Also, modeling the risk factors is hard enough; modeling and describing the final collapse (and explosion) is harder still. Some physicists might disagree with details, and would jump on this opportunity to say we are wrong. I see little reason to give them that opportunity. These details do not matter; the result is the same. We might achieve emotional “graphics” by mourning our (potentially) lost grandchildren, but I have as yet not wanted to go there. It is hard to mourn lost grandchildren when the probability of losing them is (relatively) low. What do you think?
Peter responds:
You may be right vis-à-vis end-of-the-world predictions. For more ordinary worst case scenarios (not so unlikely, not so horrific) the evidence suggests being graphic about the high risk magnitude and candid about the low risk probability is best. But maybe you can’t afford to be graphic about anything.
I also see your point that graphic details could lead to irrelevant debates over whether you got the details right.
james replies:
You ask me to answer the following question:
Does any non-zero probability of ending the world end the discussion? Or are there conditions under which you would say: “Okay, the risk still isn’t zero, but it looks smaller now than it did when I first started thinking about the problem. Given the new data, the new theorizing, the new precautions, the new limitations on what experiments you’ll do, the new something, I now think it’s acceptable to proceed.”?
This is a good question.
Some would say that, in the case of destruction of the Earth, an experiment must have an extremely low probability of this outcome, one in many billions, before proceeding. For example, see Adrian Kent, “A critical look at risk assessments for global catastrophes,” ![]() Risk Analysis 24 (2004), pp. 155–166.
Risk Analysis 24 (2004), pp. 155–166.
But science also has benefits. A transcendent risk can perhaps be balanced by a similar probability of a transcendent benefit. An example would be something on the order of a Star Trek space drive that could expand the human race by orders of magnitude and perhaps solve other risks. But despite their prominence in science fiction, breakthroughs of this magnitude are quite improbable, especially as the result of a single experiment. Therefore I would want the probability of destroying Earth to be at least as improbable before proceeding with that experiment.
Also into the balance put the costs of shutting down the experiment. An expensive collider will have to be abandoned, and a bunch of physicists will have their careers disrupted. Another cost is the cost of reducing some of the pleasant anarchy in the world. It is nice for scientists when they can do whatever they want. Finally, on the risk side of the ledger, powerful breakthroughs are often associated with brand new risks.
Estimating the probability of these risks and benefits is subjective and approximate. Physicists and others vary widely in their estimates. They also vary in their prescription of the level of risk that they believe would justify continuing, or halting, the experiments in question.
Collider physicists chose their profession because they believe in it. They also have a vested interest, and there is organizational pressure to move on with a large project. Therefore, they are likely to see the benefits as larger and the risks as smaller than an objective estimate. This is part of why Precautionary Principle folks say the burden of proof should be on the people proposing the activity.
A second problem is that of governance. While we debate what the world should do, it is appropriate that we think and write as if we were policy-makers, but that can give the illusion that we have solved the problem when we have only proposed a solution. We have influence on policy only if the world listens. Frequently the world does not listen. In 1998 Smith Dharmasaroja, a Thai meteorologist, predicted an Indian Ocean earthquake and tsunami. He advocated tsunami warning systems, but was not taken seriously. The warning systems he advocated could have saved thousands of lives in the tsunami of December 2004.
In this case collider physicists have listened a bit. They have produced two papers addressing the issue. However, they are not listening to new results that question their safety factors. They have got their okay, and plan to proceed. A few physicists and others disagree, but few hear what we are saying.
What can be done about this? What we are doing is advocating for precaution. If enough people are convinced we are right, then governments will pull the plug. There are precedents and prescriptions to which we can appeal. In 1975, biologists met at Asilomar and agreed to limit risky experiments in genetic engineering. Also, much has been written about the Precautionary Principle that should apply here. We would like to see at least a spirited debate on this topic, a careful examination of the remaining safety factors (most appear to have holes), and a professional risk assessment.
Notes from the Beirut evacuation
| name: | Caroline | |
| Field: | Government risk communication specialist | |
| Date: | July 27, 2006 | |
| Location: | Quebec, Canada |
Comment:
I was one of the lucky ones evacuated from Lebanon by the Canadian Government. I had landed in Beirut on Wednesday July 12th and the airport was bombed and closed on the 13th!
I decided to drop you a line to get your feedback on some of my observations about difficult crisis communications choices during the evacuation.
The evacuation journey took over 70 hours, 30 of which were spent in a stadium in Larnaca, Cyprus, sort of a holding tank before we get a turn on the plane. I know the Canadian representatives were doing their best, working round the clock, literally, with limited resources, having to deal with an increasingly outraged and distressed crowd. But I was struck by the lack of communications with the evacuees. I experienced for myself the impact of being kept in the dark, the psychological effect of not knowing what’s going on. People really needed to be kept informed of any developments, good or bad, to help them maintain their sanity.
To keep my own sanity through those 30 long hours, I offered my help to the staff on site – answering people’s questions and making sure everyone was registered. I insisted on the importance of giving information on a regular basis to those waiting, even if there was nothing new to say, or even if it was bad news. I argued that people would be able to cope. I gave the staff a set of recommendations to help them keep the frustration and outrage level down, based on what I’ve learned in the past couple of years and based on what I was experiencing along with everyone else in that room.
However, I wasn’t always sure what would be the best approach. When the reasons for delay are outrageous in themselves, what do you do? What do you tell people? It was a tough call. Speculations were perceived as lies because the trust level was very low. Empathy wasn’t enough. People wanted answers, but a lot of the questions had only “I don’t know” answers. There was no one in charge, no one who seemed to know the answers – no one who could tell you why some priority people were still there, why there were planes available but no way to fill them because manifests were not ready, what was being done to fix problems, who was fixing them, and how long before they could be fixed.… The situation was extremely frustrating.
It was very hard to manage giving some information without raising expectations. In order to cope, people in crisis look for hope in every piece of information shared, in every action they can take. If their raised expectations are not met, the result can be even greater outrage.
If you have any feedback to share, I would really appreciate it.
Peter responds:
I’m glad you’re home safely, glad you were able to help, and glad you took the time to write.
I agree with you, fervently, that people in crisis need a steady stream of communications – even if most of what you have to tell them is old, extremely tentative, or more apologetic than useful. The failure to keep talking was one of the most serious communication failures during Hurricane Katrina. The more screwed up things get, the more tempting it is for those in charge to avoid interacting with the victims or potential victims they’re trying (and, for the moment, failing) to help – and the more important it is to overcome the temptation and sustain the dialogue.
But as you say, sustaining the dialogue doesn’t guarantee that people will take the screw-ups gracefully. You focus on two problems. If the bottom line of your communication effort is to keep telling people that things are still pretty screwed up, they’re going to be upset – not as upset as if you had stopped communicating along with everything else, but upset nevertheless. That’s the first problem. The second problem is the grasping-at-straws phenomenon. Given half a chance, people will interpret what you tell them as much better news than it is – and then feel betrayed and all the more outraged when things don’t turn out as they’d hoped.
The best way to cope with these two problems, I think, is to keep going meta on them. “I have a little information, but not as much as many had hoped I’d be able to get.” “This isn’t going to be much help, but here’s what we’ve learned so far.” “There’s a little bit of possible good news, but it’s very tentative and we need to be careful not to get our hopes up too much.” “Mostly I couldn’t get any answers, and the answers I got don’t make too much sense.” “Things are still very chaotic, obviously. I’m really sorry.”
All that only helps a little, of course. When things are bad, things are bad. The best you can do is not to make things unnecessarily worse by communicating too little (the really serious sin) or too optimistically (much more forgivable, but still a mistake).
caroline replies:
I would add the importance of choosing the right spokesperson, someone with leadership skills and a confident demeanor to add credibility to the messages. I’m hoping things will run more smoothly with the rest of the evacuees, who will be and should be very grateful to be flown to Canada.
Outrage about global warming
| name: | Dave Gold | |
| Field: | President, Gold Health and Safety Consulting, Inc. | |
| Date: | July 20, 2006 | |
| Email: | Dave@GoldSafety.net | |
| Location: | California, U.S. |
Comment:
I’ve attended a few of your classes through AIHA, and I’ve enjoyed them quite a bit, and put some of your concepts to use in my work over the years.
I was reading an op-ed article this evening reprinted from the L.A. Times, called “If Only Gay Sex Caused Global Warming,” and you came to mind. The point of the article, in essence, is that the global warming threat does not get people excited.
Recently I saw the Al Gore movie, An Inconvenient Truth, plus I have read several articles about global warming in the paper and heard them on the radio, etc. It occurred to me after reading the L.A. Times article this evening that perhaps the reason people are not galvanized about the threat of global warming is because the outrage isn’t very high. Even the words “global warming” don't sound very threatening, do they!
It also occurred to me that perhaps, if you were concerned about this issue, and/or a Democrat/Al Gore supporter, maybe you could contact him and see what you could do to help his effort at getting people to care about this issue a lot more than they do.
Maybe you already have?
Just my thoughts. It would be nice to hear back from you on this topic. It's important.
Peter responds:
Half a dozen times in the last two decades I have been contacted by an activist group, an academic organization, or a consultant (not yet by a politician) for my advice on how to get people more outraged about global warming. And one of my longest-lasting clients, since 1985, is Environmental Defense (formerly Environmental Defense Fund), a leader on the global climate change issue.
Especially in the early years, I was very pessimistic about the prospects for arousing massive public outrage (or even “concern ”) about global warming. As you point out, the words don’t sound very threatening. “Warming” is generally a good thing. Moreover, global climate change is too abstract, and therefore hard to keep in mind, not nearly as memorable as, say, an endangered species (preferably a cuddly mammalian one). And it’s too tough – too big, unalterable, global – and thus likelier to inspire learned helplessness and denial than determined action. And it’s too slow-moving, too imperceptible, with dire outcomes only in the distant future; like frogs in a beaker of slowly heating water, we’re not equipped to notice that we will eventually start to boil.
The wonderful July 2 Los Angeles Times op-ed column you mentioned, by Harvard psychologist Daniel Gilbert, makes some of these points, and some others, in explaining why people are less worried about global warming than Gilbert thinks we ought to be.
What’s surprising isn’t how little progress the fight against global warming has made. What’s surprising is how much progress it has made. At least in terms of public awareness, public opinion, and public concern in the developed world (even the U.S.), we’ve come a lot further in two decades than I would have predicted.
- Who would have thought, even a few years ago, that what is essentially an expanded PowerPoint presentation by a wonky former Vice President and Presidential candidate would be something of a hit in movie theaters?
- This week’s Newsweek cover story is entitled “The New Greening of America: From Politics to Lifestyle, Why Saving The Environment Is Suddenly Hot.” The introductory anecdote and much of the rest of the article focuses on global climate change.
- A Google search this morning for the term “global warming” yielded 104,000,000 hits. “Endangered species” got only 38,900,000; “flu pandemic” – my own obsession – is up to just 3,310,000.
One of my corporate clients is a Canadian oil company whose CEO is firmly convinced that global warming is nonsense. Carbon dioxide is plant food, he points out to anyone who will listen (and many who won’t). But several months ago the company asked for my advice on how to reconcile the CEO’s personal views with the company’s need to make concessions. Thus its newest Corporate Responsibility Report includes a list of accomplishments and pledges to reduce greenhouse gas emissions. And it includes this quotation from the CEO: “I remain skeptical of the science related to the impact of CO2 on the climate. Nonetheless, I acknowledge that many stakeholders hold a different opinion on this issue, some very strongly. I also understand that the issue of CO2 emissions and climate change poses particular risks to the energy industry, be it reputation or regulatory risk.” In other words, public concern about global warming, at least in Canada, is so strong that the company is taking and publicizing precautionary steps its CEO considers scientifically silly.
Remarkable though it is, the progress we have made in public concern about global warming may not be sufficient to turn the tide. Global warming itself has progressed faster than most experts (even most activist experts) predicted. So has industrial development in China and India, where catching up to the West is a higher priority than reducing greenhouse gas emissions. And unlike my Canadian oil company client, the Bush administration continues to resist the pressure of public opinion on this issue.
Several aspects of outrage are especially relevant to the continuing effort to build and mobilize public outrage about global warming.

- Natural versus industrial. The ongoing debate over how much of the global warming trend is caused by human activities and how much is due to natural cycles is mostly about outrage. The logically relevant question is whether human activities can ameliorate the damage done by global warming. Whether we caused the problem in the first place is pretty much beside the point. But it’s a lot easier to mobilize outrage about anthropogenic problems than about natural problems. So activists insist that global warming is manmade, and their critics insist it isn’t.

- Morally irrelevant versus morally relevant. Outrage is more about good versus evil than about safe versus dangerous. So for purposes of mobilizing outrage at global warming, it’s important that it results not just from human activities, but from the activities of bad guys. The oil industry and the Bush administration are the movement’s favorite bad guys. Don’t feel sorry for them; they earned it. But the trick that has so far stymied the movement, I think, is to get public opinion to pivot from outrage at the bad guys to willingness to make personal lifestyle changes. Telling people they’re the bad guys if they drive SUVs or don’t switch to low-wattage light bulbs isn’t good strategy. But persuading people to make the connection is essential.

- Knowable versus not knowable. The impact on outrage of “unknowability” – uncertainty and expert disagreement – is complicated. If outrage is already pretty high, unknowability makes it higher: “How dare they expose us to risks they don’t even understand themselves?” But if outrage is low, unknowability is a good excuse for inaction: “We’ll start worrying after the experts get the science straight.” In the early years, the science behind global warming was hotly debated, and the debate strengthened the fervor of both sides. The argument wasn’t over how sure we were; it was, rightly, over whether we should wait to be sure before taking precautions. Though there are still scientific dissenters, the consensus that global warming is real and serious is a lot stronger today. Opponents still argue that we shouldn’t take costly and disruptive precautions until we’re sure. But the focus for the movement has shifted from “yes we should” to “we are sure.” Paradoxically, this may actually make it harder for the movement to sustain the outrage.

- Not memorable versus memorable. Memorable images are the key to overcoming the abstractness and imperceptibility of global warming. Melting icecaps are absolutely essential to the movement. But there are limits to how much people are willing to sacrifice (“Not my SUV!”) to save some icecaps. The next stage of the movement is going to need images that are equally memorable but more human, more personal. There are plenty of such images lurking in the computer models of a hotter future – a map of the next century’s U.S. with its new coastlines is a good candidate. But these are all hypothetical, vitiated by people’s healthy skepticism about computer models. What the movement really needs is a dramatic, photogenic human outcome that’s happening now.
- Fair versus unfair. Like moral relevance, unfairness is an almost indispensable asset in the mobilization of outrage. For much of the rest of the world, and for American elites, the statistics on U.S. energy use are a superb motivator; the evidence that Americans produce enormously more greenhouse gases per capita than anyone else gives the global cause of global warming a much-needed frisson of victimization and moral superiority. But of course for ordinary Americans it works the other way; the prospect of feeling guilty is a good reason to decide that global warming isn’t that big a deal. And opponents of the movement can marshal unfairness arguments on their behalf as well. The Kyoto Protocol isn’t fair to the West, because it exempts developing countries from the obligations it imposes on developed countries. A more symmetrical agreement to reduce greenhouse gas emissions wouldn’t be fair to the developing world, because it would prevent them from achieving our level of prosperity. Since nobody can think of a fair way to address global warming, the only fair thing to do is nothing.
These five are by no means the only outrage issues that shed some light on the global warming controversy. But they’re a start.
(As for contacting Al Gore, I don’t usually make cold calls to prospective clients. But feel free to give him my number.)
Wearing personal protective equipment around hazardous waste sites: Damned if you do, damned if you don’t
| Name: | Emery Graham |
| Field: | Ex-brownfields coordinator |
| Date: | June 27, 2006 |
| Email: | egraham@ci.wilmington.de.us |
| Location: | Delaware, U.S. |
What I would add to this site:
Environmental Health and Safety behavior influence approaches.
Comment:
EPA and OSHA have clear regulations about the use of Personal Protective Equipment (PPE) for persons who are involved with hazardous waste sites. However, when brownfield project mangers visit local residential areas contaminated with hazardous wastes they often fail to wear the prescribed protective gear. The people who live on the contaminated land are not aware of the protective practices available to minimize harm from the toxins. I believe that the residents’ failure to act is supported by the EPA professionals’ failure to inform them of the PPE requirements and their failure to wear the prescribed protective clothing.
My survey research indicates that fewer than 25% of people professionally involved with brownfields follow the health and safety regulations cited at 40 CFR 311 and 29 CFR 1910. What’s your perspective on this phenomenon and how might I go about correcting it?
Peter responds:
This is a toughie.
Many commentators – myself among them – have pointed out the contradiction of telling residents a nearby waste site isn’t terribly dangerous and there’s no need to worry, while you and your colleagues are walking around in moonsuits. It’s not necessarily a technical contradiction. There’s a difference between the occupational exposures of people whose jobs take them to one hazwaste site after another and the environmental exposures of people who live near one particular site. It can make technical sense for the former to wear PPE and still mean it when they reassure the latter that their risk is minimal.
But it sure doesn’t ring true! “You’re here for an hour and you're wearing all that protective gear. My kids and I are here all the time, with no protective equipment at all. And you're telling us there’s nothing to worry about?”
So I can see how staff at a brownfields site might be tempted not to wear their PPE.
Now you’re raising exactly the opposite concern. Your worry is that when staff don’t wear their PPE, that sends a message that the site is safe. This in turn may lead residents not to take actions they might otherwise take to protect themselves, and to demand that the people managing the brownfields cleanup do what is needed to protect them.
In theory the answer ought to be obvious. At genuinely hazardous sites, staff should wear their PPE – and should be glad to send the message to residents that the site is dangerous enough to justify such precautions. At sites where the hazard is tiny, staff should try not to wear their PPE any more than legally required, in order not to send a misleading message or a double message.
What’s wrong with this theoretical advice? For one thing, wearing your PPE is dichotomous, while risk isn’t. It’s not clear what you should do at a site that is neither entirely safe nor especially dangerous. Moreover, opinions differ about whether a site is dangerous or not (or how dangerous it is). And opinions aren’t always unbiased. The company that’s going to pay for the cleanup has a vested interest in its looking as safe as possible; the activists who want a more thorough cleanup have a vested interest in its looking as dangerous as possible.
Both sides, it seems to me, should appropriately act on their convictions (albeit their convictions are affected by their vested interests).
Those who think the site is really dangerous should put pressure on staff to wear lots of PPE, partly for their own safety and partly to send the “right” message to residents. If they won’t wear the gear that’s legally required, report them to the regulators; if that doesn’t work, raise hell. Once they’re wearing the gear, point out to residents that if the site is dangerous enough to justify all that PPE, it’s got to be dangerous enough to justify the other precautions you’re advocating.
Those who think the site isn’t really dangerous should try to get staff to wear as little PPE as the law permits, partly for their own convenience and partly to send the “right” message to residents. If you’ve got to wear PPE, don’t ignore the contradiction between your reassuring claims and your alarming apparel. Talk about why the rules make you wear all that gear, and why – even so – you think the site is a pretty low-risk environment.
Is mid-crisis consultation possible?
| Name: | Paul |
| Field: | Public relations executive |
| Date: | June 27, 2006 |
| Location: | Ireland |
Comment:
Many theorists and practitioners (including yourself) emphasise the importance of meaningful dialogue with stakeholders and publics in making decisions in relation to risk. Do you envisage this dialogue occurring once a crisis occurs? Will the time exist for such formalities? If so how do you see this process operating?
Peter responds:
I didn’t used to think mid-crisis consultation was possible. And obviously sometimes it isn’t. But more often than I imagined, it is.
Several of the best examples I know about come from Singapore during the SARS crisis. One question that arose, for example, was whether to release the names of Singaporeans under home quarantine. (One such person was photographed in a local bar, flourishing his quarantine order.) Revealing the names would enable neighbors to help police the quarantine … and enable them to help provide supplies to people who had been ordered to stay home. But it was an obvious invasion of privacy, and might lead to post-quarantine stigma even for patients who never got sick.
Prime Minister Goh Chok Tong went on national television to explain that he wasn’t sure what to do, that his cabinet’s advice was divided, and that he therefore wanted the advice of the public. He announced a 24-hour public comment period. Newspaper op-ed pages published articles and letters pro and con; Goh himself chaired a debate in a high school auditorium. At the end of the 24 hours, he reported back to the country that most people seemed to want other people’s names released, but nearly everyone agreed it wouldn’t be right to release their own names. On that basis, he said, he had decided to respect the privacy of those under home quarantine.
The Singapore government also did mid-crisis consultation on whether or not to close the schools, and on several other SARS dilemmas.
Even if you can’t (or feel you can’t) take the time to consult in the middle of a crisis, it is still possible to share the dilemma. That is, instead of pretending that your decision was easy and obvious, you can acknowledge that it was a close and debatable judgment call. This doesn’t have all the advantages of consultation, obviously; it doesn’t give people a chance to speak their mind. But it does give those whose viewpoint lost in your internal debate a sense that their perspective was respectfully considered before you decided to move in a different direction.
For more on dilemma-sharing (whether before or after a decision), see my column on “How Safe Is Safe Enough.”
Talking to poultry consumers about bird flu: How reassuring is too reassuring?
| Name: | Dan Rutz |
| Field: | Federal government information officer |
| Date: | June 20, 2006 |
| Location: | Georgia, U.S. |
Comment:
Thank you many times over for your thoughtful and comprehensive piece on talking about bird flu to poultry consumers. I really think it is among your best, if not the very best.
I especially liked the first chapter and the second part of the second. I do have a few reservations about the beginning of the second chapter, which I’ll share.
Your initial point that many farmers in affected areas may not worry enough about their exposure is well taken, although that risk really isn’t relevant unless their particular localities are involved. Obviously the general good-husbandry message is valuable to all backyard farmers and I think the materials USAID is putting forth are both practical and (if adopted) protective.
I love your paragraph in #1: “Understandably, people overreact…. We have taught them, mistakenly, that it’s about the birds.” I think you succinctly summarize the disconnect between pandemic flu fears and avian flu responses: “It isn’t absolutely clear what mental model….” This section is a must read as far as I’m concerned. You have created a valuable analysis of this unfortunate confusion.
I think it is especially important for us to avoid the “dangerous logic” of minimizing the pandemic flu risk on the grounds that none of our poultry is infected. Of course you’re right about the reverse logic this suggests: When our birds DO get sick, it falsely implies, our pandemic risk escalates. GOOD CALL.
Chapter 2 on “Being Candid and Empathic about the Human Risk of Avian Influenza” also offers lots of practical advice and, to my mind, just a little bit of over-indulgence.
Let’s first keep in mind your very sound statement: “In the meantime, we face a much tinier but nonzero human health risk: the risk of catching bird flu from infected birds.” That accurate concession on your part should, I think, figure in what follows – especially since an immense misjudging of that risk (which has happened in every new “bird flu” country) has resulted in immeasurable distress, and very measurable economic harm to “little people” who have, in some cases, been driven to the brink.
While we in public health cannot accept responsibility for occasional tragedies, we should, I think, be mindful of the collateral damage (which, I think you both are) and what we might do to lessen it (which you also do in this piece). The U.S. Ag Secretary quote is partially wrong, and partially right: “Poultry is safe to eat.” Wrong! He should have said cooked poultry is safe to eat. “Cooking poultry will kill the virus.” Right.
I’m not sure why you dwell on “proper” poultry preparation. The results of Jody’s audience participation exercise are not as impressive as the record which suggests that even when we cut corners (and apparently nearly everybody does), we STILL manage to avoid the various diseases associated with poultry consumption, e.g., Salmonella and (based on only about 200 cases worldwide) H5N1 as well. Sloppy preparation practices and an unprecedented epizootic notwithstanding, we are seeing vanishingly little disease associated with poultry consumption, even in the most impoverished corners of the earth. That, to me, speaks volumes about the “tiny” risk. You got it right when you said that; it IS a tiny risk and we should, I think, figure out the right way to say so.
Later, in #6, you suggest: “It [the risk] isn’t tiny because cooking (normal as opposed to meticulous cooking) is guaranteed to kill the virus.” Actually it probably is tiny because “normal cooking” is apparently sufficient to protect against the foodborne diseases associated with poultry (Salmonella and H5N1, to name two). You are, I think, splitting hairs to bolster your point that public fear is justified on the basis of an objective disease threat. It isn’t.
I would certainly agree that public fear IS justified for other reasons, and I am on board all the way that we must respect that fear and its resultant behaviors. I do not agree, however, that we should “enable” that fear by acquiescing to the false premise that the risk is anything greater than “tiny.” As the essay progresses you both do an EXCELLENT job of explaining just how we might go about the business of both respecting people’s concerns and steering them toward more effective countermeasures. I mean it, you really helped me a lot with that and I thank you.
I continue to cling to the notion that media, as with all of us, goes through its own adjustment reaction, and this is actually magnified through society by the coverage. This, to me, is self-evident and opens possibilities for innovative messaging strategy: At the podium I might say (when the first swan turns belly-up in the Princeton Lagoon), “The arrival of H5N1 on our shores is, indeed, a sobering event, and a major news story. Because we’ve anticipated this for so long, and because it is a ‘first,’ it is big news, and you can expect to see screaming headlines and blaring TV accounts. The attention is all about the novelty, and has comparatively little to do with public safety. Yes, we will be stepping up surveillance even more, in an effort to keep the virus out of the commercial poultry stock, which, to our best knowledge, remains virus-free. We will let you know if that changes … promise. Regardless, we would remind you that poultry always requires special care because undercooked poultry can carry germs that make people sick. Thorough cooking kills these germs. So if you like chicken, there really is no health-related reason not to continue enjoying it. Now, as always, don’t eat it raw or pink. Eat it well done instead.”
Over and over I will say, as you do, we need to validate the adjustment reaction (even or especially the news media’s) and guide people through it – with empathy rather than contempt. We need to work on how best to do that, walking the fine line of respecting but not embracing vanishingly small possibilities. I know we can’t use other threats for comparison, and I know some people won’t eat chicken for awhile – I think you’re right about that, and it is of course their decision. But we can, in good conscience, work towards an accommodation to the “new normal” because, after all, the risk is so very, very “tiny.”
I really want to thank you for this very, very helpful addition to the field. I really mean it.
Peter responds:
Thanks for your kind words – and your constructive criticism.
I don't think we’re far apart. The main issue here, as I see it, is this:
- The message Jody and I object to is: “Properly cooked chicken is completely safe.” This is true. But it’s misleading and over-reassuring to those who don’t realize that we seldom cook chicken properly; it’s off-putting to those who do realize that we seldom cook chicken properly; and it sets the first group up to feel betrayed and thus to overreact when there’s a human bird flu case that might be due to poultry consumption.
- The message we propose instead is: “Normally cooked chicken is pretty darn safe, though not completely safe – because most chicken doesn't have H5N1; because H5N1 transmits to humans only with great difficulty; and because cooking adds yet another margin of safety. A still greater margin of safety can be achieved by meticulous adherence to the procedures for ‘properly’ cooking poultry.” This is also true, and it doesn’t have the three disadvantages of the first message.
We share the conviction that much harm and little good is accomplished by poultry avoidance. We share the goal of diminishing this reaction. We share the belief that acknowledging (and maybe even validating) the adjustment reaction, instead of ignoring or belittling it, will help accomplish that goal. We differ, a little, on whether it is also important to be careful not to over-reassure about the safety of poultry – that is, whether the distinction between “completely safe” and “pretty darn safe“ is a distinction that makes a difference.
By the way, all this will change markedly if there’s ever a mutation that facilitates efficient bird-to-human transmission (rather than human-to-human transition). If that happens – and I don’t know of any reason to think one mutation is more or less likely than another – then we won’t face a pandemic; we will face a serious zoonotic disease. We won’t need to worry about social distancing, but we will need to worry about dangerous poultry. If this happens, it will be about the birds!
“Mild” versus severe pandemics – public health versus emergency response
| name: | Melanie Mattson | |
| Field: | Publisher, Flu Wiki | |
| Date: | May 18, 2006 | |
| Location: | Virginia, U.S. |
What I would add to this site:
Just keep doing what you are doing and I’ll keep coming back.
Comment:
Given the continued decay of both our public health infrastructure and our hospital capacity, a flu pandemic along the lines of 1968 would overwhelm the system, and the fragility of just-in-time supply lines would fray seriously, if not break. We don’t have to go all the way back to 1918 to examine how fragile our current systems are. The words “mild” and “pandemic” no longer belong in the same sentence.
Peter responds:
Well, yes, the experts seem to agree that our public health system is a shambles and it wouldn’t take much of a pandemic to overwhelm our hospitals. Maybe something like 1968 (about as mild as flu pandemics get) would be enough. And thanks to just-in-time inventory control, it wouldn’t take much of a pandemic to cause significant supply line disruptions either – especially if governments feel politically compelled to shut their borders. Again, maybe a rerun of 1968 would do it.
(I’d be a fool to disagree with the publisher of Flu Wiki about anything to do with pandemics. What you’re doing isn’t just giving the world by far the best source of pandemic information anywhere; you’re also creating a real worldwide pandemic preparedness community of people who guide each other, support each other, and sometimes scold each other. Flu Wiki is wonderful!)
Still, a rerun of 1968 would be a far different story than a rerun of 1918 (or, conceivably, something even worse). The main issues in a 1968-like pandemic are going to be influenza issues. But in a 1918-like pandemic, flu might turn out to be the least of our problems. While the flu virus does what it does and we wait for a vaccine to be developed and mass-produced, pandemic-induced shortages of food, energy, potable water, non-flu-related medicines, and the like could end up taking more lives than the virus itself. So could civil disruption.
In late 2005 I was working with an Australian chemical company on risk communication issues completely unrelated to pandemics. When the pandemic risk came up over lunch, I asked the CEO if his company manufactured elemental chlorine. It did. I asked if it sold into the water treatment market. It did. I asked what the company’s plans were for making sure it could continue to supply chlorine for water treatment during a pandemic. After talking some about raw materials, trucking firms, and inventories, we reached this discouraging conclusion: Roughly 5–7 days after a severe pandemic reaches Australia, some public water supplies may no longer be safe to drink. People who survive influenza can die of typhoid. My working definition of a “mild” pandemic is a pandemic that probably won’t keep my Australian client from getting chlorine to his water treatment customers.
One crucial aspect of this issue is who’s going to be in charge. Governmental response to a 1968-like pandemic should probably be run by public health authorities. The response to a 1918-like pandemic needs to be run by emergency response authorities. For the U.S. government, this is the distinction between the Department of Health and Human Services and the Department of Homeland Security (and its Federal Emergency Management Agency). In Canada, it’s Public Safety and Emergency Preparedness Canada versus the Public Health Agency of Canada. In New York City, it’s the Department of Health and Mental Hygiene versus the Office of Emergency Management.
Just about every country and just about every state, county, and city where I have consulted has one department for health and another for emergency response. Sometimes one of the two departments is running the pandemic show, and the other is virtually uninvolved. Sometimes they’re fighting over who gets the job. And sometimes they’ve actually built a fairly decent collaboration.
Ideally, I think, public health departments should be in charge of preparedness and response for a mild pandemic, and emergency response departments should be in charge of preparedness and response for a severe pandemic. That means they need to work together on preparedness. And it means they need to be ready to hand off operational control from the health people to the emergency response people as soon as the pandemic starts looking more like 1918 than 1968.
A depressingly common pattern so far: The health people are in charge, want to stay in charge, and are doing what they can to marginalize the emergency response people. So naturally they talk a lot more about the shortage of hospital ventilators than, say, water treatment facility chlorine supplies.
This is almost certainly one of the reasons why health departments have so often understated the potential magnitude of pandemic worst cases. It is also a reason to honor HHS Secretary Michael Leavitt, who has passionately insisted a flu pandemic might be horrific, and in the process has opened the door to greater DHS involvement.
Why do people keep smoking?
| name: | Eric Casey | |
| Field: | Final year student, risk management, Middlesex University London | |
| Date: | May 12, 2006 | |
| Location: | United Kingdom |
Comment:
I would like to know what the barriers are that can occur in communicating the risk of lung cancer and death from tobacco smoking.
I have seen all the communication strategy deployed to inform the public about the risk involved in tobacco smoking. But amazingly people seem not to take notice and still continue to smoke even more. What are the hindrances to effective risk communication with regard to this problem?
Peter responds:
The research literature on why people continue to smoke, and how best to persuade them to stop, contains literally thousands of publications. I don’t feel competent to summarize this literature – certainly not in a short Guestbook answer. But let me make a handful of points, some obvious and some, perhaps, not so obvious.

- In the battle between long-term health and short-term pleasure, pleasure has formidable weapons. It is never easy to persuade people not to do something they enjoy in order to improve their odds of living longer.

- Tobacco is addictive; quitting is physically difficult. And for most smokers the habit is deeply engrained psychologically as well – part of how they socialize, how they get through hard times, how they see themselves.

- The main problem doesn’t seem to be that smokers don’t know smoking is dangerous. Depending on how you ask the question, smokers sometimes actually overestimate the quantitative risk, predicting a higher death rate from smoking than the epidemiological data show. The problem is much more what psychologist Neil Weinstein calls “unrealistic optimism.” This is a very basic phenomenon. Most people judge themselves to be less vulnerable than the average person in just about every way: less likely to get fired, to get mugged, to get cancer, etc. So smokers can know that smoking is deadly in principle and simultaneously believe that it is very unlikely to kill them.

- People who are committed to a risky behavior construct rationales for continuing that behavior. Many smokers mistakenly believe that they do something (exercise regularly, avoid inhaling, smoke “light” cigarettes) that makes the risk tolerably low. Many plan to quit soon – and grossly overestimate the probability of success. Others claim a preference for living “fully” no matter what the risk, or predict that something else will probably kill them anyway so they might as well keep smoking.
- Most smokers start young, imagining that smoking is cool, that it will help them fit in better, that it will improve their sex lives, that it’s a way of rebelling against their parents. By the time they’re wiser, the dependency is strong.
- The most successful anti-smoking communication campaigns have not usually focused on the wisdom of quitting for the sake of one’s own health. Among the appeals that can sometimes work better than health:
- Love. Don’t smoke in front of your children – you don’t want them becoming smokers too.
- Attractiveness. Smokers stink (literally). People don’t want to be around them, ride in their cars, visit their homes, kiss them.
- Anger. The tobacco industry hooked you with lies and deceptions. Get even by quitting.
- Courtesy. Don’t smoke around people who object. It’s rude to inflict your smoke on non-smokers.

- Despite the difficulties, millions of people have quit smoking. In the U.S. there are now more ex-smokers than smokers. (I’m one of them. I had my last cigarette on July 1, 1981. But who’s counting?)
Preparing for a severe pandemic
| name: | Jonathan Waldron | |
| Field: | Dentist/former naval aviator | |
| Date: | May 9, 2006 | |
| Email: | jcwdentist@hotmail.com | |
| Location: | Georgia, U.S. |
Comment:
Your analytical methodology for evaluating all sorts of situations is exceptional – especially risk evaluation and possible reaction. But in the case of a worst-case scenario flu pandemic (the probability of which is very low year-to-year, yet high measured in centuries), the analysis breaks down due to the unknown effects of panic on a service-based economy. We have little precedent for this, other than the isolated populations affected by the recent hurricanes. But this will be national.
The number of possible permutations on civil society from a year-long pandemic makes government planning very problematic. With a little thought, even the most casual observer can foresee a cascade of financial calamities affecting most of society. Even if you could “work” from home, who is going to pay you? Do you really want to stand in the grocery store with a wad of money to buy food when others haven’t worked in months? Probable? No. Possible? Yes. Likely in the future? Yes.
How to deal with the complexity? Reduce the solution to a simpler solution: We need a new way of making vaccines that can be produced more quickly.
Peter responds:
I agree that the worst case scenario for a pandemic is horrific. Even a repeat of 1918 would be horrific, and that is not the worst case – though it’s the worst flu pandemic in recorded history, and it may be the worst the world can afford to plan for. I hasten to add that much milder pandemics, along the lines of 1957 and 1968, are also worth planning for. They would be anticlimactic compared to the doomsday scenarios Robert G. Webster and some other experts have been talking about. But they’d still be significant in public health terms, and they’d constitute a serious challenge for hospitals that are overburdened already.
I agree also that a speeded-up process for manufacturing influenza vaccines is badly needed. It’s hard to imagine coming up with one so fast that we would be spared even the first wave of a pandemic (unless we got lucky and the virus dawdled for a few months between when it “learned” efficient human-to-human transmission and when it started spreading rapidly). But the quicker the better, obviously.
My best guess is that for the first few months of a severe pandemic, if and when we get one, we won’t be able to do much medically. But our non-medical response will make a big, big difference in how well we get through the crisis.
- How well we plan now to implement social distancing strategies, for example, may determine the extent to which we can slow the spread of the disease, buying time for the vaccine manufacturers.
- How well we plan now to keep critical jobs filled and critical supply lines open may determine the extent to which we avoid “secondary” deaths – not from the virus but from shortages of food, energy, clean water, non-flu medications, and the like.
- How well we plan now to reorganize our economy for emergency conditions may determine the extent to which we sustain ourselves, our jobs and incomes, and our morale.
- And how well we plan now to communicate candidly with people and to call on them to help themselves and help each other may determine the extent to which society (and civility) crumbles or hangs together.
Since I’m a communication person, this last point is especially important to me. John Barry’s book about 1918, The Great Influenza, reports real differences between U.S. cities in whether officials leveled with their citizens or tried to over-reassure them. Barry concludes that cities (like San Francisco) that were candid saw less social disruption than cities that tried to soft-pedal the bad news in order to “avert panic.” Although public panic is far rarer than most officials imagine, it is perhaps likelier to emerge during a severe pandemic than during most crisis situations. All the more reason to treat people like adults – to share the bad news, share the feelings of devastation, and enlist their forbearance and their help.
And all the more reason to get them used to the possibility beforehand.
Fake Tamiflu
| name: | Zak | |
| Field: | Engineer | |
| Date: | April 25, 2006 | |
| Location: | United Kingdom |
Comment:
Concerning your Tamiflu stockpiling piece, one more “It's Futile” argument you haven’t directly covered that I saw on Wikipedia’s article on Tamiflu is that stockpilers buying it without a prescription (probably the majority of them) have no way of verifying the authenticity of their purchases (a similar issue to trading on eBay). Governments presumably (hopefully!) don’t have this problem.
I guess this would belong under argument 5, “The Tamiflu might not work,” because there’s arguably little difference between genuine-but-ineffective Tamiflu and flour-filled capsules if that’s all you have at the onset of a pandemic.
Thanks for an interesting article, anyway.
Peter responds:
I haven’t got a very good idea how much of the Tamiflu available on the Internet is real and how much is fake. But I’ve certainly seen warnings (we mentioned them briefly under #18) that there's a lot of counterfeit Tamiflu out there.
As you point out, even genuine Tamiflu may not work. But fake Tamiflu is guaranteed not to work. As far as I know, there hasn’t been a Tamiflu shortage this flu season, and prescriptions have been filled without any policing of whether they were for an actual case of seasonal flu or a pandemic flu stockpile. The flu season is winding down now, and it’s hard to tell what the situation will be in the months ahead. I’d find a doctor willing to give me a prescription and head for a bricks-and-mortar drugstore.
Activism versus education, sensationalism versus inspiration
| Name: | Iyra |
| Field: | Student |
| Date: | April 25, 2006 |
Comment:
My spouse and I met at an environmental publication. I was there with a biology and natural history interest and he was there because of an interest in wildlife protection and environmental activism. Over time, I decided to get back into academic life. Recently, he has had more opportunity to engage in direct action.
I completely support his motives and am prepared for the consequences of peaceful protest, but I am having difficulty in distinguishing activism from actions intended to hit the media in sensational ways. He argues that the first thing is to capture interest and only then can you make a point. I believe real change will be slow and people on the other side have to be inspired to take corrective action rather than pressurized. What is your opinion?
Peter responds:
It’s hard to be sure without knowing exactly what he’s doing, but I think I’m probably more on your husband’s side than on yours. The important point, though, is that the world needs people on both sides.
There are several ways activists can overplay their hand and risk doing more harm than good. Among them:
- They can break the law, hurt people, or damage property.
- They can come across as rude, intransigent, unreasonable, extremist, or obsessed.
- They can make factual claims they can’t back up and lose credibility.
These are real risks, and serious activists take them seriously. At the same time, the risk of being too mild-mannered, too boring, and too willing to compromise is also real. It is simply true that some level of outrageousness helps attract media coverage. It also helps attract the attention of readers and viewers, and much-needed contributions of money and volunteer time. And as I noted in my recent column on “The Outrage Industries,” the public is a lot more forgiving of the alarmist exaggerations of activists than of the over-reassuring exaggerations of industry. (The public is not generally forgiving of activists who hurt people or damage property, however.)
Of course you’re right that persuading people on the other side requires a much gentler, longer-term, more empathic approach.
It helps to see activism and education, sensationalism and inspiration, as all part of an ecosystem of social change strategies. As in any ecosystem, diversity works better than monoculture. Somebody needs to arouse attention among the uninvolved. Somebody needs to mobilize the true believers. Somebody needs to educate the ignorant. Somebody needs to negotiate compromises with the opposition. Somebody needs to stick to the data. Somebody needs to inspire with lofty goals. Somebody needs to hit hard at evil practices. In successful movements of the past – labor, civil rights, feminism, etc. – all these niches were filled. It sounds like your husband is helping to fill some of them, and so are you.
Talking to wildlife rescuers about their bird flu risk
| name: | Rachel Fischoff | |
| Field: | President, Wildlife Rehab Alliance | |
| Date: | April 16, 2006 | |
| Email: | sfischo@calstatela.edu | |
| Location: | Illinois, U.S. |
Comment:
I am the President of the Wildlife Rehab Alliance, a U.S.–Canada wildlife rescue and rehab organization whose members routinely rescue, rehab, and raise downed and/or orphaned wild birds and wild mammals, and return them to the wild. With H5N1-infected dead swans in Europe and a dead marten in Germany in the recent news, I am vigilant.
Your site is thankfully realistic and useful. I appreciate the total coverage; and that the points are openly, logically and sanely explored. It helps me decide how to present the issues to WRA members.
I presume that wildlife rehabbers and wildlife rescuers will, eventually, be especially at risk. Think for a moment about what we do. When there is a wild duck thrashing sickly on the banks of a pond, we capture it and care for it. When there is a dazed eagle on its back in a muddy roadside ditch, we pick it up and rehab it. When we see a limp, whimpering orphaned baby raccoon in the brush, we swoop it up and raise it.
Will we know which ones are victims of H5N1 – i.e., which ones are dangerous to our health? No way. We didn’t know which ones had West Nile Virus either. Many of us, perhaps romantically, figure that we’ve already HAD West Nile several times!
If you have any special thoughts about our H5N1 concerns and issues, I would be most grateful to hear them.
Peter responds:
Two risk communication issues arise when thinking about wildlife rescue/rehab in the context of bird flu. The one you seem most worried about is how to make sure your members take the risk of exposure to H5N1 seriously enough, if/when it arrives in the U.S. and Canada – especially given that some of them may have underestimated the risk of West Nile Virus. The second issue, of course, is how to keep wildlife rescuers from overreacting to this real but fairly small danger.
With animal rescuers who are insufficiently concerned, the obvious task is to alert them to the risk. They may need a wake-up call that getting up close and personal with an H5N1-positive bird (or mammal) is a real risk – small, because H5N1 is hard for humans to catch, but nonetheless real. I would emphasize also that wildlife rescuers are an invaluable H5N1 surveillance resource. Your volunteers may be the first to encounter a sick or dead bird, or they may be the ones to get the call from a neighbor. You need a protocol for liaising with public health authorities – one that protects the volunteer while it helps protect the community.
You don’t have to reinvent the wheel. Check out the USGS National Wildlife Health Center page on “Interim Guidelines for the Protection of Persons Handling Wild Birds With Reference to Highly Pathogenic Avian Influenza H5N1.”
Bear in mind, though, that not everyone who seems unconcerned really is unconcerned. Some wildlife rescuers may actively resist the reality that the birds and mammals they care about so much might actually kill them. (In much the same way, many wildlife experts have resisted the accumulating evidence that migratory birds are important vectors for H5N1.) This is closer to denial than to apathy; it’s a willful refusal to consider the risk. If you think this may be an issue, you might want to put less stress on the risk to volunteers, and more stress on the risk to other wildlife. Transporting a bird that’s sick with H5N1 to a bird sanctuary, for example, doesn’t just present a small risk to the volunteer who does the transporting; it may also present a large risk to the other birds in the sanctuary. In order to help keep H5N1 from spreading more widely through the bird population, rescue procedures may need to change.
As wildlife rescuers become more aware of the risks, the second question may also need to be addressed. How can your volunteers be persuaded to continue their mission, when handling sick birds (and mammals) may soon become more dangerous? This question was also raised by hospital volunteer coordinators during the SARS outbreaks, and is sure to confront hospital volunteer coordinators even more forcefully if there is ever a severe flu pandemic. One key to keeping volunteers from quitting seems to be advance communication. Before H5N1 reaches North America, you should try to help your members learn enough about the risks to get through their initial “shock and awe” – so they remain a resilient resource when the time comes. And of course you should help them learn enough about the available precautions to feel that they can adequately protect themselves as well.
Proper training and equipment, plus imagining in advance what it might feel like to suddenly view birds as a danger, can help produce sturdy and appropriately cautious wildlife rescuers/rehabbers.
So you have three possible volunteer reactions to worry about: apathy, denial, and excessive fear. And there may be others. You can find out by talking with your members, asking them what they know, believe, and feel about the risk of catching avian influenza from infected wildlife. And remember, other countries are ahead of the U.S. in facing this problem. Learn what you can from the news coming out of bird sanctuaries and wildlife groups in the U.K.
(My wife and colleague Jody Lanard helped draft this answer.)
Measuring pandemic fear, panic, denial, and apathy
| name: | Fiona | |
| Field: | Communication specialist | |
| Date: | April 16, 2006 | |
| Location: | Canada |
Comment:
In advance of developing a pre-crisis flu pandemic internal communications plan, I am conducting some primary research. I intend to survey my target audience (all sworn emergency response members and civilian staff) to find out more about what they know and think about the pandemic issue, where they get their information (who influences them), what they would like more information on, how they want to receive that information, etc. I also want to gain a sense of their level of personal/family preparedness if any, and most importantly find out how concerned they are (or are not) about a pandemic.
You have written extensively about the “fear family of emotions” with apathy on one end of the spectrum and panic or denial on the other. To know which way to motivate my target audience with the communications plan, I need to know where people fall on the spectrum. I have some anecdotal evidence that in general people are insufficiently alarmed (either apathetic or willfully ignoring the issue) but I want substantiated evidence.
My question is: How is it best to find this out as part of a survey? What kinds of questions should I ask without being obvious? Or can I be obvious?
I would like to use the survey again over time to measure any improvements in the target audience's level of concern, level of preparedness, etc., so it is very important that I get the questions right the first time.
Peter responds:
Here are links to three surveys – one on pandemic flu and two on SARS – that may help you develop your own questionnaire. You’ll be interested in the survey results, I suspect, as well as the questions the authors used to measure their respondents’ level of concern/anxiety/fear.
- “Avian Flu Survey” (Harvard School of Public Health, January 2006) (Note that this survey does not always use clear terminology to show whether the questions refer to avian influenza that is occasionally transmitted from birds to humans, or pandemic influenza that may someday start spreading from humans to humans.)
- Quah, SR, and Lee, H-P, “Crisis Prevention and Management during SARS Outbreak, Singapore.” (Emerging Infectious Diseases, Centers for Disease Control and Prevention, February 2004)
- Imai, T, et al., “SARS Risk Perceptions in Healthcare Workers, Japan”
 (Emerging Infectious Diseases, Centers for Disease Control and Prevention, March 2005)
(Emerging Infectious Diseases, Centers for Disease Control and Prevention, March 2005)
The methodological questions you raise are a little daunting. I’m not sure I know the best answers – but you are definitely asking the right questions!
Particularly daunting is the question of how to measure denial as distinct from apathy. People in denial routinely claim to be apathetic; they have become “unconcerned” because they’re more frightened than they can bear. I’m confident pandemic apathy is currently a lot more common than pandemic denial, but it’s important not to miss the denial – especially since you plan to use your questionnaire to track reactions over time. And your mention of people who are “willfully ignoring the issue” certainly raises the hypothesis of denial. Apathetic people aren’t being willful. They’re just not worried.
The obvious way to distinguish denial from apathy is to try to arouse more concern/fear. If it works, people were apathetic; if it backfires, they were in denial, and have gone deeper into denial. (If it has no effect at all, it was presumably a weak message.) But obviously you’d like to identify denial without driving anyone deeper into it. I can’t think of a reliable way to do that. Sometimes it’s possible to get a whiff of denial if people become visibly more anxious (perhaps even while filling out your questionnaire) before they trip a mental circuit-breaker and become apparently more bored instead. But a whiff is a long way from “substantiated evidence.”
It would be interesting, and perhaps enlightening, to add a scenario – give people a graphic, two-minute description of 1918, perhaps – and ask how that makes them feel. This might be a not-too-intrusive way of exploring the possibility of denial. Genuinely apathetic people ought to experience some emotional arousal (if not fear, at least empathy) in response to an evocative description of the 1918 pandemic. People in denial dare not rise to the bait. At least that’s how I'd interpret these results – though the interpretation would certainly be debatable.
Except for the problem with denial, I do think it's okay to be obvious – that is, to ask people explicitly how they feel about the risk of a pandemic. There is certainly a long history of quantifying concern just by asking. I would try to distinguish people’s sense of the likelihood of a pandemic from their sense of how horrible it could be. And I might also ask how concerned they think their families, friends, and neighbors are. Whether you interpret this straightforwardly (as their estimate of other people’s level of concern) or psychodynamically (as a projection of their own concern), it’s worth knowing.
(Note: My wife and colleague Jody Lanard contributed to my answer to this question.)
Coming out of the closet about pandemic preparedness
| name: | Bill Furney | |
| Field: | Communication Coordinator, NC Office of Public Health, Preparedness & Response | |
| Date: | April 15, 2006 | |
| Email: | Bill.Furney@ncmail.net | |
| Location: | North Carolina, U.S. |
What I would add to this site:
I would like to see a section that addresses media witch hunts and/or political agendas. The death of the miners in West Virginia is an example of the former and Katrina hitting New Orleans is an example of the latter.
Even after the owners of the mines took responsibility and said that they made a mistake in their communications the media weren’t satisfied. They wanted the name of the person who misunderstood the report over the radio and caused the false announcement that the miners had been found alive to be made.
Katrina was even worse. Any facts about who might have been responsible for the failures of New Orleans were quickly lost in the media’s perpetuation of ideological battles. This bothers me greatly because I have no doubt that ANY shortcoming during a pandemic – predictable or not – will soon suffer the same onslaught of attack journalism. We need to be prepared.
Comment:
I’ve read your July 6, 2005 column "Superb Flu Pandemic Risk Communication: A Role Model from Australia" and was elated to find such a detailed breakdown of a good example of how to communicate the pan flu issue.
I would like to take Health Minister Tony Abbott’s approach one step farther and develop language that skips all the dancing and goes straight to the heart of the matter. In other words, I am looking for a good and proper way to tell the public that government cannot prepare for every eventuality associated with a pandemic, that people must be prepared to take some responsibilities, and that it is unrealistic to expect the healthcare system not to be overwhelmed in a true pandemic like Spanish flu.
Abbott comes close when he says, “There are obvious limits to how much governments can invest in preparations for hypothetical events, however serious. Still, responsible governments should make extensive preparations for reasonably foreseeable contingencies.” My concern is that this language does not acknowledge that it is a certainty that systems WILL be overwhelmed in a Spanish flu-type pandemic.
My plan is to mount a campaign that will address home care and preparedness, giving people action steps and reason to maintain calm and order. But I see it as absolutely essential to convey to the public that a pandemic on the scale of Spanish flu is something that cannot be totally accommodated by government or the healthcare system.
Peter responds:
There has been a lot of progress in the direction you’re recommending since Health Minister Abbott’s precedent-setting speech in Australia. In the U.S., HHS Secretary Leavitt and others have become more candid than officials usually are, acknowledging that a severe pandemic would overload the healthcare system; that the federal government cannot ride to the rescue when a crisis strikes everywhere at once; and that communities, neighborhoods, companies, civic groups, and individuals need to prepare to cope largely on their own.
Still, I agree with you that still more candor is called for. I’m especially dismayed by the continuing willingness of many officials to imply that vaccination is a likely deus ex machina. Even admissions that there may not be enough vaccine for everyone are grossly over-optimistic; it’s quite likely there won’t be any vaccine for anyone for some months. Local officials don’t help when they speak with pride about their ability to mass-vaccinate the population within days, without acknowledging that they don’t yet have anything to put into the needles.
Your focus on home care is also on target, I think. Part of getting ready for a pandemic is lying in bed at night trying to figure out how you would reorganize your household to take care of a very sick family member while minimizing the likelihood of infecting the rest of the family. Materials on home flu care do exist, but they’re not as widespread, as detailed, or as pandemic-oriented as they ought to be.
So the message you have in mind is a good message – that you can’t do everything for people in a severe pandemic, that they need to get ready to do as much as possible for themselves and for each other.
The trick is to make this message compassionate and regretful, in some cases even apologetic – not defensive or accusatory. Some government officials get to resenting people for having unrealistic expectations of the government and insufficient expectations of themselves. It’s an understandable feeling. But calling people irresponsible or overly demanding or ungrateful doesn’t do a lot of good. And it’s a little unfair as well, in the face of three realities:
- By routinely over-promising, officials have trained the public to expect everything to be taken care of for them.
- Meanwhile, the U.S. has allowed its public health infrastructure to decay for decades, so our response capacity is weaker than it should be.
- And in the specific area of pandemic preparedness, the U.S. was slow to respond and is still behind on some dimensions (antiviral stockpiles, for example).
You’re still right that a severe pandemic like 1918’s Spanish Flu would be beyond the capacity of any system. Still, the case for local preparedness, private sector preparedness, civil society preparedness, and individual preparedness needs to be made without rancor. The tone that’s called for, I think, is a mix of regret (we wish we’d done more at the federal and state levels), alarm (we may well face a catastrophe that will overwhelm all our systems) and determination (if we all do as much as we can to get ready, we will be that much better prepared to cope).
Whatever you do, post-pandemic recriminations are inevitable. “Why didn’t the government do more to prepare, so that it would be better able to cope?” “And why didn’t the government warn us more convincingly that we needed to prepare ourselves?” If we dodge the pandemic bullet, on the other hand, the recriminations will focus on how much money you wasted on unnecessary precautions, and how badly you scared us all for nothing. I don’t know of any way to avoid results-oriented blame: You should have known the pandemic would come/not come/be severe/be mild and planned accordingly. Warning people in ways that are impactful but not accusatory will help maximize their preparedness and minimize their inclination to blame you later. But you’ll still get blamed. Sorry.
Risk communication seminars
| Name: | Jennifer Pflugfelder |
| Field: | Corporate communications |
| Date: | April 15, 2006 |
| Email: | jpflugfelder@ssg.petsmart.com |
| Location: | Arizona, U.S. |
Comment:
I wasn’t able to find a list of upcoming seminars on your web site. Is this something you can make available as I’m looking to book a 2006 conference?
Peter responds:
For a long time I had a policy of not posting any information on presentations I was giving, because I didn’t want this site to look promotional. I changed my mind a few months ago, and decided I would announce presentations that met three criteria: (a) Registration is open to the public; (b) Registration is available online; and (c) The presentation is at least a half-day seminar, not just a short speech.
Two March events (one in Florida and one in California) met those criteria. The links were posted on my home page until the events were over.
The only event currently on my calendar that meets the criteria is September 28 in Washington, DC. It’s a one-day crisis communication seminar, sponsored by the Public Affairs Council. I’ll post it over the summer. But if you want to know about it now, check out www.pac.org/crisis.
If something comes along sooner that meets the criteria, I’ll post that too.
More on Tamiflu stockpiling ethics and psychology
| name: | Caia | |
| Field: | Occasional blogger | |
| Date: | March 10, 2006 | |
| Location: | Massachusetts, U.S. |
Comment:
Thank you for your excellent article about Tamiflu stockpiling and the specious arguments against it. I feel rather foolish; I parroted that line about “inappropriate use increasing resistance” in a post I made about bird flu. It didn’t make complete logical sense to me, but I’m a former English major, not a scientist. It somehow didn’t occur to me that supposedly authoritative sources (or journalists) would just make that up. I suppose my cynicism about the official response to bird flu has been inadequate.
A thought about last year’s flu vaccine: Some people did voluntarily give up a shot. I did. Because I have a chronic illness, my doctor informed me I did qualify despite the shortage, and was surprised I turned it down.
My reasoning was that I wasn’t terribly likely to catch the annual flu, being out of college, not being around kids much, and not working with the public. But more importantly, while my chronic illness may have qualified me to get a flu shot, it’s not one that I’ve ever learned causes respiratory illnesses to be more dangerous. It might suck more for me to have the flu than a healthy person, and take me longer to recover, but it was unlikely to kill me. I thought of my grandfather, aged 93, and responded to the suggestion I get a flu shot some old person or some baby needed more with outright incredulity.
I’m no saint. If I’d thought I were at any more risk of dying than a healthy young adult, I would have gotten the shot.
And that leads me to some indecisiveness about Tamiflu. I’d pretty much decided not to stockpile any, perhaps as much because I feared gentle rebuke or dismissal from my doctor as anything else. I still feel like that’s the right decision. I’m not at particular risk of contracting a possible pandemic flu; I have masks and gloves and plans to go home and stay. I’m taking steps to minimize my risk. Surely someone else will need it more than me.
But now I’m worrying, because as a young adult I may be more at risk, if this pandemic turns out like 1918. I don’t know if my having an autoimmune illness makes it even more likely that I would develop a cytokine storm response. I don’t know if anybody knows that right now. It’s one thing to think about stockpiling Tamiflu and not getting sick, thus having the drug go to waste when it might have saved someone. I think, “I wouldn’t be able to live with it.” Sounds like the end of the discussion, doesn’t it? But it’s another thing to really consider that I might not be able to live without it. I’m no saint, so the decision isn’t so easy.
And maybe that’s part of why some doctors and public health officials produce phony reasons against personal Tamiflu stockpiling. They may be emotionally necessary rationalizations. They’re not just scientists and physicians, they’re human beings. As you said, the logic that the greater good is better served if the government has all the Tamiflu is hard logic. If the public health officials have decent imaginations, it must be very hard indeed for them to embrace, knowing it may mean tens upon tens of thousands of deaths for those not prioritized. The more they know about the possible effects of a severe pandemic, the harder it may be for them to come to terms with that math, and with themselves as the ones doing the calculations.
And the doctors may have it even worse, because they care about, as well as for, their patients. “Sorry, I'm going to have to let you suffer and perhaps die because you’re not that important to society”? How many want to say that? How many can accept that that may be the reality of their decision, especially with the unspoken reality that they themselves ARE that important to society, and so will be high on the list to be saved? They may have to believe that the requests for Tamiflu are misguided, and belittle them, in order to allay their own guilt, even if they believe they are acting ethically, for the greater good.
None of this is to say that their obfuscations and outright falsehoods are good public policy or serve their own interests in the long run. But it goes a long way towards explaining.
Peter responds:
I really like your point that public officials and doctors probably aren’t trying to be devious when they advance invalid arguments against Tamiflu stockpiling. They may simply be trying, unconsciously, to avoid the pain of seeing others as “not worthy” of protecting with a scarce medication.
As you say, belittling people’s reasons for wanting Tamiflu, and inventing specious reasons why they shouldn’t want it, isn’t good public policy – or good risk communication. But it certainly becomes more forgivable when we see it as a human response to feeling guilty about Tamiflu rationing. Your last few paragraphs are thus an important addendum to your first paragraph, which was rather more cynical, maybe even a little angry.
As for the way you are thinking (and feeling) through your own moral dilemmas about whether to get an annual flu shot and whether to stockpile Tamiflu, I have nothing to add – except to thank you for sharing a very good role model. Well, maybe one thing to add: “The choice isn’t easy” and “both answers have merit” are equivalent statements, at least in this case. Having reasoned carefully to the conclusion that there’s a lot to be said for either option, it may be time to focus more on which one appeals. Which feels right? Which sits better? That may make the choice a bit easier.
Message points for a pandemic flu school flyer for parents
| name: | Nancy | |
| Field: | Writer, editor, volunteer activist | |
| Date: | March 10, 2006 | |
| Location: | New Hampshire, U.S. |
Comment:
I have permission from our elementary school principal to prepare a series of pandemic awareness/education handouts that will go home to approximately 600 families in the weekly notices packets. It may be distributed at the middle school and high school as well, and it is possible the effort will be rolled out on a regional basis. I consume (and digest!) a vast amount of H5N1 information daily. I have so much information, I don’t know where to begin.
I believe the first of these notices is going to be the most important. If it fails to capture the imagination of the audience, the rest will be ignored.
I am not a trained risk communicator. That said, I could use some guidance from you and Jody. Specifically, how many topics do you think I should introduce in the first handout (8.5" x 11" double-sided), and what information would you consider essential to convey? I think less is more and will keep the word count under 1,000.
I am thinking the following:
- Why we are communicating to families at this time?
- Define pandemic.
- Identify current issues of concern.
- Introduce the concept of preparedness.
- List local, state, and federal resources families can go to for more information.
- Preview what will be in the next flyer.
Is this too much? The wrong focus? Too little?
I am also wondering whether it is appropriate to send this information home with the children. It will be inserted into a packet that goes home with the kids every week. Most kids don’t even look at it as the info is for parents. However, some of the older kids do flip through the packets. I don’t want to scare them and raise the ire of parents.
Peter responds:
You already got a lot of good help on this question from the “Effect Measure” public health blog. Readers who want to check it out should look at the March 7, 2006 post entitled “Three points about bird flu to tell others.” Read the main post by “Revere” first. Then read the comments, which start with Nancy’s question.
I agree with the consensus that you should aim for a foot-in-the-door, not overwhelm your not-yet-very-interested audience with everything you know. Vincent Covello advises that risk communicators should always stick to three points, and support each point with three pieces of supporting evidence. I’m not sure three is a magic number and four is the kiss of death. But whether it’s the number of main points or the number of supporting facts, three or four is surely better than 30 or 40 in a one-page flyer! I feel like something of a hypocrite giving this advice, since so much of what I write goes on and on (and on). But it is good advice nonetheless.
The three main points Revere lists in his “Effect Measure” post make sense to me: (1) We can’t stop a pandemic if the biology of the virus moves that way; (2) In a serious pandemic every community will be pretty much on its own; and (3) There’s a lot of preparing to be done that isn’t about medicine or public health.
I also agree with Revere’s comment on San Francisco’s 1918 experience, as documented by John Barry: A community that is psychologically prepared and not over-reassured can get through the catastrophe better than a community that’s caught flat-footed and told not to worry. I’m not sure that’s a message for parents, but it’s certainly a reason why what you tell parents needs to be sobering and even alarming. (As for whether the kids can bear to hear the bad news too, see two 2005 Guestbook entries: “Giving children frightening bird flu information” and “Risk communication for children.”)
In talking about Revere's third message – there’s preparing to be done – I would certainly mention a few things parents can do at home to get their households better prepared. (And I’d tell them where to go for longer lists.) And as Revere points out in his later response to you, the first flyer should say something about school preparedness, especially the dilemma of when/whether to close the schools. Ideally, the flyer would invite parents to help develop a school (or school system) pandemic preparedness plan. This may go way beyond anything your principal will let you send home with the kids – but I’d aim in that direction. A school flyer warning parents about a pandemic but saying nothing about the state of school system pandemic planning is bound to sound a little hollow. At least promise to address the issue in a later flyer … and then take it up with the School Board.
Finally, a fourth message: It’s not about the birds. Many of your students’ parents have been watching, hearing, and reading news about a “bird flu pandemic” that could be incredibly dangerous. And they have learned that bird flu has already made it from Asia to Europe and is probably headed for North America. Understandably, many of them equate the pandemic risk with dead birds. This systematic confusion of bird flu and pandemic flu is a serious problem. People become excessively worried when local birds get sick (which is very bad for chicken consumption). Worse, they remain insufficiently worried so long as local birds aren’t sick.
The H5N1 catechism:

- Bird flu or avian influenza is a disease among birds. A very small number of people have caught it, nearly all of them from sick or dead birds. But it takes intimate contact and very bad luck for a person to catch bird flu. (Birds catch it easily.) Even so, close contact with a sick bird or a bird that might be sick ought to be avoided. Eating a well-cooked chicken is safe even if the chicken had bird flu. But the person who cooked the chicken took some risk – as would a cat that ate it raw. Still, all of these risks are currently very small. They’re close to zero for people who have no contact with sick or dead birds.

- Experts are worried that the novel strain of bird flu called H5N1 might mutate in a way that gives it the ability to pass more easily from birds to humans, and from humans to humans. Since people haven’t had H5N1 before, there is no natural resistance and no established vaccine. If H5N1 (or any novel bird flu virus) “learns” how to pass easily to and among humans, the virus would inevitably spread worldwide. This is called a pandemic. It might be mild. Or it might be severe and kill tens of millions or even hundreds of millions. A pandemic will result if the virus starts spreading easily among people anywhere in the world. It will be spread by travelers, not by birds. It will afflict people worldwide, regardless of whether local birds do or do not get bird flu.

- Bird flu is thus a very small human health risk, pretty much confined to people who have contact with sick or dead birds – though it is a catastrophe for the poultry industry. Pandemic flu is a possible huge risk to public health – but there is no pandemic flu right now. The two are connected in that it will take a bird flu mutation to launch a pandemic. Once that mutation happens, if it ever does, thereafter it’s not about the birds.
Yes, I know, that’s too much information for just one point on a one-page flyer. And telling people it’s not about the birds probably isn’t as important as getting them hooked on household, school, and community pandemic preparedness. Still, it would be a big step forward if people knew it’s not about the birds – and knew it before the spring migration reaches our shores.
Just-in-time pandemic preparedness
| Name: | Stewart |
| Field: | Educator |
| Date: | March 10, 2006 |
| Location: | Arkansas, U.S. |
Comment:
I guess I have been consumed by the avian flu since first hearing about it. I just check updates on it daily.
I am a concerned educator and parent of a two-year-old. My question is: Trying to avoid over-reacting to this recent flu scare, what are some signs that might come that would indicate now it is time to prepare (purchasing Tamiflu, stockpiling, and such) and beat the government and general public to the punch?
Peter responds:
The U.S. government is already paying serious attention to pandemic preparedness. So are most of the world’s governments – though many of them don’t have the resources to do much, and no government is doing as much as they’ll all wish they’d done if and when a pandemic materializes. More and more individuals are also taking pandemic preparedness seriously.
So it's a bit late to talk about beating them to the punch. Still, once a pandemic is obviously imminent (if that time ever comes), the competition for supplies will be fierce. The resulting instant scarcity will make just-in-time preparedness a bad bet – even if it weren’t an oxymoron to begin with.
The time to prepare is now. I don’t mean to imply that the past few weeks of news from Europe have significantly changed the situation. The odds that the H5N1 virus will “learn” efficient human-to-human transmission doesn’t depend very powerfully on how many European countries have found some dead swans or cats or chickens. Some experts do see recent signs of increased pandemic risk. Some don’t. And I’m not an expert. Before H5N1-positive birds and cats started turning up in Western Europe, I already thought the time to prepare was now.
That doesn’t necessarily mean you should drop everything and focus your life on pandemic preparedness. It certainly hasn’t meant that for me. Increase your purchases of long-lasting foods that don’t require refrigeration, and slowly build a “revolving stockpile” that will keep your household going for 4–6 weeks if needed. Talk your doctor into prescribing some extras of the medications you can't do without, then grit your teeth and fill the scrips even though your insurance company probably won’t cover the cost. Get some Tamiflu if you can – and if you think it’s likely to work, and if you feel okay about there being that much less Tamiflu available for high-risk people who get the seasonal flu.
Make your own shortlist of pandemic precautions worth integrating into your life. You don’t know if the pandemic will start tomorrow, a year from now, ten years from now, or never. Don’t assume it’s tomorrow and distort your life unbearably. Don’t imagine it’s never and postpone your preparations indefinitely.
Outrage management and school-parent relations
| Name: | Pamela Dean |
| Field: | Head of an Episcopal school |
| Date: | February 20, 2006 |
| Location: | Texas, U.S. |
Comment:
One of my Board members sent me the link to “It’s The Outrage, Stupid.” Your principles and procedures for dealing with outraged consumers cross into all areas of our culture today.
I just had a meeting with a group of mothers today about headlice. Sound trivial? Not to moms. Two of them were gathering together people, calling for a petition that would go to the Board because of a lice outbreak at our school.
I asked one of those moms to gather information for us and I set up a meeting time to discuss our procedures and share ideas for improvement. We had ten people come. We ended up with an improved procedure and consumers who knew they were heard and could effect change.
After almost 20 years administrating private schools, I’ve learned the hard way to follow the steps you’ve so carefully listed. I’m going to share your advice with my staff, as they deal with parents of children in their rooms. It’s all about communicating, isn’t it?
Peter responds:
Thank you for the testimonial. For more articles on outrage management strategies, check out the website’s Outrage Management Index. But I have to say it doesn’t sound like you need it!
Risk communication versus media relations
| Name: | Barbara |
| Field: | Public health risk communications |
| Date: | February 20, 2006 |
Comment:
I am interested in your thoughts about how risk communication fits with the art and science of media relations. CDC combines the two as if they are entirely compatible. I am hearing that people who are considered public information officers, at least in local and state government settings, consider their roles to be media relations.
I see media relations as a tool in the broader scope of risk communication. In the end, I’m not sure that PIOs are the best people to do the risk communication that public health needs.
Peter responds:
Media relations people are experts on dealing with the media – on how to get your press release printed or your video news release broadcast; on how to manage a successful interview; on how to set up a news conference that will attract reporters and yield positive coverage. The care and feeding of journalists is what they do.
Of course the care and feeding of journalists isn’t a goal. It’s a means. The payoff of good media relations should be media content that affects the audience – the public – the way you want it to: content that provides the information you want people to know, inculcates the attitudes you want people to have, and motivates the actions you want people to take. We used to call it public relations. But as P.R. took on a slightly bad odor in people’s minds (even P.R. people’s minds), we came up with new terms. “Public information” is one – implying that you don’t actually care what people think or do as long as they're accurately informed. “Media relations” is another.
Risk communication is talking with people about bad things that might happen – how likely the bad thing is, how awful it could get, what precautions people might want to consider taking (or how unlikely it is, why it wouldn’t be so awful anyhow, why precautions aren’t necessary). A lot of risk communication does take place via the news media. How else are you going to tell millions of people about pandemic preparedness, or global warming, or water pollution? A lot of risk communication takes place via non-news media, media with no journalist between you and your public – from websites to pamphlets. The very best risk communication is small-scale and interactive: one-on-one conversations and small public meetings.
Even when they’re working in a one-way reporter-mediated medium, risk communicators worry about different issues than other communicators. How alarming or reassuring should you be? How confident or tentative should you sound? How do you deal with people’s fear, anger, and other emotions? How do you involve people in your organization’s risk management decision-making and help them make their own risk management decisions? How do you talk about risks that are technically not very serious but nonetheless emotionally compelling? How do you talk about risks that are not very compelling but nonetheless deadly?
A skilled risk communicator may or may not also know how to write a release and run a news conference. A skilled media relations person may or may not also know how to frame a risk comparison and listen to a frightened neighbor. What matters, obviously, isn’t what job title people have, but what set(s) of skills they have.
When I was in graduate school in the late 1960s, there was considerable debate over whether P.R. people needed special schooling in P.R., or whether any good journalist could cross over from covering the news to dishing it out. Marketing and advertising were already considered communication disciplines that required a specialized education; they had a strong science component along with their craft component. But P.R. was nearly all craft, as was journalism. Today, journalism is still nearly all craft. But most corporations distinguish their P.R. practitioners (who have mastered the craft, and may well be ex-journalists) from their P.R. strategists and policy-makers (who have studied such arcane matters as the dynamics of public opinion and the relationship between attitudes and behavior).
Governments have been slow to make this transition. The average state or federal health agency probably has a couple of people with Ph.D.s in things like health education or social marketing or even risk communication. But they’re not usually in the public information office – which is typically staffed, still, with ex-journalists.
Of course there’s nothing to keep an ex-journalist from learning risk communication. Dick Thompson at the World Health Organization did, for example. And some ex-journalists just have good instincts, even for risk communication. But too many are proud of their craft and suspicious of those egghead “communicologists.” Too often they write good news releases and stage good news conferences, but don’t know how to talk about risk with a citizen who is frightened, angry, or apathetic – and don’t even know there’s a field there worth knowing.
Doctor-patient risk communication: persuasion or just the facts?
| Name: | John Paling |
| Field: | Speaker and consultant on communicating risks |
| Date: | February 20, 2006 |
| Email: | john@riskcomm.com |
| Location: | Florida, U.S. |
Comment:
I am delighted to announce the availability of my book, Helping Patients Understand Risks. For detailed information, please see http://www.riskcomm.com/hpur.htm.
The book started out as an extended handout for my lectures and conference presentations and is intended to appeal to busy physicians in all branches of the profession rather than the specialists who focus on communication research.
The book points out that, unlike other professions that communicate risks to the public (where only a few people are entrusted with the task and they are carefully trained), in healthcare virtually all clinicians do it and virtually none of them has received any training. Consequently, I believe that the way doctors and healthcare agencies currently explain risks to patients has the potential to work against patients’ best interests. In response, the book offers several simple strategies that healthcare professionals could adopt – including visual aids that show the risk (frequency) numbers from both the negative and positive perspective at the same time.
Peter responds:
Helping Patients Understand Risks was a good read. I like your breezy style, your visual aids (especially the palette), and your very convincing argument about why patients find relative risk too confusing for doctors to use. (A treatment that reduces some risk from two-in-a-million to one-in-a-million cuts the relative risk by 50%, while it cuts the absolute risk by one-in-a-million. The former fact is likelier to mislead than enlighten.)
You’ve put some of the most important basics of risk communication in a form that is easy to digest and use, yet true to the research and theory base from which you've drawn.
It would be interesting to add some material specifically on the doctor's goal – what difference does it make whether the doctor is trying to help the patient see how dangerous something is (e.g., why you should quit smoking) versus how safe something is (e.g., why you shouldn’t worry too much about these side effects) versus both at the same time. Some of what you’ve written seems to assume that the problem is patient overestimation of medical risks, that the doctor’s goal is to meet the informed consent obligation without unduly scaring the patient. But that’s only one of the problems. Sometimes the goal is to duly scare the patient about lifestyle choices that are far more dangerous than the patient supposes.
john replies:
Perhaps I am totally naïve in defining the doctor’s “goal.” I have always seen the professional’s goal as making the facts available to the listener/patient in a way that is as neutral as possible. In my own work, I consciously strive to be transparently trustworthy – and not gently paternalistic – partly in the hope that listeners will feel that they trust me totally and, as a result, that they will be open to actually “hear” the evidence-based data in context.
Subjectively, I feel that trustworthiness is the strongest of your outrage factors. By striving always to show that I am not untrustworthy, I hope my audience will be less likely to filter out my message and less likely to significantly distort the science through your other outrage factors.
If I understand your position, you seem to feel that the professional should use our knowledge of outrage etc. to color the communication, such that the patient’s response is moved towards the patient’s (or society’s) best interests.
Perhaps you are the experienced pragmatist and I am the idealistic neophyte. Perhaps I am like a newspaper reader who idealistically expects objective reporting when the very process of selection and presentation style inevitably produces an editorial slant. My goal might be naïve, but I still think that, in many medical situations, the doctor cannot know best because the consequences side of the equation is heavily weighted by patient values.
peter replies:
I believe that persuasion goals are just as compatible with trust as information goals – as long as they’re not hidden or disavowed.
I have no quarrel with a communicator who simply wants to convey information and doesn’t care what use the receiver makes of that information. But as soon as the communicator cares – as soon as the doctor really hopes the patient will quit smoking or agree to surgery or whatever – then it is destructive to trust for the doctor to pretend otherwise. The communicator’s obligation under those circumstances is twofold: (a) To acknowledge his/her goal=bias=stake. (b) To be scrupulous about not excluding or understating information that might support an opposing conclusion.
A good communicator with Goal X and a good communicator with Goal Y will say somewhat similar but not identical things. A poor communicator with Goal X and a poor communicator with Goal Y will be further apart in what they say – underestimating the effectiveness (and ignoring the ethics) of giving the other side its due. The communicator I trust least is the one who pretends (or imagines) that s/he wants merely to inform me, while I suspect that s/he has a preference about what conclusion I end up reaching.
I actually believe in persuasion. I think doctors really should care what decisions their patients actually reach. Moreover, I think they do care. If so, they need to own their bias. Figuring out what works and what's ethical is tougher once the doctor abandons the assumption of indifference – but everything until then has an element of deception (and an element of self-deception) in it.
john replies:
Then you would advise a doctor to always answer when a patient asks, “What would you do, doc?”?
My understanding is that where the choice is not strikingly obvious (cigarettes), doctors are taught to say something like, “Well, I really can’t decide for you but here are the issues you should consider….”
peter replies:
I think the doctor’s answer should depend on how debatable the doctor believes the decision is, and how strongly the doctor feels s/he knows which decision is best for the patient. But all answers should acknowledge both the patient’s autonomy and the doctor’s opinion (if the doctor has one).
Thus:
- “I don’t know what I’d do in your shoes. It’s a really tough decision. Here are the reasons to do X, and here are the reasons to do Y….”
- “It’s a debatable decision, and neither choice is foolish. If it were up to me, I think I’d do X, for these reasons…. But there’s also a case for Y. Another doctor might even recommend Y, for these reasons….”
- “I think the case for X is a lot stronger than the case for Y. Here’s how I assess the pros and cons of each…. I think most doctors would recommend X, as I do. But not all, and in the final analysis it’s your decision.”
- “Medically, this just isn’t debatable. X is a sounder choice than Y, for these reasons…. I really hope you will decide to do X. I think Y would be a serious mistake. But of course the decision is yours, and I will still be your doctor even if you decide to act against medical advice.”
The answers I don’t like:
- “My opinion is irrelevant. I’m not you. I don’t want to tell you what I think because it might bias your decision.”
- “Do X. Sign here.”
Note: John Paling has written an extended response, which is posted on this site.
Outrage about risk to the elderly
| name: | Ricardo Morales | |
| Field: | Chemical engineer in government | |
| Date: | February 20, 2006 | |
| Email: | ricardomoralescr@yahoo.com | |
| Location: | Costa Rica |
Comment:
I agree with the idea that risks affecting children are perceived as more “risky.” Have you encountered this perception to be true also when the elderly are involved? We have, in the case of electromagnetic fields!
I would like to hear more comments to know how generalized this perception of mine is.
Peter responds:
Most lists of what I call “outrage factors” include something like “effect on vulnerable populations.” The theory is that there will be more outrage – more concern, more fear or anger, more inclination to take action – when a risk endangers children, the elderly, the handicapped, or the sick than when it endangers healthy adults.
Societies obviously differ some in their attitudes toward these various vulnerable groups. There are many cultures in the world that have traditionally revered their elderly. In the United States, I believe, the urge to protect children is much stronger than the urge to protect other vulnerable populations.
We are especially ambivalent about the elderly. On the one hand, some of the most horrifyingly vivid images emerging from the Hurricane Katrina disaster were images of elderly people left to die alone in upstairs rooms or on rooftops, or left to die en masse in a nursing home whose staff abandoned their patients and fled the premises. On the other hand, we seem to care very little about the 35,000 elderly Americans who die every year from the seasonal flu, many of whom could be saved by a more aggressive annual vaccination campaign.
This ambivalence shows up in professional debates over how to measure the mortality from any risk. Simply counting the number of people who die treats the elderly as neither more nor less important than their children and grandchildren. Counting “years of life lost,” on the other hand, treats the elderly as less worth saving than young adults, who are in turn less worth saving than children (who “have their whole lives in front of them”). The fight between these two standards has been ongoing for decades among U.S. risk assessors. I know of no risk assessment methodology that “overvalues” the elderly the way the years-of-life-lost standard undervalues them.
There are times when Americans do seem willing to sacrifice young lives for the sake of older ones – or even to sacrifice the lives of people of all ages for the sake of taking a protective stance toward the elderly. Consider our confused thinking about a possible influenza pandemic. Many countries have announced that in a severe pandemic, the limited supply of antivirals would be allocated primarily to healthcare workers, cops, and others whose skills were needed to keep society running during the crisis. The United States, on the other hand, has avoided this rational but (some say) hard-hearted decision. Or at least it has avoided announcing such a decision, or discussing its pros and cons. U.S. leaders continue to talk about providing Tamiflu to the most vulnerable segments of society. Most often mentioned are the elderly and the immunocompromised.
Yet when I go to pandemic preparedness conferences, one of the facts that most strike fear into the hearts of those attending is that the 1918 Spanish Flu pandemic killed lots of healthy young adults – and that H5N1 is so far doing the same thing. The seasonal flu kills mostly children and the elderly. That should make it a particularly terrifying disease, if we were especially outraged by threats to vulnerable populations. It doesn’t seem to work that way. Instead of the typical U-shaped curve for flu deaths, the 1918 pandemic had a W-shaped curve. In addition to killing children and the elderly, it also struck a high proportion of healthy young adults, turning their strong immune systems against them. That threat to not-so-vulnerable populations seems to be part of what’s terrifying about the prospect of a pandemic.
We really do want to protect our elderly and other vulnerable populations. We are willing to sacrifice to do so. This willingness is especially strong when we’re looking at specific, identifiable vulnerable individuals. It weakens when we’re talking more theoretically, when the vulnerable populations are statistics rather than people (or at least video). And it pretty much disappears when we become aware that not-so-vulnerable populations are threatened too. We want to sacrifice for the elderly vulnerable from a position of comparative invulnerability ourselves.
We will reach out to help our elderly, but when push comes to shove we won’t die for them. We will die for our children.
That’s how it looks to me in the U.S. It may be different in other parts of the world. (And it may look different to me when I’m 80 instead of 60!)
Surgical masks: Another pandemic risk communication controversy
| name: | Kay | |
| Field: | State health agency risk communicator | |
| Date: | February 9, 2006 | |
| Location: | U.S. |
Comment:
I just finished reading your Tamiflu stockpiling column and I couldn’t agree with you more. It’s a relatively clear dilemma – should you stockpile Tamiflu in case of a pandemic, or should you be a “good citizen” and do what’s best for society? I personally have not stockpiled Tamiflu. But months ago I advised my daughter and her family (in fact, all my family members) to run – not walk – to their doctor for a Tamiflu prescription. I know the government won’t be able to protect them in a pandemic. But as a mother, that’s my job. If another mother fails to do her job, it’s a shame. But I’ll do what I can for MY kids.
Having said that, I also am concerned about the message being sent about masks. Our scientists are saying we absolutely should not advise people to stockpile surgical masks in case of a pandemic. Why? Because there’s “no evidence they work to prevent transmission of influenza in non-medical surroundings.” Several questions arise.
(1) If surgical masks don’t work to prevent transmission of influenza when worn by the general public, why do pandemic plans advise health care workers to wear them in any interaction with patients with flu-like symptoms? Isn’t that a much higher-risk setting than just being out in public? If mask use is indicated for a high-risk setting, why wouldn’t it be helpful in a lower-risk situation?
(2) Is there really evidence that masks don’t help prevent influenza transmission, or it is just a case of no studies having been done? (Bet it’s the latter.)
(3) If masks aren’t indicated for prevention (e.g., for you and me to wear when we’re healthy but have to ride the subway shoulder-to-shoulder with people who are coughing and sneezing), why are they indicated for the people who are coughing or sneezing? To simplify – if a mask keep their germs IN, why won’t it keep their germs OUT?
(4) If the concern is that people who wear masks will later self-inoculate their mucus membranes after they touch contaminated items or surfaces, or while taking off their own mask, isn’t that a matter that can be addressed by hygiene education? What does it have to do with whether wearing a mask is a good idea in a pandemic?
(5) The experts are saying that we will run out of masks in a pandemic and that there likely will not even be enough for health care workers. If that is anticipated, doesn’t it make sense to conclude that people WILL want masks (and will make their own ad hoc versions, if necessary)? So why not advise people to stockpile them now, explaining honestly about their benefits and limitations and educating people about how to optimize their use? If we start to run short, manufacturers will make more. That’s supply and demand. But if we keep downplaying mask use, and run out when we most need them, will we again “scold” people for putting their individual needs ahead of society’s?
(6) If there’s no evidence that masks help prevent influenza transmission when used by the general public, why haven’t studies been done to find out one way or another? Does anyone remember SARS? People wore masks! It’s been a while – what’s everyone waiting for?
Bottom line: The experts say masks really aren’t helpful. Hand-washing is overrated. Most of us have no chance to get vaccine or Tamiflu.
“Don’t hoard Tamiflu in advance,” we are told. “There are people who need it more than you. We will give Tamiflu only to pandemic patients who are admitted to the hospital.” But we don’t want the “worried well” inundating the hospitals, so we have to develop some risk communication messages to convince them to stay home unless they’re really sick. Of course, if we are successful at keeping them away from the hospital until they are really sick, it will be too late for Tamiflu to do any good.
What’s a risk communicator to do?!!!
Peter responds:
This response was written jointly with my wife and colleague Jody Lanard M.D.
There are three fundamental issues here – and they all apply to a lot more than the surgical mask controversy:

-
What does “sound science” tell us, and are health officials consistent in deciding when to rely on intuition and when to stick to the evidence?
Infectious disease experts often discourage amateurs from taking precautions that are not evidence-based.
- This is reasonable when the scientists are advising against far-fetched, possibly dangerous precautions, especially if people are prone to take them instead of potentially more useful precautions.
- It is less reasonable when they’re advising against precautions that common sense (and the little evidence that’s available) says probably do some good and virtually no harm.
- It is least reasonable when they’re simultaneously endorsing other precautions that are similarly supported more by intuition than by data.
The same people who insist there’s no convincing evidence that mask-wearing by the public helps reduce the transmission of influenza also urge people to cover their mouths when they cough. Only when pressed do they concede there is not much evidence on behalf of that either. But the “experts” get to decide when they want to recommend things even though there’s no supporting evidence, and when they want to recommend against things because there’s no supporting evidence.
Not to mention that a mask does cover your mouth, and may keep you from touching your face (also widely recommended) – and it does so a lot more efficiently than a tissue or a sleeve when you’re standing on a bus holding the strap with one hand and your possessions with the other. At least until most people are wearing them, masks also increase social distance (try wearing one in public and watch the distance increase), which is universally agreed to be useful in reducing contagion.
Yet most health officials say people shouldn’t plan to wear masks in public during a flu pandemic. There must be something about the public wearing of masks that strikes terror into the hearts of officials and experts.
But this apparent terror is slowly morphing into a degree of acceptance. The CDC’s current “Cover your Cough”
 page starts out advising you to “cover your mouth and nose with a tissue when you cough or sneeze or cough or sneeze into your upper sleeve, not your hands.” But then the instructions add: “You may be asked to put on a surgical mask to protect others.” The CDC is not yet ready to concede that it might make sense to wear a mask to protect yourself as well as others (though that is what doctors and nurses do), nor that you might want to do it without being asked. Still, there’s progress.
page starts out advising you to “cover your mouth and nose with a tissue when you cough or sneeze or cough or sneeze into your upper sleeve, not your hands.” But then the instructions add: “You may be asked to put on a surgical mask to protect others.” The CDC is not yet ready to concede that it might make sense to wear a mask to protect yourself as well as others (though that is what doctors and nurses do), nor that you might want to do it without being asked. Still, there’s progress.More progress is reflected in a literature review written by the World Health Organization’s “Writing Group” and published in the January 2006 issue of the CDC’s own Journal of Emerging Infectious Diseases. The “Hygiene and Disinfection” section notes:
Recommendations for “respiratory hygiene/cough etiquette,” such as covering one’s mouth when coughing and avoiding spitting, have been made more on the basis of plausible effectiveness than controlled studies (32). As summarized in part 1 of this article, influenza virus can remain viable on environmental surfaces and is believed transmissible by hands or fomites (3). Most, but not all, controlled studies show a protective effect of handwashing in reducing upper respiratory infections (Appendix 2). Most of the infections studied were likely viral, but only a small percentage were due to influenza (33). No studies appear to address influenza specifically.
In other words, there is no hard evidence that covering your mouth when you sneeze or coughing into your sleeve reduces influenza transmission. And there is only the slightest hint of hard evidence that hand-washing does so. Nevertheless, these are widely and officially recommended methods of reducing the risk of flu transmission. What the WHO Writing Group calls “plausible effectiveness” translates in plain English into common sense.
The same article presents an extremely tentative retrospective finding that surgical masks worn in public during the SARS outbreaks in Hong Kong was one of a group of precautions that collectively reduced influenza transmission – though there is no proof it was mask-wearing that did the trick:
Influenza and other respiratory viral infections apparently declined in Hong Kong during the 2003 SARS epidemic, as determined on the basis of a review of viral diagnostic laboratory records (20). Public health interventions included closing schools, swimming pools, and other public gathering places; canceling sports events; and disinfecting taxis, buses, and public places. A high percentage of people wore masks in public and washed hands frequently, and in general, much less social mixing occurred.
The real breakthrough comes in the article’s “Discussion” section, where the authors treat mask-wearing with unusual respect:
WHO has recommended that mask use by the public should be based on risk, including frequency of exposure and closeness of contact with potentially infectious persons; routine mask use in public places should be permitted but not required. This recommendation might be interpreted, for example, as supporting mask use in crowded settings such as public transport.
If public mask-wearing is going to be recommended (or at least tolerated) during a pandemic, it follows that public mask-stockpiling ought to be recommended (or at least tolerated) beforehand. We aren’t aware of any current surgical mask production bottleneck, nothing analogous to the Tamiflu rationing dilemma. Of course once a pandemic has begun there are likely to be mask shortages, like the ones hospitals in other countries experienced during SARS. As you point out, that’s all the more reason to stockpile masks now, stimulating the demand and thus reducing the likelihood and severity of future shortages.
Mask-wearing isn’t a panacea, of course. Dr. Alison McGeer, a Canadian infectious disease specialist (and excellent risk communicator) who survived her own case of SARS, said in a recent interview for the CBC-TV show “Black Dawn” that “one of the consequences of wearing a mask – particularly for those of us who don’t usually wear masks – is that it draws your hands to the face. If your hands are not clean, and you keep putting your hands up around your face, you may actually increase the risk that you might get influenza despite the fact that you’re wearing a mask.”
No precaution is a panacea. As your comment rightly says, the solution is hygiene education – to try not to fiddle with your mask; to cough or sneeze into something that can trap most of the droplets; to wash your hands as soon as you get to your destination after riding on public transport; to remember to turn off the public washroom sink with a paper towel.

-
Why are officials and experts so often contemptuous of precautions the public finds appealing?
Here is one Q&A from the State of Delaware’s official website page on “Avian Flu FAQs”:
Q. Would you recommend that Delawareans wear breathing masks when in public? Should travelers use breathing masks outside the United States?
In the case of a pandemic, we would not discourage any activity that limits the spread of the virus no matter how ineffective as long as these activities are safe. At this time, in the absence of a pandemic, there is no need to take … precautions against H5N1.Well, at least they said it was okay to wear a mask, “no matter how ineffective.” But the answer positively drips contempt. Compare it to this excerpt from Delaware’s website on “regular” flu:
How to Prevent the Spread of Influenza
DPH recommends residents take the following steps to prevent viral illnesses and relieve symptoms should they occur:
Cover your mouth when coughing or sneezing….
We cannot fully explain the tone of ridicule and disdain that frequently accompanies health officials’ advice against mask-wearing. One of us (Sandman) thinks it might have something to do with the fact that masks are part of the doctors’ professional equipment, not to be profaned by laypeople’s use. Lanard disagrees. Neither of us has any evidence for or against this hypothesis.
It’s got to be more fundamental than that, because it’s not just masks. Officials and experts tend to be contemptuous of any precaution the public comes to on its own, without (or especially against) the advice of the professionals. We suspect that there is a lot of ego at stake here – that the people whose job it is to tell us how best to protect ourselves simply do not take kindly to unseemly public displays of autonomy. And we suspect that the less confident they are about the knowledge base behind their precautionary recommendations, the more they feel a kind of projected contempt for people who make up their own minds about precautions.
Note that our evidentiary support for the previous paragraph is non-existent. We believe that ego, insecurity, and projection are probably behind health officials’ contempt for publicly chosen precautions on the same basis that we believe that covering your mouth and wearing a mask probably help reduce the spread of influenza.

-
What’s the risk communication angle – in particular, how does the availability of precautions affect people’s level of concern about a risk?
Health officials typically offer two contradictory explanations for opposing a precaution the public finds attractive.
- On the one hand, they say, hearing the precaution recommended or seeing others actually taking the precaution will scare people too much.
- On the other hand, they also say, hearing the precaution recommended or actually taking the precaution themselves will reassure people too much.
Both rationales are familiar with respect to surgical masks. They showed up during the SARS outbreaks and they are showing up again in debates over pandemic influenza preparedness.
- Mask-wearing will leave you too terrified to live your normal life.
- Mask-wearing will leave you too complacent to take the officially recommended precautions.
This two-barreled opposition is not unique to mask-wearing. During debates about distributing potassium iodide pills to people living near nuclear power plants, a June 13, 2002 New York Times editorial noted: “Nuclear advocates fret that making the pills available will exaggerate public fears, while nuclear critics worry that the pills will breed complacency about nuclear risks.”
Experts on both sides concede that the rapid use of potassium iodide could help to prevent thyroid cancer in people (especially children) exposed to certain kinds of radiation that might be released during a nuclear power plant accident or attack. And experts on both sides concede that the drug has to be taken quickly, too quickly to make after-the-fact distribution a practical option. Nonetheless, many experts oppose public distribution beforehand. People might get overanxious and take the pills prematurely. Or people might get overconfident and take the pills belatedly. Or, sometimes, both arguments from the same expert, who is certain only that there must be some good reason why control shouldn’t be handed over to mere patients.…
What does risk communication theory and research tell us about how the availability of precautions affects risk perception? In a nutshell, you would expect two effects, both of them desirable:
- People who are unaware of a risk or unconcerned about it become more aware and more concerned when they hear about precautions against that risk that others are recommending, considering, or taking. If you’re not into pandemic preparedness, hearing people talk about stockpiling surgical masks may pique your interest; seeing people walking around in surgical masks is likely to arouse some concern. Whether or not you end up a mask-stockpiler or a mask-wearer yourself, you probably end up more sensitized to the pandemic risk than you were.
- People who are very concerned about a risk become less afraid – or more able to bear their fear – when they hear about precautions they can consider taking. This effect is amplified if and when they decide to act. If you’re preoccupied with the risk of a pandemic, it helps you cope better emotionally if you know there are things you can do to protect yourself. Thinking about masks; choosing what sort of mask you need and how many to buy; actually buying your mask supply; learning how to use the mask properly – these are all activities that can help you stay calm … even as they help rouse your apathetic neighbor.
So if you think people ought to be really apathetic about a risk, you don’t want them hearing about precautions, deciding about precautions, or taking precautions. And if you think people ought to be really terrified, you don’t want them doing those things either. But if you want people to be concerned, maybe even fearful, but coping well and getting on with life, then precautions are invaluable.
In short, whether or not surgical masks help people protect themselves during a flu pandemic, surgical masks can help people establish and sustain the right frame of mind to confront a pandemic.
The communication “signal” sent by increasing public interest in stockpiling masks may also provoke local hospitals and other institutions (prisons, police, even retailers and taxi companies) to work on their own mask stockpiles. A predictable sign that these institutions are late to the game will be if they start to protest that public stockpiling is interfering with their ability to get the supplies they need.
This is all common sense (though there is research to support it). Though a memorable car crash may propel you to start wearing a seatbelt, most people put their seatbelts on without vividly imagining the crash. Though you may install smoke detectors after hearing about a horrific house fire, most people change the batteries in their smoke detectors, when the darn things start to beep, without vividly picturing their houses burning down. Precaution-taking becomes integrated into normal life. It reminds people that the risk is real, and simultaneously reminds them that they are addressing the risk sensibly – that they are neither apathetic nor powerless.
The self-efficacy that people feel when choosing which precautions to take and which to eschew helps them cope with their fears, and is thus a bulwark against panic or (more commonly) denial. That’s why offering people a menu of precautions is better risk communication than offering just one, and it’s why the precautions people come up with themselves are worth encouraging if at all possible. But none of that means that people who stockpile surgical masks (or Tamiflu) are less likely than non-stockpilers to wash their hands a lot. People who take one kind of precaution tend to take others as well. This is predictable from studies of cognitive dissonance, and demonstrable from studies of precaution-taking during the SARS outbreaks in Hong Kong and Singapore.
During the SARS outbreaks, four British public health doctors traveling in Thailand went through their own initially skeptical adjustment reaction to the sight of so many people using (and misusing) masks in public. Eventually, they reached this tentative conclusion: “The mask became a highly visible symbol of individual and collective determination to achieve control even though its value in community settings is questionable…. Perhaps it is this perception of the importance of personal and collective responsibility by members of the public that the mask symbolises best and the public health contribution of this symbolism should be remembered for future emerging infections.”
What’s a risk communicator to do? Keep pushing, internally as well as publicly, for straight thinking and straight talking. Especially straight thinking! There was a time when we imagined that companies and governments self-awarely misled their publics. We came to realize that mostly they mislead themselves first. That’s the main problem, we think, with Tamiflu policy and communication … and with mask policy and communication … and with lots of other areas of pandemic policy and communication. Risk communicators often need to help health officials and experts think straight before it’s possible to help them talk straight.
Kay responds:
So often I feel like I am shouting, “But the Emperor is not wearing any clothes!” and people (smart people!) just stare at me blindly. I start to wonder if maybe I’m the one who “just doesn’t get it.”
We’re beginning to get feedback from our local health departments on our draft pandemic plan and so many are saying “risk communication is our only weapon” or something to that effect.
Whoa, horse! There are some things we can’t risk communicate away. For example, if Tamiflu is the only drug that will improve your chance of surviving pandemic influenza, AND you have to start taking it within 36-48 hours for it to work, AND if the only way you can get Tamiflu is to be admitted to the hospital, I just can’t think of a message that will convince people to keep trying to get through to their doctor’s office rather than go to the emergency room if there’s a pandemic and they have developed flu-like symptoms.
Moreover, that message shouldn’t be given from an ethical perspective. It takes a day or more (if you’re lucky) to get a call back from a doctor now! So how dare we tell people to wait patiently when that wait might make the difference in whether they survive? Will there be an influx of “worried well” to hospitals? I’m not so sure about that because most people will have the sense to know that emergency rooms are where they’ll be at highest risk of exposure to the virus. But there sure will be a truckload of “worried sick” if policy effectively denies them any other option.
The strategy I keep pushing is to say right here right now: “We’ll do our best. Our best won’t be good enough. In a pandemic it is realistic to expect that there will be severe limits on availability of vaccine and antiviral medications and most people will not have access to these resources, at least for many months after a pandemic begins. This fact is unlikely to change, and you should consider it seriously in making your own pandemic preparations. These are preparations we think you should make, and here’s why.…”
Our actual approach is to be less blunt, but I did get the following language included in a letter to the business community: “It cannot be stressed strongly enough that in a severe pandemic, actions of individuals, businesses and community organizations, as much as those of government, will greatly determine the outcome.”
So I’ll keep pushing back until they get sick of me, and then I’ll push some more.
LOVE your columns (but then you knew that).
Pandemic risk and the U.S. poultry industry
| name: | Logan Boss | |
| Field: | PIO Northwest Georgia Public Health | |
| Date: | January 19, 2006 | |
| Email: | hlboss@gdph.state.ga.us | |
| Location: | Georgia, U.S. |
Comment:
Reference this opinion piece – Stuart Appelbaum, “Avian flu defense can enlist poultry workers” – in the 12/28/05 Atlanta Journal-Constitution.
I’m curious about your thoughts on this piece from both public-health and industrial-safety-and-hygiene perspectives, especially the statement that “it makes little sense to immediately vaccinate physicians who will treat infections and not poultry workers.” The piece appears to be a thinly veiled, although admirable, plea for poultry-worker rights, but seems to confuse some of the main issues with avian flu, particularly the notion that local birds are the key.
Thank you and your wife for maintaining this informative, useful site and Happy New Year!
Peter responds:
As you rightly point out, the author of this column is very confused – or trying to confuse others – about the role of the U.S. poultry industry in the risk of a flu pandemic, and about the role of U.S. poultry industry employees in preventing such a pandemic.
A flu pandemic is by definition a worldwide human epidemic. If a novel flu virus (like H5N1) jumps from a bird to a human, and then starts spreading easily from human to human, a pandemic will be a very likely outcome – no matter where it starts. It certainly could start in Georgia, but Georgians are just as vulnerable if it starts in Vietnam or Turkey. If and when a flock in Georgia is diagnosed with H5N1, the risk to poultry workers who have contact with that flock will go up substantially. If it spreads widely throughout Georgia, the risk to all Georgia poultry workers will go up substantially. But the risk to other Georgians will be only slightly higher than it was.
In other words, how close you are to the nearest H5N1-positive bird matters little – unless it’s very close indeed. What matters for those of us who don’t have intimate contact with sick or dead birds is whether a novel flu virus anywhere in the world starts spreading among humans.
The version of this confusion that I see all the time comes from industry spokespeople, as opposed to union spokespeople like Appelbaum. Industry flacks frequently assert (and even more frequently imply) that as long as U.S. poultry flocks are H5N1-free, U.S. citizens don’t need to worry about a pandemic. This is errant nonsense. It encourages Americans to feel safer than they ought to feel so far. And it sets Americans up to feel more endangered than they ought to feel if and when H5N1 reaches a U.S. flock – at which point the industry may belatedly realize the harm it has done itself.
I have watched this happen in country after country. The time to tell people that their risk doesn’t depend on whether the country’s bird population is H5N1-free is before the first H5N1-positive bird is found in that country … not after.
Appelbaum is on solid ground arguing that Georgia poultry workers should be watching out for signs of disease in their flocks, and should be reporting those signs promptly. I think U.S. poultry companies have a pretty good record of wanting to catch avian flu outbreaks early – but I’d be willing to hear an argument that workers need whistleblower protection just to make sure. And they’ll certainly need protective gear and maybe even prophylactic doses of Tamiflu if they find infected birds and need to cull the flock.
But all of that is only marginally related to pandemic risk. It’s a run-of-the-mill industrial hygiene issue. Appelbaum is dead wrong when he claims that Georgia’s poultry workers are in the front lines of the fight against a pandemic. Even if H5N1 comes to Georgia’s poultry, the risk of a pandemic won’t increase by much. And even if H5N1 never comes to Georgia’s poultry, Georgians still need to prepare for a possible pandemic – which will probably come, if it comes at all, via people, not birds. If that happens, healthcare workers, cops, morticians, power plant operators, truckers, and many others will have a priority claim to antivirals and vaccine (when there is a vaccine) so they can help keep society going. Poultry workers won’t make the cut.
This sort of confusion would be easier to clear up if we stopped using terms like “bird flu” and “avian influenza” for the feared human pandemic. At the moment, there is no pandemic, because there is no novel flu virus (that is, a flu virus that is new to people and to which people therefore have no natural resistance) that is capable of efficient human-to-human transmission. To launch a pandemic, a bird flu virus would need to “learn” to spread efficiently among humans, which requires either a mutation (the virus changes all by itself) or a reassortment (the virus mixes-and-matches genetic material with another flu virus). If and when that happens, the resulting pandemic strain of influenza will no longer be avian. It will make more sense to call it Vietnam Flu or Turkey Flu (or conceivably Georgia Flu) than “bird flu.” It will certainly be a human flu by then.
Family pandemic preparedness and family pandemic communication
| Name: | Nancy |
| Field: | Parent, volunteer |
| Date: | January 14, 2006 |
| Location: | New Hampshire, U.S. |
What I would add to this site:
I would like to see information on what concrete steps you and your wife think appropriately prepared families should be doing to get ready for a potential pandemic.
Comment:
In regards to what schools should be teaching children about avian flu preparedness, our school does an excellent job of emergency preparedness (shelter in place, fire drills, lockdowns, etc.). However, there has been nothing communicated about avian flu. I, frankly, don’t believe the administrators even understand the risk.
I have a 7-year-old and a 10-year-old. Both of them are more informed on world events than most adults they encounter in the course of a normal day. What I have noticed with regard to their reactions to avian flu news is that they actually are scared – because it can “come here” (unlike Katrina or the war in Iraq or even direct acts of terror given our remote, rural, non-strategic location).
I have taught my children about the stages of a pandemic, the geography of where the avian flu is now, what will happen if efficient h2h occurs, and what our family is doing to prepare. However, I have begun to tone down the information I share with them or that they have secondary access to (leaving NPR on in the car, for example), because I did see them getting over-stressed.
I answer their questions as they arise. If I feel like there is something they NEED to know, I tell them. Otherwise, I am regularly reinforcing a pro-handwashing, anti-nose-picking-eye-rubbing-nail-biting lifestyle in all our daily lives, and I’m leaving it at that – for now.
Peter responds:
The question of how to talk to children about pandemic risks (and other scary realities) comes up often. Please see two 2005 Guestbook entries: “Giving children frightening bird flu information” and “Risk communication for children.”
In my responses to these two earlier comments, I stressed that children are more resilient and fear-tolerant than we often suppose; that they cope better when their questions are answered candidly than when adults try to over-reassure them with bland generalizations; and that it helps if the family is taking appropriate precautions, not just sitting and waiting for disaster to strike.
But it doesn’t sound like you are over-protecting your children from knowledge about pandemics. You’ve taught them the basics, and you’ve given them some things they can to do to reduce their own risk. That sounds like enough for now. If the news gets bad and you think a pandemic may be imminent, you’ll want to talk with them some more. Until then, I’d take my cues from them, waiting to see if they bring it up.
Of course I’d like to see their school bring it up too – not so much for your kids’ sake as for the ones who haven’t heard much at home about pandemics. There are pros and cons to your pushing hard for a pandemic component in the school curriculum, and in the school system’s own emergency planning. It’s obviously a step forward for the school system to think through its pandemic preparedness plan, and for your community’s children to start getting emotionally ready. And there’s a long history (smoke detectors, radon testing, etc.) of parents learning about family safety from their children, who learned it at school. On the other hand, your own children may have objections to being known as the kids whose mom is obsessed with influenza.
My wife and colleague Jody Lanard collaborated on the rest of this answer, on what pandemic precautions you might consider taking.
The U.S. Department of Health and Human Services has recently released two good, basic checklists:
- “Pandemic Flu Planning Checklist for Individuals and Families”
- “Faith-Based & Community Organizations Pandemic Influenza Preparedness Checklist”

HHS is also planning to post a preparedness checklist for schools by March 1, at: http://pandemicflu.gov/plan/tab5.html.
One piece of advice that HHS isn’t giving: to try to get a stockpile of Tamiflu or Relenza, the two antiviral drugs that are likeliest to help in a pandemic. U.S. official policy is to recommend against personal stockpiling of antivirals. We think stockpiling is an ethical dilemma. What’s best for your family may not be what’s best for the country. See The Dilemma of Personal Tamiflu Stockpiling.
If you want to go beyond the HHS recommendations, the Flu Wiki has a page with links to a wide range of government and non-government pandemic preparedness guides. We haven’t read all of them.
We want to underscore one implication of the universal recommendation to stockpile food, water, and other basic necessities. It is important to do this now, before a pandemic actually begins. Otherwise, everyone will be trying to stockpile at the same moment of acute risk, and supplies will run out quickly.
We have lived most of our lives in the Atlantic hurricane and snowstorm belt. We’re used to the last-minute rush to the store for canned goods, bread, batteries, and candles. The desire to load up on necessities overtakes everyone at the same time, whenever a storm is forecast. For pandemic preparedness, people should front-load that impulse, and strike while the iron is cold. Shop now.
That’s true for storms too, of course, but pandemics are a lot bigger. Imagine all the world’s people deciding at roughly the same moment to stockpile everything they can think of to help maintain “social distance” by staying home, and to do so immediately before distribution networks are disrupted by the imminent pandemic. Preparedness will work a lot better if people gradually (but not too gradually) build up a “rolling stockpile” of basic necessities. Start right now, and keep using and replacing your pandemic supplies in a routine way. It is also important to help neighborhood and charitable organizations do the same thing, on behalf of those who cannot afford to buy or store large quantities of basic necessities, and on behalf of those who can, but don’t.
And by all means involve your children in this stockpiling effort.
The “outrage factors”
| Name: | Dick Traeger |
| Field: | Chem Engr – National Lab Research/Mngmt |
| Date: | January 14, 2006 |
| Location: | New Mexico, U.S. |
What I would add to this site:
A concise listing of responses to risks – Can I see it? Am I in control? Etc.
Comment:
A number of years ago I heard your presentation on the perception of risk at a national chem engr meeting. The room was packed and the talk mesmerizing – no one sneezed. Since then I have been trying to find out where you were to get a copy of your perception of risk list. Finally picked up this web site from Freakonomics.
I have nothing to say other than that your analysis is most useful in all current technologies. One example: The fear of groundwater contamination blows away all rational thought – impacts all energy and waste development.
Thanks for your insights – they are needed.
Peter responds:
Thank you for your kind words. I’m glad you found the website.
My list of the top twelve “outrage factors” is in one of my seminar handouts ![]() , and at the bottom of the handout are several links to articles with more detailed descriptions of the factors. But here is the list:
, and at the bottom of the handout are several links to articles with more detailed descriptions of the factors. But here is the list:
| Twelve Principal Outrage Components | ||
|---|---|---|
| Safe | Risky | |
| 1. | Voluntary | Coerced |
| 2. | Natural | Industrial |
| 3. | Familiar | Exotic |
| 4. | Not memorable | Memorable |
| 5. | Not dreaded | Dreaded |
| 6. | Chronic | Catastrophic |
| 7. | Knowable | Unknowable |
| 8. | Individually controlled | Controlled by others |
| 9. | Fair | Unfair |
| 10. | Morally irrelevant | Morally relevant |
| 11. | Trustworthy sources | Untrustworthy sources |
| 12. | Responsive process | Unresponsive process |
I have another list of eight “secondary” factors that I use much less often, and that isn’t anywhere on the website till now:
| 13. | Effect on vulnerable populations |
| 14. | Delayed vs. immediate effects |
| 15. | Effect on future generations |
| 16. | Identifiability of the victim |
| 17. | Elimination vs. reduction |
| 18. | Risk-benefit ratio |
| 19. | Media attention |
| 20. | Opportunity for collective action |
Note that there are lots of other lists – some longer, some shorter, all overlapping. Several of the factors on my list are actually collections of subfactors. (For example, your “Can I see it?” – detectability – is part of knowability, #7.)
Note also that “my” list is based more on research by Paul Slovic, Baruch Fischhoff, and Sarah Lichtenstein than on anything of my own.
Finally, note that most of the research along these lines (it’s called the “psychometric paradigm”) has moved away from long lists of conceptual “factors” to a much shorter list of two statistical factors that account for most of the variance. The two factors are usually labeled “dread risk” and “unknown risk” – but they are much broader than my #5 and #7. For a recent article that reviews the psychometric approach and applies it to catastrophic risks, see Paul Slovic and Elke Weber, “Perception of Risk Posed by Extreme Events.” ![]()
I continue to find longer lists of outrage factors useful to remind my clients (and myself) that predicting how upset people will be about a risk is mostly a matter of assessing the risk according to these factors – and that getting people more or less upset is mostly a matter of managing one or more of these factors upward or downward. That’s not all there is to outrage management. (See my Outrage Management Index for more.) But it’s a good place to start.
Copyright © 2006 by Peter M. Sandman
